In this issue, we discuss the physiology, or functioning, of the respiratory system, what can go wrong with those functions, and what natural alternatives exist to correct them.
In our last newsletter, we explored the anatomy of the respiratory system — its structures and patterns. In this issue, we continue with Part 2 of the series by discussing the physiology, or functioning, of the respiratory system. This is crucial, since once we understand the parts of the system and how they work, we can explore those things that can go wrong with those functions…and what natural health alternatives exist to correct them.
Four areas of respiration
Any discussion of the function of the respiratory system has to begin by breaking that function down into its four component parts, or areas. I’m not talking about inhalation and exhalation (or expiration as doctors refer to it) here, but rather the four distinct areas in which the act of respiration takes place in the human body. These are
- Pulmonary ventilation
- External pulmonary respiration
- Internal tissue respiration
- Cellular respiration
1. Pulmonary ventilation
To a large degree, we covered this in our last newsletter as part of our discussion of the anatomy of respiration. But now, given a different context, let’s reexamine this area of respiration. In pulmonary ventilation, outside air (aka room air) is taken into the body. This occurs through both the nose and mouth, which provides redundancy. If the nose is plugged, we breathe through our mouth, for example. In addition, this dual channel provides emergency capacity for stress situations such as when running — we breathe through both the mouth and nose. Room air is composed of 80% nitrogen, 20% oxygen, and trace gases including water vapor, argon, and carbon dioxide, plus very small amounts of other gases. It should probably be noted that the oxygen content of the air in early prehistoric times was probably around 35% — as proven by analyzing air bubbles trapped in fossilized amber. Nowadays, as I just mentioned, the average oxygen content of air is about 20-21%. However, in some industrial cities with heavy air pollution, the oxygen content may actually run as low as 17%. As a side note, at 15%, life as we know it might conceivably cease to exist. Something to think about…or not. At the very least, it’s one more reason to make every attempt to maximise your oxygen intake.
For the most part, this area of respiration is mechanical. Things that can go wrong include, drowning, choking, strangulation, or lack of oxygen in the air — things mostly outside the scope of alternative therapies and nutrition.
2. External pulmonary respiration
External pulmonary respiration involves the exchange of gases within your lungs — or more specifically the exchange of gases between the tiny sacs, the alveoli, in your lungs and the blood in your pulmonary capillaries. (This is the primary focus of this newsletter, and we will discuss it in some detail in a moment.)
3. Internal (blood) respiration
Here we’re talking about the exchange of gases between the cells in your body and blood in your systemic capillaries. Other than where it takes place, the process is virtually identical to that seen in external pulmonary respiration.
4. Cellular respiration
Cellular respiration involves metabolic processes within the cell. (We will discuss this in a future newsletter that explores cellular biology.)
Movement of gases
As mentioned above, the focus of this newsletter is on the movement of gases in external pulmonary respiration. When we refer to the movement of gases in respiration, we are talking about the exchange of gases in the lungs — moving carbon dioxide out of the body and oxygen in. In principle, this is remarkably simple and ultimately can be summarized in two words: Boyle’s Law. The trick is in getting to that point.
But first, let’s take a look at Boyle’s Law to see where we’re going. Boyle’s Law states that for a fixed amount of an ideal gas kept at a fixed temperature, pressure and volume are inversely proportional (while one increases, the other decreases). Or to phrase it another way, gases flow from an area of high pressure or concentration to an area of low pressure or concentration. Now let’s go into the slightly more complicated discussion of how that applies to respiration.
External Pulmonary Respiration
When the mouth and nose are open, the air pressure in the lungs equals the atmospheric pressure in the surrounding environment. The pressure of the space between the visceral and parietal pleura (the sacs that surround the lungs) is only slightly less than the atmospheric pressure — which keeps them pressed against each other.
When you take in a breath (inspiration), it contracts the diaphragm and increases the diameter of the thoracic cavity, decreasing the pressure between the lung and parietal pleura. In addition, the ribs are lifted up, further increasing the size of the thoracic cavity — thus lowering the pressure even more. When needed, as when running or exerting yourself, additional muscles such as the external intercostals, the scalenes, and the external oblique abdominals can help pull up the ribs even further providing for an even larger cavity — and even lowered pressure.
It is the lowering of pressure in the pleura space that draws air into the lungs. A “nature abhors a vacuum” kind of thing. Or to put it another way, air rushes into the lungs to fill the empty space and equalize the pressure.
On expiration, relaxation of the diaphragm causes it to return to its position higher up in the chest cavity, shrinking the size of the cavity, thereby increasing the pressure in the plural space, which expels air from the lungs. And as with inhalation, when needed, other muscles come into play. For example, the internal intercostals and the rectus abdominis muscles (aka the six pack) can help more forcefully shrink the size of the chest cavity, thereby moving air out more completely.
In addition, expansion and contraction of the flexible ribs and the chest can aid in inspiration and expiration.
As we’ve already mentioned, the accessory muscles of respiration aid in times of pulmonary stress such as during exercise or high stress. Specifically, we’re talking about:
- The external intercostal muscles, which connect the ribs and the collarbone and which pull the ribs up during respiration
- The sternocleidomastoid muscle, which helps raise the first rib, sternum, and collarbone up by pulling against the head
- The scalene muscles, which also pull the ribs up against the collarbone
- The rectus abdominis and internal intercostal muscles, which pull the ribs down, collapsing the chest cavity and aiding in expiration
Alveolar capillary air exchange
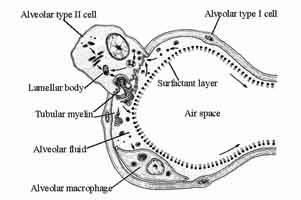
Once fresh room air has been drawn into the lungs, the exchange of gasses in the alveoli must take place. Each alveolus is lined by a handful of alveolar epithelial cells — similar to the epithelial cells that line the inside of your mouth and throat. Alveolar epithelial cells are very thin, and as it turns out, the thinnest part of that alveolus cell (the part that does not contain the cell nucleus) rests against the thinnest part of the pulmonary capillary wall — thus facilitating the diffusion of gas between the capillary and the alveolus. CO2 diffuses out of the blood, across the wall of the pulmonary capillary and then across the alveolus cell wall and into the lung. Likewise, O2 diffuses in the opposite direction to oxygenate the blood. This is the alveolar-capillary exchange, or pulmonary respiration.
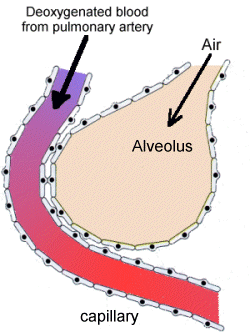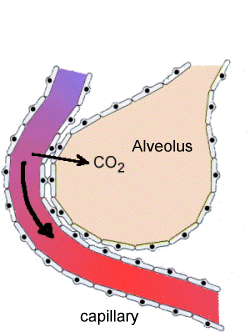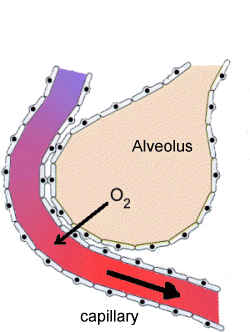 As I’ve already described, pulmonary respiration involves an exchange of gases, swapping oxygen in the alveoli for CO2 in the blood circulating through the pulmonary capillaries and vice versa. Which brings us back to Boyle’s Law. The movement of this exchange is dictated by Boyle’s Law of Gases, which says that gases move from areas of high pressure or concentration to areas of low pressure or concentration. Because the partial pressure or concentration of oxygen is higher in the lungs than in the capillaries, oxygen pushes into the capillaries and is captured by hemoglobin in the blood. Likewise, because the partial pressure or concentration of carbon dioxide is higher in the capillaries than in the lungs, carbon dioxide pushes in the opposite direction through the walls of the pulmonary capillaries and alveoli and into the lungs. That’s Boyle’s Law.
As I’ve already described, pulmonary respiration involves an exchange of gases, swapping oxygen in the alveoli for CO2 in the blood circulating through the pulmonary capillaries and vice versa. Which brings us back to Boyle’s Law. The movement of this exchange is dictated by Boyle’s Law of Gases, which says that gases move from areas of high pressure or concentration to areas of low pressure or concentration. Because the partial pressure or concentration of oxygen is higher in the lungs than in the capillaries, oxygen pushes into the capillaries and is captured by hemoglobin in the blood. Likewise, because the partial pressure or concentration of carbon dioxide is higher in the capillaries than in the lungs, carbon dioxide pushes in the opposite direction through the walls of the pulmonary capillaries and alveoli and into the lungs. That’s Boyle’s Law.
It should also be noted that carbon dioxide additionally comes from the buffer system in the blood plasma (not only from red cells) that rids the body of excess acid. We talked about this in the last newsletter. It’s called the bicarbonate system. The bicarbonate system allows you to add large numbers of CO2 or O2 molecules to the blood without affecting the acidity or alkalinity of the blood to any significant extent. In effect, the bicarbonate system serves as your body’s pH buffer system. This is necessary because any change in blood pH beyond 1/10 of a point is potentially lethal. Incidentally, the bicarbonate buffer system also is in play, but to a lesser extent, in body tissue itself. This is why changes in acidity show up in body tissue before they show up in the blood.
Things that can go wrong with respiration
For the most part, unless we’re talking about disease states (which we’ll do in the next issue of the newsletter), problems that can arise at the physiological level of the respiratory system are mostly mechanical.
Suffocation and obstructions
For example, pulmonary suffocation can result from the closure of the nose and mouth or throat by a foreign body — resulting in strangulation. Alveolar suffocation, on the other hand, results from water in the alveoli of the lungs preventing the exchange of gasses. Tissue suffocation results from obstructions in the flow of blood through the capillary bed. And cellular suffocation results from metabolic poisons such as rotenone, malonate, and cyanide.
Incidentally, cyanide is a particularly effective metabolic poison in that it completely blocks the cell from exchanging gases. Once inhaled or absorbed through the skin, it only takes about seven seconds to reach every single cell in your body. It is particularly insidious in that at the first whiff, it signals the brain that the body is suffocating, which actually forces your body to take a deep breath — inhaling even more cyanide. The impulse to inhale deeply cannot be resisted by any act of will. Death occurs in about 2-3 breaths. It is so quick acting because it affects virtually every single cell in our body at the same time. Of course, inhaling cyanide is not an issue that most of you are particularly worried about in the course of daily living.
Common clinical obstructions and defense mechanisms
As we’ve already discussed, at the physiological level, most of the problems you face are mechanical, not nutritional. And since we’ve already covered the different types of suffocation you might experience, at this point, it is probably worth focusing for a moment on the different locations that obstructions may occur. For example, other than deliberate strangulation or suffocation, there are very few common clinical obstructions of the nose and mouth that can occur and lead to suffocation because of the dual passageways and the ease in clearing them. Further down, in the larynx, the epiglottis prevents food from entering the airway upon swallowing. It can, however, malfunction if one breathes while swallowing (e.g. when talking). Another potential problem is epiglottitis (a viral infection of the epiglottis), which can also very rapidly cause death if it leads to closure of the airway as the result of swelling.
Another defense against suffocation is the involuntary gag reflex, which protects the breathing passage. The gag reflex is triggered in the back of the throat by anything that is not part of a normal swallowing mechanism. When a chunk of food, for example, is transported towards the back of the tongue, its presence usually elicits an automatic series of muscle contractions designed to propel the food on down the esophagus and into the stomach, in effect, completing the interrupted swallow. Efforts at completing the swallow at first increase, and then, if unsuccessful, are converted to attempts to expel the food out through the mouth. And if that doesn’t work, retching and finally vomiting are triggered.
Involuntary coughing is another protective mechanism used by the respiratory system to defend itself. If any foreign body makes its way into the trachea and/or lungs, violent spasms of coughing serve to expel the foreign matter. The lungs treat the presence of foreign matter as a serious threat — which it is. The coughing is triggered by any foreign body (dust, pollen, fluid, etc.) that is not a gas entering the trachea.
It is worth mentioning that alcohol, anesthesia, and other drugs can decrease or even eliminate both the gag and cough reflexes. This is the primary reason you can’t eat or drink before surgery. As it turns out, as these reflexes are in the process of being suppressed, the vomiting reflex is automatically triggered. This, of course, is a potential major problem in emergency surgery when the patient may have been eating or drinking shortly before the surgery. It is also a potential problem after drinking heavily or overdosing on sleeping pills. Nausea is triggered as consciousness starts to fade. If there is any food or drink in the stomach, vomiting is likely. At that point, since both the gag and coughing reflex are inhibited, choking on the vomit is a strong possibility — as many collegiate binge drinkers, unfortunately, can attest to each year. As a side note, once gag and cough reflexes are fully suppressed, the nausea and potential for vomiting go away. It happens only in “transit” as the reflexes are in the process of being suppressed.
 A third level of protection is offered by the cilia in the tracheo-bronchial tree. These cilia, or hair-like projections in the cells lining the upper airway beat toward the mouth to remove small foreign material. These cilia are an essential part of the respiratory system’s defense mechanisms. Incidentally, cigarette smoking destroys these cilia en masse and in short order. Loss of the cilia harms smokers in three ways:
A third level of protection is offered by the cilia in the tracheo-bronchial tree. These cilia, or hair-like projections in the cells lining the upper airway beat toward the mouth to remove small foreign material. These cilia are an essential part of the respiratory system’s defense mechanisms. Incidentally, cigarette smoking destroys these cilia en masse and in short order. Loss of the cilia harms smokers in three ways:
- First, cancer causing particles and the secretions that trap them cannot be cleared
- Second, because they cannot be cleared, the carcinogens stay in contact with the lining cells longer
- And finally, the absence of cilia makes the lungs and cells lining the trachea bronchial tree that much more vulnerable to other cancer causing pollutants such as smog
Lung cancer is particularly insidious and has an extremely high fatality rate (about 92% once diagnosed) but is easily preventable. Smoking causes 98% of lung cancer — with air pollution and radon gas accounting for the rest. The bottom line is that one of the most deadly cancers — and one of the most prevalent in the world today — is 99% preventable.
Central control of respiration
Respiration is regulated by the brain, and that regulation is both conscious and unconscious (voluntary and involuntary). In a sense, breathing presents us with the intersection of the conscious and unconscious minds. On the one hand, we can breathe without thinking about it — even while asleep or unconscious — and yet, on the other hand, we are fully able to exercise conscious control of our breath. We can control our breathing, speed it up and slow it down and dictate how deep each breath is.
It is interesting to note that the brain’s need to breathe is triggered far more by the build-up of carbon dioxide in the blood than by the need for oxygen — a not so subtle distinction. And in point of fact, this distinction is more than just trivial information. It’s why deep sea divers or yogic breathing make use of hyperventilation to drop CO2 levels as low as possible before taking in and holding your breath.
The brain exercises its control of respiration through several distinct centers of respiratory control in your brain, all of which are driven by small changes in blood chemistry. The medullary rhymicity center establishes the basic normal rhythm of 12-15 breaths per minute at rest. (As we mentioned in our last newsletter, the rate of this rhythm can be reprogrammed to a significantly lower rate.) In fact, the medullary rhymicity center actually has separate inspiratory and expiratory centers. And beyond that, a separate center, the apneustic area, controls breath holding. To a large degree, these centers are regulated by changes in the acid alkaline levels of the blood. And as I just mentioned, these centers can be conditioned/trained to alter their normal rhythms. This is a fact of more than passing interest as:
- Rapid breathing and stress are intimately connected.
- Panic attacks and rapid breathing are also closely related.
- Slower breathing lowers blood pressure
- There is an old wisdom that says that every person on earth is given a specific number of breaths to last their entire life — or to put it in more practical terms, the slower you breathe, the longer you live! This is not mere folk wisdom. Evidence of it is seen throughout the animal kingdom. Animals noted for their longevity such as the elephant and tortoise have respiratory rates significantly slower than human beings. The tortoise, for instance, breathes only 4 times per minute. Tortoises, by the way, can live upwards of 300 years. Animals with fast breathing rates, on the other hand, such as monkeys (32 times per minute) and shrews (660 times a minute) have much shorter life spans — for the shrew, about 18 months. Efficiency in breathing leads to longer life and better physical performance. Top athletes understand this principle.
- In yoga, it is said that breath is the cord that ties the soul to the body.
Incidentally, the respiration centers can be depressed or excited by drugs or alcohol — sometimes with deadly effect. Alcohol is an absolute depressant. Drink enough and you totally shut off the body’s breathing mechanisms. As a side note, the “enjoyment” factor of alcohol comes from the fact that the first thing it depresses is your sense of inhibition. As you continue drinking, the effect of the alcohol then goes on to depress every other function in your brain. In cases of binge drinking, after you pass out, the alcohol in your stomach may continue to suppress your breathing to the point where it stops completely and you die in your sleep or suffer irreversible brain damage. Sleeping pills or narcotics can do the same thing. “Party on, dude!”
Physical trauma that can disrupt respiration
There are really only two primary forms of trauma that can disrupt respiration:
- Pneumothorax (air in the chest)
- Pulmonary edema (fluid in the lungs)
Pneumothorax
If air enters the pleural space between the lung and the chest wall, it causes a loss of the vacuum that, as we’ve already discussed, is necessary for respiration. Where does that air come from? Ninety percent of the time, it comes from outside the chest (e.g. through a hole in the chest wall — gun, knife, etc.) or from the inside if the wound penetrates far enough (e.g. a hole in the lung caused by that same gun or knife). Without a vacuum to hold the lung against the chest wall, the lung collapses (partially or completely), which prevents any gas exchange on that side of the chest. Treatment involves the insertion of a chest tube and suction to recreate the vacuum, then stapling the hole closed. Treating a hole in the chest wall is much easier than treating a hole in the lung. As I mentioned, the primary cause of pneumothorax is external trauma (guns, knives, automobiles, etc.). But on some occasions, holes can be caused by internal conditions such as a spontaneous pneumothorax, a ruptured bleb (an air or fluid filled sac caused by emphysema), or hyperinflation of the lung during anesthesia.
Pulmonary edema (fluid in the lungs)
This is an internal condition, also known as cardiogenic edema , which is caused by failure of the left heart, which causes blood to back up into the lungs. As we discussed in our series on the cardiovascular system, right heart failure causes edema to the body (blood returning to the heart from the body enters through the right atrium). But in pulmonary edema, if the left heart is not pumping out blood as fast as it’s receiving it from the lungs (blood from the lungs reenters the heart through the left atrium), the blood will back up into the lungs. And since it’s under pressure, it will seep into the alveoli and the spaces between the alveoli and fill them with fluid. If not treated immediately, the patient will literally drown in their own blood.
Safeguarding your respiratory system
That concludes our discussion of the physiology of the respiratory system. In the next part of this series, we’ll discuss the diseases of the respiratory system; but before we conclude this issue, let’s briefly talk about some of the things you can do to protect the physiological functions of your respiratory system. And other than the obvious things such as avoiding getting stabbed, shot, or being in an automobile accident, you might want to consider:
- Quitting smoking. 1.2 billion people smoke worldwide — some 43 million in the United States alone. There isn’t much you can say good about smoking. As we’ve already seen, it destroys all of the cilia in your trachea bronchial tree. It is the primary cause of lung cancer and emphysema (which we will talk more about next newsletter). And it’s harmful to everyone around you — even weeks after you finish your cigarette.
- You might want to consider investing in a high quality air filtration system (and no, the Ionic Breeze does not count). The IQAire Health Plus is highly regarded — and is priced accordingly.
- Supplement with a good proteolytic enzyme formula to help thin mucous, reduce inflammation in the lungs, and reduce the chances of embolisms in your lungs.
- Check the radon levels in your house — easy and not expensive.
- Consider incorporating nasal irrigation into your daily routine to optimize the flow of air through your nasal passages.
- As we discussed last issue, practice breathing exercises to optimize the efficiency of your lungs.
- And maybe consider that move to Tasmania after all. Or if you don’t want to live down under, you can check this list of the places that have the world’s cleanest air.
- Oh, and learn the Heimlich maneuver in case of emergencies.
That’s it for now. In our next issue, we’ll conclude our series on the respiratory system by discussing the diseases that can affect your ability to breathe such as COPD, Emphysema, Asthma, Allergies, Bronchitis and flu, Bird flu, Pneumonia, Cystic fibrosis, Pulmonary fibrosis, and Pulmonary embolism.
For more information on the Respiratory System: