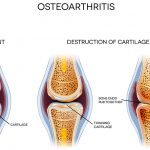
As we get older, wear and tear on the joints causes pain and can limit activities for many people. Knee problems in which cartilage is destroyed over time are very common, particularly in those with osteoarthritis. But if your doctor suggests having total knee replacement surgery to improve your comfort level, you might want to get a second and even third opinion. That’s because new research has found that fewer than half of all total knee replacement operations taking place in the United States can be medically justified.
The subjects were 175 adults who had undergone a total knee replacement procedure. They were all part of a much larger, ongoing study known as the Osteoarthritis Initiative. The average age among the participants in this experiment was 67, and 60 percent of them were women, which closely mimics national statistics for both age and gender for this surgery. The scientists developed a methodology for analyzing the positives and negatives involving the operation for each patient. It included an assessment of pain and functionality in the knee, the range of motion and laxity of the ligaments, radiographic imaging, and the age of the subject. By focusing on these specific criteria, they were able to assign scores and evaluate both the risks and the benefits of having total knee replacement, and ultimately determine which one outweighed the other in each case.
The study, which was conducted at Virginia Commonwealth University in Richmond, found that the potential benefits of total knee replacement surgery were greater than the possible risks for only 44 percent of participants.1 Blaszczak-Boxe, Agata. “Are doctors performing too many unnecessary knee-replacement surgeries?” CBS News. 30 June 2014. Accessed 6 July 2014. http://www.cbsnews.com/news/are-doctors-performing-too-many-unnecessary-knee-replacement-surgeries 34 percent of the surgeries were labeled inappropriate because the risks were determined to be more considerable than the benefits. And the remaining 22 percent were identified as inconclusive since the benefits and risks were essentially at the same level. The risks, incidentally, are not insignificant and include: infection, the new knee coming loose from the bone over time, blood clots formed at the surgical site, patellar clunk syndrome, joint stiffness even after the healing period, and allergic reactions.
These results are worrisome, particularly considering the increasing rates of total knee replacement surgery in recent years. According to the Centers for Disease Control and Prevention, 719,000 total knee replacements took place in 2010. And a 2012 study at Brigham and Women’s Hospital in Boston showed that not only had total knee replacement surgeries more than doubled in frequency between 1999 and 2008, but also that the increase could not possibly all be due to growing population numbers and rates of obesity.2 Losina, E.; et al. “The dramatic increase in total knee replacement utilization rates in the United States cannot be fully explained by growth in population size and the obesity epidemic.” Journal of Bone and Joint Surgery. 1 February 2012. Accessed 7 July 2014. http://www.ncbi.nlm.nih.gov/pubmed/22298051 It is possible another contributing factor is improvements to this type of surgery. And, to some extent the jump in total knee replacement surgeries can also be attributed, at least in part, to fairly widespread coverage of the procedure by insurance companies and the money to be made by the surgeons.
There is a frequently used diagnostic assessment for arthritis patients known as WOMAC, or the Western Ontario and McMaster Universities Arthritis Index, which is based on specific categories of pain, stiffness, and physical function issues. If you have arthritis yet register none or mild on your WOMAC questionnaire answers, you shouldn’t be considered a candidate for knee replacement surgery. This type of procedure should be reserved for only those patients experiencing intense pain and lack of mobility because of severe cartilage deterioration. Other, non-invasive forms of treatment for those with milder cases of arthritis in the knee include making important lifestyle changes such as losing weight and going from high-impact to low-impact exercise. Physical therapy can also be very beneficial for strengthening the nearby muscles and improving the range of motion in the knee.
Osteoarthritis is a very common degenerative disease, with approximately 27 million adults diagnosed in the U.S. Most doctors simply try to alleviate symptoms with pain relievers and anti-inflammatory medications. Instead, there are natural options that can reduce swelling and knee stiffness and discomfort. Even better, some supplements can help repair and even rebuild affected cartilage. For much more on the topic, read Jon Barron’s report called A Five-Pronged Approach to Chronic Joint Pain and Inflammation.
References
| ↑1 | Blaszczak-Boxe, Agata. “Are doctors performing too many unnecessary knee-replacement surgeries?” CBS News. 30 June 2014. Accessed 6 July 2014. http://www.cbsnews.com/news/are-doctors-performing-too-many-unnecessary-knee-replacement-surgeries |
|---|---|
| ↑2 | Losina, E.; et al. “The dramatic increase in total knee replacement utilization rates in the United States cannot be fully explained by growth in population size and the obesity epidemic.” Journal of Bone and Joint Surgery. 1 February 2012. Accessed 7 July 2014. http://www.ncbi.nlm.nih.gov/pubmed/22298051 |