This is an alternative health website, and to be sure, over the years, I’ve tweaked medical doctors in my newsletters and blogs. But truth be told, and as I have said many times before, unlike many in the alternative health community, I’m a huge fan of doctors — not so much the medical organizations that represent them — but the doctors themselves. Yes, there are doctors who are incompetent or unethical, but for the most part, the overwhelming majority of medical doctors I have met in my life are extremely competent, highly dedicated, and often even heroic. And make no mistake, no matter how into alternative health you are, there are times you absolutely need a doctor. If your name is John Wayne Bobbitt, you need a doctor, not an herbalist.
Now for any Millennials reading this newsletter, John Wayne Bobbitt was frontpage news–and a medical miracle–a quarter of a century ago. One night, after he had gone to sleep, his wife, Lorena, in revenge for him allegedly forcing himself on her earlier that evening (a charge he was acquitted of in a subsequent trial), grabbed a knife from the kitchen, entered their bedroom, and removed her husband’s penis at its base.[1] She then left the apartment with the severed member and drove away in her car, tossing it into a field. After realizing the severity of her crime, she stopped and called 9-1-1. John Wayne’s penis was found after an exhaustive search, and it was reattached in the hospital where he was treated. Now, although it never regained full sensation, his re-attached penis functioned well enough that John Wayne was able to pursue a brief career starring in a couple of adult films.
So, for any of you Millennials who think nothing interesting ever happened before you were born, you can consider yourself corrected. But more to point, this is something an alternative healer could not have done. Or to put it another way, no matter how much you rely on alternative health, there are times only a medical doctor will do.
That said, when it comes to most catastrophic illnesses, medical doctors are clueless. They merely manage symptoms and push test numbers up and down. And when it comes to health and nutrition, for the most part, things are even worse; doctors are often arrogantly ignorant. On average, the typical doctor spends a total of 6-8 hours in their entire medical career studying health and nutrition — and yet they feel free to dogmatically pronounce on all aspects of diet and supplementation with less knowledge than any lay person who has read two good books on the subject has. For shame!
In the developed world, we have grown up trusting our doctors. They are frequently the heroes on our favorite TV shows, and we have largely turned over to them complete responsibility for our health. And yes, modern medical science has made incredible advances and contributions which have alleviated much pain and suffering. Surgical technique (the cutting apart and repairing of the human body ala John Wayne Bobbitt) has made remarkable progress. Identification of germs that cause disease and improved sanitation, which aids in preventing that disease, have also seen epic achievements. Burn treatment, trauma, and emergency room care are nothing less than miraculous. When it comes to these areas of medicine, the value doctors bring to us is impossible to measure.
With this background in mind, it seemed a good time to once again give a tip of the hat to some of medicine’s most recent breakthroughs–treatments and procedures that go where no alternative healer can go.
Prosthetic Innovation

If you lose a limb, it ain’t growing back, no matter how many vitamins you take. For millennia, the only option was a prosthetic. Think Captain Hook. Originally made from iron, steel, copper, and wood, they had basic functionality and minimal cosmetic appeal. Over time, both functionality and cosmetics approved so that you could pick things up with a prosthetic hand or walk with a bending prosthetic knee, all covered in flesh colored plastic.
More recently, new materials such as carbon fiber and advances in computer miniaturization have come into play allowing for some major innovations just now appearing.
Making Quality Prosthetics Affordable for Everyone
So far, high-tech prosthetics have been extremely expensive and only available to amputees in first world countries–totally out of reach for most of the world’s amputees, many of whom are children.
Open Bionics, a UK-based start-up tech company, has developed the ability to produce remarkable 3D printed prosthetics that are 1/30 the cost of standard prosthetics.1 http://openbionics.com/
And make no mistake, these are not old-style, do-nothing, prosthetics. They operate using sensors attached to the skin that detect muscle movements. The muscle movements control the hand and open and close fingers. And each prosthesis is custom designed for its individual user. The person’s limb is scanned with a tablet computer, which is inexpensive to do. The design of the prosthetic is then planned out using preprogrammed computer models, again inexpensive. A 3-D printer then produces the custom arm in about 40 hours, again inexpensive.
And as if cutting-edge bionic arms weren’t cool enough, Open Bionics is working with Disney to develop a range of royalty-free Hero Arm covers from the Star Wars, Marvel and Frozen universes. The goal is to make kids feel proud of their prostheses. This changes the image of prostheses from medical devices to bionic arms inspired by beloved characters.
The Hero Arm is now available for people in the UK with below elbow upper-limb differences, aged eight and above. But ultimately, Open Bionics’ goal/mission is to make “beautiful bionic limbs” more available.
Prosthetics with Movement Sensation
Almost 10 years ago, we talked about the mind controlled “Luke arm,” named after Luke Skywalker that allowed users to control it with their brains, thus duplicating “almost” everything a real arm could do. Nevertheless, it came up short in one very important way: it had no sense of touch. Now, scientists are on the verge of developing a way for users to intuitively “feel” their prosthetics, allowing them to manipulate objects blindly.2 Paul D. Marasco1, Jacqueline S. Hebert, Jon W. Sensinger, et al. “Illusory movement perception improves motor control for prosthetic hands.” Science Translational Medicine 14 Mar 2018: Vol. 10, Issue 432, eaao6990. http://stm.sciencemag.org/content/10/432/eaao6990 The work, which was published in the journal Science Translational Medicine, is a huge step towards making artificial limbs feel just as natural as the real deal.
The ability to sense the spatial position and movements of one’s own body (kinesthetic sense) is critical for limb use. To effortlessly complete an intentional movement, the brain needs feedback from the body regarding the movement’s progress. This largely nonconscious kinesthetic sense helps the brain to learn relationships between motor commands and outcomes to correct movement errors. And this skill, of course, is something that prosthetics had difficulty replicating. Prosthetic systems for restoring function have predominantly focused on controlling motorized joint movement. Without the kinesthetic sense, however, these devices do not become intuitively controllable. By vibrating the muscles used for prosthetic control via a neural-machine interface, the researchers were able to produce the illusory perception of complex grip movements. Within minutes, three amputees who tested the arms integrated this kinesthetic feedback and improved movement control. It quickly became clear that the artificial “feeling” feedback was immensely helpful, and the researchers note that it enhanced the subjects’ ability to use their prosthetic without looking directly at it. Even when their artificial limb was in sight, the patients exhibited more accurate and precise movement. This feedback approach for closed-loop control opens a pathway to seamless integration of mind and machine.
More Prosthetic Innovations
Check out:
Cancer Vaccine
For almost a quarter of a century (boy, time sure flies), I’ve been saying that cancer is fundamentally a disease of the immune system. Yes, it’s triggered by mutations in your DNA that cause cells to go rogue and become cancerous, but under normal circumstances, your immune system will identify each and every one of those rogue cells and eliminate them from your body before they ever take root and multiply. You “get” cancer, not from individual rogue cells but when your immune system fails in its job and allows those cells to take over. That’s why, for decades, I’ve said that the most exciting research in cancer involved using your own immune system to fight cancer.
Human trials of a cancer “vaccine” that promises to eliminate 97% of all tumors are expected to start before the end of the year.
Over the last several years, different forms of cancer immunotherapy have been developed and tested. Some target naturally occurring checkpoints that limit the anti-cancer activity of immune cells. Others, like CAR T-cell therapy have proven very successful in treating some types of leukemia and lymphomas but have been less effective in dealing with solid tumors. In addition, they require a patient’s immune cells to be removed from the body and genetically engineered to attack the tumor cells.3 Shum T, Kruse RL, Rooney CM. “Strategies for enhancing adoptive T-cell immunotherapy against solid tumors using engineered cytokine signaling and other modalities.” Expert Opin Biol Ther. 2018 May 4. http://www.ncbi.nlm.nih.gov/pubmed/29727246 , 4 ERIC BOCK. “CAR T-Cell Therapy Moves Closer to FDA Approval.” NIH Record. Vol. LXVIII, No. 24. (Accessed 12 May 2018.) http://nihrecord.nih.gov/newsletters/2016/11_18_2016/story1.htm Now, to be sure, a number of these approaches have been successful, but they each have downsides — from difficult-to-handle side effects to high-cost and lengthy preparation or treatment times.
Well, human trials of a cancer “vaccine” that promises to avoid all these problems, and that has already been found to have eliminated tumors in nearly all treated mice, are expected to start before the end of the year. Researchers at Stanford University’s School of Medicine published a study earlier this year in the academic journal Science Translational Medicine that reported on a developed strategy to treat cancer through a new form of immunotherapy that uses the body’s immune system–as nature intended–to fight existing cancers.5 Idit Sagiv-Barfi, Debra K. Czerwinski, Ronald Levy, et al. “Eradication of spontaneous malignancy by local immunotherapy.” Science Translational Medicine, 2018; 10 (426): eaan4488. http://stm.sciencemag.org/content/10/426/eaan4488 Researchers injected small amounts of two immune-stimulating agents directly into solid tumors in about 90 mice. The technique wiped out cancerous cells in 87 of the mice, including distant, untreated metastases. And the study found that the approach seems to work for many different types of cancers, including those that arise spontaneously.
What is unique about this method is that it works to reactivate the body’s cancer-specific T-cells by injecting mere millionths of a gram of the two agents directly into the tumor site. One, a short stretch of DNA called a CpG oligonucleotide, works with other nearby immune cells to amplify the expression of an activating receptor called OX40 on the surface of the T-cells. The other agent, an antibody that binds to OX40, activates the T-cells to take on the specific cancer cells around it. Because the two agents are injected directly into the tumor, only T-cells that have infiltrated the tumor are activated. In effect, these T-cells are “prescreened” by the body to recognize only the cancer-specific proteins found in that tumor–and work only inside that tumor. The results, at least in the mice, are rapid, relatively inexpensive to accomplish, and do not produce the adverse side effects often seen with body-wide immune stimulation.
This is a very targeted approach. Only the tumor that shares the protein targets displayed by the treated site is affected. This approach attacks specific targets without having to identify exactly what proteins the T-cells are recognizing. And then, as a bonus, and almost miraculously, some of these tumor-specific, activated T-cells then leave the original tumor to seek out and destroy other identical tumors wherever they may exist throughout the body.
“When we use these two agents together, we see the elimination of tumors all over the body,” said Ronald Levy, MD, professor of oncology and lead researcher. “This approach bypasses the need to identify tumor-specific immune targets and doesn’t require wholesale activation of the immune system or customization of a patient’s immune cells.”
Multiple Sclerosis
MS is an autoimmune disease in which the body’s immune system attacks myelin, a key substance that serves as a nerve insulator and helps in the transmission of nerve signals. From a medical standpoint, what we understand about multiple sclerosis is mostly hunches and guesswork. Nevertheless, it does appear that MS (as with most idiopathic autoimmune disorders) is the result of an overall system imbalance triggered by things within our ability to alter, and that the final causative factor in the chain of events is inflammation. It is a nasty disease with few good medical options. As I have discussed previously, there are alternative options that can help your body role back many of the symptoms–if not necessarily the disease itself. What follows is a discussion about a new medical treatment that may offer an alternative for those who choose to stick with the medical option when the standard pharmaceutical prescriptions are not working.
A randomized clinical trial with 110 patients who’d been diagnosed with relapsing-remitting multiple sclerosis found that people with multiple sclerosis may be able to “reset” their immune system and potentially reverse their symptoms with a transplanted infusion of blood-based stem cells. That is: stem cells from the patients’ own blood is collected 10 days after they started a drug regimen and then reinjected into their bloodstream. Specifically, the treatment involves using cancer drugs to decimate a patient’s immune system and then restarting it with a stem cell transplant. Obviously, then, this is not a first-choice treatment but a treatment of last resort.
The study built on earlier work by Dr. Richard Burt, a stem cell specialist at Northwestern University’s Feinberg School of Medicine that focused on immune cells as a treatment for MS.6 http://ebmt2018.abstractmgmt.com/uploads/15-presentation.pdf The researchers’ objective was to see if they could stop “the immune attack on the brain” VS standard drug treatment as prescribed by a neurologist. MS patients are typically treated with immunosuppressants like interferon. But these treatments often have harsh side effects, including an increased vulnerability to infections. And the drugs can be expensive; as of 2018, the median cost for a year’s supply of MS drugs is $80,000.
The main goal of the trial was to see whether the transplant worsened neurological symptoms. Well, according to the abstract of Burt’s presentation, about 60 percent of the patients who received standard drug therapy experienced a decline as measured by neurologists on standardized scales; by comparison, only six percent of patients who received the transplant therapy progressed similarly.7 Richard K Burt, Roumen Balabanov, John A Snowden, et al. “NON-MYELOABLATIVE HAEMATOPOIETIC STEM CELL TRANSPLANTATION VERSUS CONTINUED DISEASE MODIFYING THERAPIES (DMT) IN PATIENTS WITH HIGHLY ACTIVE RELAPSING REMITTING MULTIPLE SCLEROSIS (RRMS). EBMT, Annual Meeting. 17 March 2018. http://www.professionalabstracts.com/ebmt2018/iplanner/#/presentation/636
Stem cell treatments can have serious side effects, as does standard drug treatment. But as Burt told BBC news, “The data is stunningly in favor of transplant against the best available drugs — the neurological community has so far been skeptical about this treatment, but these results will likely change that.”8 “Stem Cell Transplant for MS Shows Promise.” WebMD. March 19, 2018. (Accessed 8 May 2018.) http://www.webmd.com/multiple-sclerosis/news/20180319/stem-cell-transplant-for-ms-shows-promise The bottom line is that this new treatment offers hope for those unwilling to do the work involved in utilizing an alternative health protocol or for whom standard drug treatments don’t work.
Stem Cell Therapy for Macular Degeneration
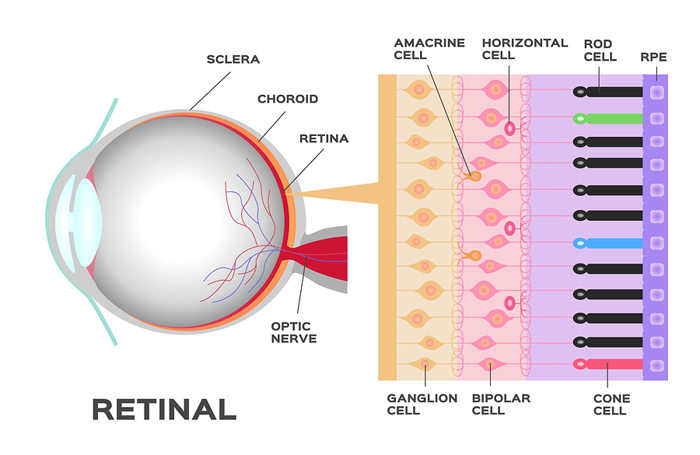
The macula is an oval-shaped pigmented area near the center of the retina of the human eye. It is responsible for the central, high-resolution, color vision that is possible in good light. This kind of vision is impaired if the macula is damaged, such as by the progressive destruction caused by age-related macular degeneration (AMD). AMD is a major cause of blindness, with dysfunction and loss of retinal pigment epithelium (RPE) tissue central to the progression of the disease. Until now, there was little medical science could do to help, but that may be changing.
According to a study published in Nature Biotechnology, researchers were able to engineer a “living” RPE patch comprised of human stem cells on a coated, synthetic basement membrane.9 da Cruz, Lyndon; Fynes, Kate; Georgiadis, Odysseas; et al. “Phase 1 clinical study of an embryonic stem cell-derived retinal pigment epithelium patch in age-related macular degeneration.” Nature Biotechnology 2018 V36 P328. http://www.nature.com/articles/nbt.4114 The patch is only one layer of cells thick – about 40 microns – and 6mm long and 4mm wide. For the study, the patch was successfully inserted underneath the rods and cones in the back of one eye in each of two patients with severe exudative (wet) AMD. The patch was not only successfully inserted, but it also survived and converted into the type of cells that make up the retinal pigment epithelium. The result is that visual acuity improved over the next 12 months. And only local immunosuppression was required long-term.
Douglas Waters, 86, and one of the two patients involved in the study, could not see out of his right eye before the procedure. “Couldn’t see anything,” he told the BBC. “I can now read the newspaper” with it. “In the months before the operation my sight was really poor, and I couldn’t see anything out of my right eye. It’s brilliant what the team have done, and I feel so lucky to have been given my sight back.”10 James Gallagher. “Macular degeneration: ‘I’ve been given my sight back.'” BBC. 19 March 2018. (Accessed 9 May 2018.) http://www.bbc.com/news/health-43458365
So far, the two patients (the other is a woman in her early sixties) have maintained improved vision in the treated eye for a year. They went from not being able to read with their affected eye at all, to reading 60 to 80 words per minute.
As you get older, parts of you stop working, and for the first time researchers have been able to turn a stem cell into a specific part of the eye that’s failing and put it back in the eye and get vision back.
Prof Lyndon da Cruz, consultant retinal surgeon at Moorfields and one of the researchers involved in the study, told the BBC: “We’ve restored vision where there was none. It’s incredibly exciting. As you get older, parts of you stop working, and for the first time we’ve been able to take a cell and make it into a specific part of the eye that’s failing and put it back in the eye and get vision back.” However, he does not call this a “cure” as completely normal vision is not restored. But going from blind to being able to read is astonishing enough.
Miscellaneous Miracles
In truth, far beyond what we’ve discussed above, there are many, many advancements being made in and around the field of medicine. Let’s briefly touch on a few more.
Robotic surgery
Most of us have seen medical dramas on TV that make use of robotic surgical tools that make possible minimally invasive surgeries on the most delicate elements of the human anatomy. But beyond whatever you may have already seen, the capabilities of that technology are about to explode.
3-D Visualization and Augmented Reality for Surgery
Augmented reality is a recent technology for executing detailed surgical operations that is similar to VR. It combines 3-dimensional (3-D) computer-generated objects and text superimposed onto real images and video, all in real time. The main difference between VR and AR is that the former uses generated images, the latter uses real images, video frames, and 3-D graphics.11 SL Tang, CK Kwoh, MY Teo, NW Sing. “Augmented reality systems for medical applications.” IEEE Eng Med Biol Mag. 1998;17 ((3)) 49- 58. http://ieeexplore.ieee.org/abstract/document/677169/ The ability to quantify and manipulate spatial information–to relate one set of data to another (registration)–is fundamental to surgical navigation. And now, in the last year, surgeons have begun experimenting with the next generation of AR surgery that allows them to immerse themselves in hi-res, 3-D representations of their subject. It has already been used in several hospitals in neurosurgery, cosmetic surgery, and retinal microsurgery.
Those surgeons who have used this technology are beyond enthusiastic.
Artificial Intelligence
And then there’s artificial intelligence. IBM Watson has demonstrated the ability to not only diagnose potential medical problems, but also predict outcomes such as future heart attacks and death, as well as design custom patient protocols. But even better, Watson can cross reference the massive amount of individual patient data it has gathered and stored in the cloud and thereby predict disease outbreaks around the globe–before any human could recognize the pattern/problem.
Gene Editing
Yes, alternative approaches including diet and supplements can protect your DNA from damage and can even alter the ability of damaged genes from expressing themselves and manifesting illness. But truth be told, there is little evidence that any tools in the alternative arsenal can repair damaged or faulty DNA. (Check out Everything You Need to Know About Epigenetics.)
Now, however, this option may fall within the realm of human possibility–and in a profound and wide-ranging way. What we’re talking about may very well represent one of the most significant advances in the history of modern medicine. The revolutionary CRISPR/Cas-9 gene-editing technology is about to change medicine in ways that were previously unimaginable. Gene editing is about to go mainstream. This will certainly alter how we treat cancer, for example–by simply “editing” any cancer cells in your body out of existence.12 Dom Galeon. “The First American CRISPR Trial in Humans Will Target Cancer.” Futurism. January 18, 2018. (Accessed 13 May 2018.) http://futurism.com/first-american-human-crispr-trial-target-cancer/ It also could be used to protect against other scourges such as sickle cell anemia and Alzheimer’s and Parkinson’s disease once their genetic components are clearly identified. And it could be used to eliminate a whole host of viral diseases that are currently unassailable since they hide within the body’s cells, coopting their DNA. We’re talking HIV, herpes, and shingles, for example.13 Martyn K. White, Wenhui Hu, and Kamel Khalili. “The CRISPR/Cas9 genome editing methodology as a weapon against human viruses.” Discov Med. 2015 Apr; 19(105): 255–262. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4445958/
Are there ethical concerns related to gene manipulation? Absolutely, especially considering human history. But make no mistake: gene editing is inevitable. Stopping it is not an option, so we better learn to control how and when it’s applied to make sure it’s used to help eliminate disease–not to build a genetically superior master race or build human/animal body part supply factories. In other words, we better learn to own it before it owns us. But that said, it’s potential for reversing and preventing many horrible diseases is astounding.
Conclusion
As I’ve said many times, it is easy to see that modern medical science has indeed made incredible advances and contributions which have alleviated much pain and suffering–and will likely continue to do so as humanity stumbles into the future. However, in our exploration, we have seen glimpses of medicine’s darker side–chinks in the armor of its accomplishments if you will. For now, though, for this one issue of the newsletter, let’s give medicine its due and leave on a high note. Congratulations to doctors and all they have accomplished!
References
| ↑1 | http://openbionics.com/ |
|---|---|
| ↑2 | Paul D. Marasco1, Jacqueline S. Hebert, Jon W. Sensinger, et al. “Illusory movement perception improves motor control for prosthetic hands.” Science Translational Medicine 14 Mar 2018: Vol. 10, Issue 432, eaao6990. http://stm.sciencemag.org/content/10/432/eaao6990 |
| ↑3 | Shum T, Kruse RL, Rooney CM. “Strategies for enhancing adoptive T-cell immunotherapy against solid tumors using engineered cytokine signaling and other modalities.” Expert Opin Biol Ther. 2018 May 4. http://www.ncbi.nlm.nih.gov/pubmed/29727246 |
| ↑4 | ERIC BOCK. “CAR T-Cell Therapy Moves Closer to FDA Approval.” NIH Record. Vol. LXVIII, No. 24. (Accessed 12 May 2018.) http://nihrecord.nih.gov/newsletters/2016/11_18_2016/story1.htm |
| ↑5 | Idit Sagiv-Barfi, Debra K. Czerwinski, Ronald Levy, et al. “Eradication of spontaneous malignancy by local immunotherapy.” Science Translational Medicine, 2018; 10 (426): eaan4488. http://stm.sciencemag.org/content/10/426/eaan4488 |
| ↑6 | http://ebmt2018.abstractmgmt.com/uploads/15-presentation.pdf |
| ↑7 | Richard K Burt, Roumen Balabanov, John A Snowden, et al. “NON-MYELOABLATIVE HAEMATOPOIETIC STEM CELL TRANSPLANTATION VERSUS CONTINUED DISEASE MODIFYING THERAPIES (DMT) IN PATIENTS WITH HIGHLY ACTIVE RELAPSING REMITTING MULTIPLE SCLEROSIS (RRMS). EBMT, Annual Meeting. 17 March 2018. http://www.professionalabstracts.com/ebmt2018/iplanner/#/presentation/636 |
| ↑8 | “Stem Cell Transplant for MS Shows Promise.” WebMD. March 19, 2018. (Accessed 8 May 2018.) http://www.webmd.com/multiple-sclerosis/news/20180319/stem-cell-transplant-for-ms-shows-promise |
| ↑9 | da Cruz, Lyndon; Fynes, Kate; Georgiadis, Odysseas; et al. “Phase 1 clinical study of an embryonic stem cell-derived retinal pigment epithelium patch in age-related macular degeneration.” Nature Biotechnology 2018 V36 P328. http://www.nature.com/articles/nbt.4114 |
| ↑10 | James Gallagher. “Macular degeneration: ‘I’ve been given my sight back.'” BBC. 19 March 2018. (Accessed 9 May 2018.) http://www.bbc.com/news/health-43458365 |
| ↑11 | SL Tang, CK Kwoh, MY Teo, NW Sing. “Augmented reality systems for medical applications.” IEEE Eng Med Biol Mag. 1998;17 ((3)) 49- 58. http://ieeexplore.ieee.org/abstract/document/677169/ |
| ↑12 | Dom Galeon. “The First American CRISPR Trial in Humans Will Target Cancer.” Futurism. January 18, 2018. (Accessed 13 May 2018.) http://futurism.com/first-american-human-crispr-trial-target-cancer/ |
| ↑13 | Martyn K. White, Wenhui Hu, and Kamel Khalili. “The CRISPR/Cas9 genome editing methodology as a weapon against human viruses.” Discov Med. 2015 Apr; 19(105): 255–262. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4445958/ |