We get thousands of emails at the Foundation every month, and they cover the full gamut — from thanks for the information we provide to requests to join MLM companies to accusations that we’ve abandoned our principles and are now supporting the enemy: mainstream medicine. But that said, there’s one type of email that stands out. And that’s the snarky email from the person who writes in to dismiss an entire newsletter or blog by snottily asking, “Where are the clinical studies to back your support of alternative medicine? I won’t pay attention to anything if it’s not backed by clinical studies.”
Why is this so frustrating?
Because it is based on a mistaken belief, inherent in the question, that mainstream medicine is different — that it’s somehow better, that it’s scientifically “proven” by irrefutable studies. Unfortunately, this belief is both mistaken and naïve and so off base that there’s nothing “we” can ever say to disabuse these people of the notion once they’ve got it locked into their heads.
Fortunately, the mainstream medical community occasionally let’s down its guard and hands us a perfect creampuff of a response that we can use to speak for us. Every now and then, a report or study will slip through from the world of medicine that perfectly highlights how much of medical practice is actually “unproven.” In fact, as it turns out, the vast majority of mainstream medicine is no more “proven” than alternative medicine, and in most cases, it’s decidedly worse since the anecdotal evidence in support of much of alternative medicine at least goes back hundreds of years and has the worldwide validation of millions of people. In truth, as I have pointed out before — and as it turns out, according to the US government’s Office of Technology Assessment (US OTA) — only 10% to 20% of all procedures currently used in medical practice are supported by controlled clinical studies. That’s it — just 10-20 percent! And that’s a blue sky number as it assumes that all studies come to valid conclusions — something we know is categorically not true. After all, I spend three quarters of my time on this website demonstrating why study after study has come to flawed conclusions.
Antibiotics for sinus infections
In a moment, we’re going to take a look at the study on antibiotics that triggered this newsletter and see how it highlights the issues mentioned above, but first we need to take a quick look at the antibiotic landscape to provide some context for the study.
According to a 2005 report in the Journal of Orthomolecular Medicine, “In America, over 3 million pounds of antibiotics are used every year on humans. With a population of 284 million Americans [back in 2005], this amount is enough to give every man, woman, and child 10 teaspoons of pure antibiotics per year1 Null G, Dean C, Feldman M, Rasio D. “Death by medicine.” Journal of Orthomolecular Medicine, 2005. Vol 20, No 1, p 21-34. http://orthomolecular.org/library/jom/2005/pdf/2005-v20n01-p021.pdf ” Also according to the report, “Almost half of patients with upper respiratory tract infections in the U.S. still receive antibiotics from their doctor” even though “the CDC warns that 90% of upper respiratory infections, including children’s ear infections, are viral, and antibiotics don’t treat viral infection. More than 40% of about 50 million prescriptions for antibiotics each year in physicians’ offices were inappropriate.”
Or to look at it another way, in hospitals, 190 million doses of antibiotics are administered each day. In addition, among non-hospitalized patients, more than 133 million courses of antibiotics are prescribed by doctors each year. It is estimated that 50 percent of these latter prescriptions are unnecessary since they are being prescribed for colds, coughs, and other viral infections. Antibiotics only work on bacterial infections, not on viral infections.
But now to the study at hand!
It is estimated that 20% of all antibiotics prescriptions are written for the treatment of sinus infections, which are indeed bacterial. In fact, it’s accepted gospel that antibiotics are the sine qua non of treatment for bacterial sinus infections. And to prove the point, the vast majority of people with sinus infections get better after treatment with antibiotics. So what’s not to love?
 Unfortunately, although antibiotics for sinus infections may be medical gospel, the treatment was also part of the 80% of medical procedures that had never been tested…until now. And the verdict isn’t good. According to a study released just a couple of weeks ago in the Journal of the American Medical Association, the accepted gospel turns out to be unacceptable. In their study of 166 adults with sinus infections, the researchers found that those who took the antibiotic amoxicillin didn’t feel better any faster than those who received a placebo. People in both groups experienced about the same amount of relief after three days.2 Jane M. Garbutt, Christina Banister, Edward Spitznagel, Jay F. Piccirillo. “Amoxicillin for Acute Rhinosinusitis – A Randomized Controlled Trial.” JAMA. 2012;307(7):685-692. http://jama.ama-assn.org/content/307/7/685.short
Unfortunately, although antibiotics for sinus infections may be medical gospel, the treatment was also part of the 80% of medical procedures that had never been tested…until now. And the verdict isn’t good. According to a study released just a couple of weeks ago in the Journal of the American Medical Association, the accepted gospel turns out to be unacceptable. In their study of 166 adults with sinus infections, the researchers found that those who took the antibiotic amoxicillin didn’t feel better any faster than those who received a placebo. People in both groups experienced about the same amount of relief after three days.2 Jane M. Garbutt, Christina Banister, Edward Spitznagel, Jay F. Piccirillo. “Amoxicillin for Acute Rhinosinusitis – A Randomized Controlled Trial.” JAMA. 2012;307(7):685-692. http://jama.ama-assn.org/content/307/7/685.short
To quote the report, “There is now a considerable body of evidence … that antibiotics provide little if any benefit for patients with clinically diagnosed acute rhinosinusitis.” They then added, “Yet, antibiotic treatment for upper respiratory tract infections is often both expected by patients and prescribed by physicians.”
Jay Piccirillo, one of the study’s authors, said that researchers chose the three-day mark because, while it’s well established that most sinus infections resolve by 10 days with or without antibiotics, they wanted to see whether antibiotics hastened resolution. He then continued by saying that if their work had shown that antibiotics made people feel much better by the third day, using the drugs might have been justified. But in fact, by Day 3 of treatment, sinus infection symptoms had improved equally for both groups, with no additional benefits realized by those in the amoxicillin group.
By the seventh day, the results were skewed “slightly” in favor of the amoxicillin group, with a few additional individuals reporting relief from their symptoms. However, the difference was so slight that the researchers concluded that most individuals would not benefit from an antibiotic when experiencing a sinus infection.
To summarize: no difference on day 3; little difference on day 7. As a side note, patients in both groups were permitted to use a handful of over-the-counter medications to manage pain, fever, cough, and nasal congestion.
Now at this point, we could launch into a discussion of why prescribing huge numbers of antibiotics for something with little demonstrable benefit actually presents a huge problem in driving antibiotic resistance. Quite simply, the more you prescribe antibiotics, the more likely that bacteria will develop resistance to them, thus rendering those same antibiotics woefully ineffective over time, ultimately making them useless when needed for something more serious. But that’s a different newsletter. What we’re discussing today is how medicine is much more anecdotal than most people believe.
But lack of supporting studies, as was stated by the Office of Technology Assessment and as was the case with the mistaken practice of prescribing antibiotics for sinus infections, is only part of the problem. The next part of the problem is even more incomprehensible. What if you finally get the studies that prove a procedure doesn’t work…and doctors refuse to pay attention to them? No joke!
Angioplasty
In 2007, I wrote about a study that found that angioplasty did not save lives or prevent heart attacks in non-emergency heart patients.3 William E. Boden, M.D., Robert A. O’Rourke, M.D., Koon K. Teo, et al. “Optimal Medical Therapy with or without PCI for Stable Coronary Disease.” N Engl J Med 2007; 356:1503-1516. http://www.nejm.org/doi/full/10.1056/NEJMoa070829#t=article In fact, according to the study, angioplasty gave only slight and temporary relief from chest pain, the main reason it is performed — virtually no different than that seen with medication. Even more signigicant was the fact that the mortality curves for the angioplasty and medicine groups were virtually identical during the initial 4.6 years of the study. Why are these results important? Because at the time the study was released, doctors were performing about 1.2 million angioplasties a year in the United States alone, at a negotiated cost of about $25 billion a year. That’s $25 billion wasted every year in just the US — and on just this one medical procedure.
Since that initial study, two more studies have come to virtually the same conclusion — that using angioplasty to open blocked arteries to treat chest pain or angina may be riskier and no more beneficial than medication.4 The BARI 2D Study Group. “A Randomized Trial of Therapies for Type 2 Diabetes and Coronary Artery Disease.” N Engl J Med 2009; 360:2503-2515. http://www.nejm.org/doi/full/10.1056/NEJMoa0805796 Obviously, now that multiple scientific studies published in major peer reviewed journals have demonstrated repeatedly that angioplasty is a wasteful and ineffective procedure, and since medicine is evidence based, the procedure has obviously been eliminated from the medical repertoire, right?
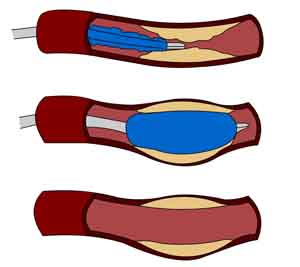 Well, as it turns out, not so much. In all, the reduction in angioplasty surgery since the evidence of its ineffectiveness was first published amounts to a mere 10-15% drop from its peak. Even more startling is that upon being presented with the clear evidence of angioplasty’s ineffectiveness, the response of the medical community was not to decrease the number of angioplasties performed in the US — but to decrease the amount of time required to get one once you’re admitted to the hospital. As the American Heart Association said with great pride just a few days ago, “More than 90 percent of heart attack patients who require an emergency artery-opening procedure known as angioplasty are treated within the recommended 90 minutes, compared to less than half five years before.”5 American Heart Association Rapid Access Journal Report. “Most heart attack patients needing angioplasty treated within recommended time.” 22 Aug 2011. American Heart Association. (Accessed 18 Feb 2012.) http://newsroom.heart.org/pr/aha/most-heart-attack-patients-needing-213626.aspx
Well, as it turns out, not so much. In all, the reduction in angioplasty surgery since the evidence of its ineffectiveness was first published amounts to a mere 10-15% drop from its peak. Even more startling is that upon being presented with the clear evidence of angioplasty’s ineffectiveness, the response of the medical community was not to decrease the number of angioplasties performed in the US — but to decrease the amount of time required to get one once you’re admitted to the hospital. As the American Heart Association said with great pride just a few days ago, “More than 90 percent of heart attack patients who require an emergency artery-opening procedure known as angioplasty are treated within the recommended 90 minutes, compared to less than half five years before.”5 American Heart Association Rapid Access Journal Report. “Most heart attack patients needing angioplasty treated within recommended time.” 22 Aug 2011. American Heart Association. (Accessed 18 Feb 2012.) http://newsroom.heart.org/pr/aha/most-heart-attack-patients-needing-213626.aspx
Wow! What can one say in response other than to spell out the logic of the argument in case anyone missed it?
Medical doctors now have multiple scientific studies performed by their own people that confirm that angioplasties are expensive and essentially useless, and their response is not to stop using the procedure, but to speed up access to it?!!
Wow!
And it’s not like this is an aberration.
Hormone replacement therapy (HRT)
Although I’ve been railing against HRT with synthetic hormones for several decades now, it was not until the early 2000’s that the medical community gave any indication that they were aware there were any risks associated with it. In fact, at that time, HRT was one of the most commonly prescribed treatments in the world. The first chink in the armor came in 2002 and 2004 when the two parallel Women’s Health Initiative (WHI) studies on postmenopausal HRT were cancelled because preliminary study results indicated that the health risks of the conjugated equine estrogen and progestin therapies being used exceeded benefits.[fn/]”NHLBI Stops Trial of Estrogen Plus Progestin Due to Increased Breast Cancer Risk, Lack of Overall Benefit.” 9 Jul 2002. NIH. (Accessed 19 Feb 2012.) http://www.nhlbi.nih.gov/new/press/02-07-09.htm [/fn],6 Barbara Alving. “NIH Asks Participants in Women’s Health Initiative Estrogen-Alone Study to Stop Study Pills, Begin Follow-up Phase.”2 Mar 2004. NIH (Accessed 19 Feb 2012) http://www.nhlbi.nih.gov/new/press/04-03-02.htm In other words, instead of helping women, the protocol was killing them.
In 2003, The Lancet added fuel to the fire when it published the results of the Million Women Study, which provided the first clinical evidence that HRT is associated with both a substantially greater risk of getting breast cancer…and dying from it.7 Million Women Study Collaborators. “Breast cancer and hormone-replacement therapy in the Million Women Study.” The Lancet, Volume 362, Issue 9382, Pages 419 – 427, 9 August 2003. The study found that all types of HRT, including estrogen and progestin combinations, and estrogen alone — but always involving synthetic forms of both hormones — increased the risk of breast cancer.
It reached a crescendo of negativity in 2008-2009 with the publication of three disturbing studies. The first found that HRT leads to a 62 percent increased risk of stroke,8 Francine Grodstein, JoAnn E. Manson, Meir J. Stampfer, Kathryn Rexrode. “Postmenopausal Hormone Therapy and Stroke – Role of Time Since Menopause and Age at Initiation of Hormone Therapy. Arch Intern Med. 2008;168(8):861-866. http://archinte.ama-assn.org/cgi/content/full/168/8/861 and the second found that it leads to a 35 percent increased risk of heart disease.9 Ellen Løkkegaard1,Anne Helms Andreasen, Rikke Kart Jacobsen, et al. “Hormone therapy and risk of myocardial infarction: a national register study.” Eur Heart J (2008) 29 (21): 2660-2668. <http://eurheartj.oxfordjournals.org/content/29/21/2660.full.pdf+html> The third study was actually a follow up on the two WHI studies and found that within a year of discontinuing HRT, the number of new breast cancers among women in the first WHI study declined by 28 percent.10 Rowan T. Chlebowski, Lewis H. Kuller, Ross L. Prentice, et al. “Breast Cancer after Use of Estrogen plus Progestin in Postmenopausal Women.” N Engl J Med 2009; 360:573-587February 5, 2009. http://www.nejm.org/doi/pdf/10.1056/NEJMoa0807684 The study also found that 50 percent of the subjects in the second WHI study had stopped HRT as recommended, and that was reflected in a 43 percent drop in new breast cancers. Plus, when news got out to the public, women stopped taking HRT in substantial numbers, and again, breast cancer rates plummeted. (Ironically, this plunge in breast cancer incidence and mortality was then promoted by the medical community as evidence of the great advances being made in breast cancer treatment. Wow, again!)
 So where do things stand today with HRT? You might think, having been found only marginally effective, and with study after study now proving that it significantly increases mortality, and, most importantly, since there is an alternative using bio-identical hormones which appears to be more effective and does not carry the same risks, that HRT would be pretty much passé — confined to a medical museum, along with surgery without anesthesia and mercury to treat syphilis. But if you thought that, you’d be wrong. Because, in spite of the nearly undeniable congruence between HRT use and disease risk, many in the medical establishment claim that the reduction in breast cancer has more to do with the fact that the subjects in the studies got more frequent mammograms than women in the general public, and that fewer mammograms means fewer detected cancers. In other words, they claim that cancer rates aren’t really less — we’re just detecting fewer of them.
So where do things stand today with HRT? You might think, having been found only marginally effective, and with study after study now proving that it significantly increases mortality, and, most importantly, since there is an alternative using bio-identical hormones which appears to be more effective and does not carry the same risks, that HRT would be pretty much passé — confined to a medical museum, along with surgery without anesthesia and mercury to treat syphilis. But if you thought that, you’d be wrong. Because, in spite of the nearly undeniable congruence between HRT use and disease risk, many in the medical establishment claim that the reduction in breast cancer has more to do with the fact that the subjects in the studies got more frequent mammograms than women in the general public, and that fewer mammograms means fewer detected cancers. In other words, they claim that cancer rates aren’t really less — we’re just detecting fewer of them.
The International Menopause Society (great name) actually disputed the studies claiming that breast cancer takes 10 years to develop, so cancers reported in the studies could not possibly have resulted from HRT.11 “A rapid decline in the incidence of breast cancer following cessation of menopausal hormone therapy: sense or nonsense?” 21 Jan 2009. International Menopausal Society. (Accessed 19 Feb 2012.) http://www.imsociety.org/updates_view_open.php?menopauseliveID=141&SESSID=bj47hkpr8ghipqh5iv22t5kcu1 Then again, where does that 10 year figure come from? What studies is it based on? Before the WHI study, who had made the connection between HRT and breast cancer…other than the alternative health community? And finally, not to be outdone, the pharmaceutical companies chimed in. According to a spokesperson for Wyeth, the company that manufactured one of the leading HRT pills of the day, “We don’t believe the article [study] supports the theory that the decline in use of estrogen plus progesterone caused a one-time abrupt nationwide decline in breast cancer incidence. If this was the case, then we should be seeing further reductions in breast cancer rates because the rates of HRT use continue to fall, but we aren’t seeing this.”
Although it seems inconceivable, given the peer reviewed study-based evidence, a number of medical professionals have bought into these counterclaims and are still arguing in favor of prescription HRT drugs — and successfully it would seem. As many as 36 million prescriptions are still written for them every year.12 “Hormone Therapy Statistics (Updated June 2011).” North American Menopause Society. (Accessed 19 Feb 2012.) http://www.menopause.org/hormonetherapystats.aspx Yes, that’s down from their peak in 2001, but 36 million is still huge…and inexplicable based on the evidence. It would seem that medical doctors are quite willing to ignore any studies that fall outside their ingrained belief system. In other words, just because your doctor is prescribing a treatment for you doesn’t necessarily mean that the majority of studies support it. In fact, it might be quite the contrary.
The bottom line, once again, is that modern medicine is not really based on scientific studies — despite what we have been led to believe. Less than one percent of health care spending in the US goes to examining what treatments are most effective. And even when that information finds its way into peer reviewed journals, it can take up to 17 years to gain widespread acceptance in the medical community and eventually to the exam room or operating table. When they first said “you can’t teach an old dog new tricks,” they could just as well have been talking about doctors as dogs. According to a 2009 study, less than half of all cardiac guidelines are based on scientific evidence.13 Tricoci P, Allen, JM, Kramer JM, Califf RM, Smith SC JR. “Scientific evidence underlying the ACC/AHA Clinical Practice Guidelines.” JAMA. 2009;301:831-841. http://jama.ama-assn.org/content/301/8/831.full But that “less than half” estimate is at the high end. When you factor in the less “glamorous” areas of medicine, which are less studied, not to mention off-labeling (prescriptions for uses other than those for which the drug was created and tested), which involves no scientific study and accounts for 21% of all pharmaceutical sales, and we’re back to the OTA assessment that only 10-20% of all medical procedures are validated by scientific research. As a result, too many doctors and patients are making decisions without the benefit of the latest research; they only think they are.
In truth, it is amazing how little has changed since 1978 when the US OTA made its pronouncement — and since we keep referring to it, perhaps we should look at the exact quote:
“It has been estimated that only 10 to 20 percent of all procedures currently used in medical practice have been shown to be efficacious by controlled trial. Given the shortcomings in current assessment systems, the examples of technologies that entered widespread use and were shown later to be inefficacious or unsafe, and the large numbers of inadequately assessed current and emerging technologies, improvements are critically needed in the information base regarding safety and efficacy and the processes for its generation.”14 “Assessing the Efficacy and Safety of Medical Technologies.” Sept 1978. OTA Congress of the United States. http://www.fas.org/ota/reports/7805.pdf
But that’s still not the worst of it.
When studies are just plain wrong — deliberately
So far, we’ve been talking about the 80% of procedures that are unstudied — but are believed to be correct based on anecdotal evidence. And we’ve talked about the studies that seem to prove a point, but are still, for years, argued against by diehards who still insist on prescribing discredited procedures…to the bitter end. But in both cases, we’re at least talking about honest attempts to arrive at a consensus. Unfortunately, there’s a whole other side of studies that is notably less honest.
Working out of Duke University, Dr. Anil Potti conducted a series of studies on individualized treatments for cancer that were published in peer reviewed journals and were considered “the holy grail of cancer.” Personalized cancer treatments, if they worked as indicated in Dr. Potti’s studies, could be a last hope for people whose bodies don’t respond to conventional treatments. Unfortunately, it turned out that Dr. Potti had jigged his data to produce his favorable studies.
As a result, Dr. Potti was forced to resign his position at Duke, nine of his widely cited papers have been retracted from medical journals, and law suits have been filed by patients (or their surviving relatives) who feel they were misled and given false hope when participating in his studies.15 Roxanne Nelson. “Dr. Potti and Duke University Sued Over Faulty Research.” 13 Sept 2011. Medscape Today News. (Accessed 19 Feb 2012.) http://www.medscape.com/viewarticle/749577
 There are two lessons here. First is that just because a study is peer reviewed does not “guarantee” the validity of its results, despite what most people believe. Peer review only means that the “logic” behind a study and its “methodology” “appear” to be valid to other professionals who have read the paper before it is published. Peer review does not and cannot catch false data or deception. Second, once a flawed study is peer reviewed and published, it now becomes a cited source for other studies, which then propagate its false conclusions — giving those conclusions ever more credence as study after study bases its conclusions on the original false data — until such time as the conclusions become gospel in the scientific world, despite being as false as the day they were formulated out of fabricated data. In law, they would call this the fruit of the poisonous tree. Sometimes it can take years — even decades — for an entrenched falsehood to be overturned and the house of cards built on it to come crashing down.
There are two lessons here. First is that just because a study is peer reviewed does not “guarantee” the validity of its results, despite what most people believe. Peer review only means that the “logic” behind a study and its “methodology” “appear” to be valid to other professionals who have read the paper before it is published. Peer review does not and cannot catch false data or deception. Second, once a flawed study is peer reviewed and published, it now becomes a cited source for other studies, which then propagate its false conclusions — giving those conclusions ever more credence as study after study bases its conclusions on the original false data — until such time as the conclusions become gospel in the scientific world, despite being as false as the day they were formulated out of fabricated data. In law, they would call this the fruit of the poisonous tree. Sometimes it can take years — even decades — for an entrenched falsehood to be overturned and the house of cards built on it to come crashing down.
And this happens more often than you might think. For example, there’s the work of Dr. Dipak K. Das, Ph.D., a professor in the Department of Surgery and Director of the Cardiovascular Research Center at the University of Connecticut. An investigation of his research conducted over the last decade concluded that he was guilty of 145 counts of fabrication and falsification of data.16 Chris DeFrancesco. “Scientific Journals Notified Following Research Misconduct Investigation.” 11 Jan 2012. UCONN Today. (Accessed 19 Feb 2012.) http://today.uconn.edu/blog/2012/01/scientific-journals-notified-following-research-misconduct-investigation/ His work was vetted and published in a number of peer reviewed journals, including:
- American Journal of Physiology — Heart & Circulatory
- Antioxidants & Redox Signaling
- Cellular Physiology & Biochemistry
- Free Radical Biology
- Free Radical Research
- Journal of Agriculture and Food Chemistry
- Journal of Cellular & Molecular Medicine
- Journal of Nutritional Biochemistry
- Journal of Pharmacology and Experimental Therapeutics
- Molecular & Cellular Cardiology
- Molecular & Cellular Chemistry
And his work was highly cited, highly influential. Thirty of his papers were cited more than 100 times each, according to Thomson Scientific’s Web of Knowledge. One, in Toxicology, was cited 349 times, while another, in Free Radical Biology, was cited 230 times.
To reiterate, falsified studies were peer reviewed and vetted in multiple prestigious journals. And the falsehoods only came to light because of an inside tip — not through peer review.
Wow yet again!
Conclusion
Look, I’m not saying that all studies are bad or that there is no science in medicine. That’s obviously absurd. All I’m saying is that peer reviewed studies, although they are important tools, provide far less validation and certitude than most people think. The other important point is that a large percentage of medicine is based on much less science than you have been led to believe. In fact, studies are often merely an attempt by researchers to present their hypotheses in a way that the medical community will embrace — thus advancing their career. Or even worse, they are often presented by pharmaceutical companies in an attempt to convince the FDA and doctors to embrace their products. In fact, pharmaceutical companies get to run their own studies to test their own products. They then get to filter the results — to cherry pick the data, throwing out negative studies and submitting only the favorable studies to the FDA for approval. They can pay for 20 studies for their drug, as an example, of which 17 come back negative, and then submit only the three positives to the FDA — thus getting their drug approved based on just 15% of their studies indicating any benefit for the drug. And only the three positive studies get published in peer reviewed journals; the 17 negative studies are simply buried. Your physician, who then prescribes the drug for you, never sees them. She prescribes based on the distorted three studies she gets to read. And when you take your prescription drugs, you’re convinced they’re backed by solid science, even when that’s not necessarily so. And then sometimes, pharmaceutical companies simply decide to skip all that inconvenience and simply hire “ghost researchers” to put their name on articles actually written by the pharmaceutical companies’ own marketing departments. That allows pure marketing material to be peer reviewed and become part of the medical database and be cited as authenticated studies by subsequent researchers — thus perpetuating pure fabrication.
Coda:
In the midst of my writing this newsletter, 60 Minutes came out with a story about how repeated studies have shown that antidepressants are no better than placebos except in cases of extreme depression. (How many times have I said that?) As part of the story, they interviewed doctors who still believe in antidepressants and therefore discounted the studies because the studies’ results weren’t congruent with their existing paradigm. Instead, those doctors cited studies performed by the pharmaceutical companies “proving” that their drugs do indeed work.
Wow for the final time!
In the end, the 60 Minutes story is the perfect coda to this newsletter — graphically demonstrating how nebulous the science behind medical treatments actually is. Enjoy!
PS: For those of you who have successfully used antidepressants for mild depression and swear by them and therefore think this study must be nonsense, the 60 Minutes story explains how that works.
References
| ↑1 | Null G, Dean C, Feldman M, Rasio D. “Death by medicine.” Journal of Orthomolecular Medicine, 2005. Vol 20, No 1, p 21-34. http://orthomolecular.org/library/jom/2005/pdf/2005-v20n01-p021.pdf |
|---|---|
| ↑2 | Jane M. Garbutt, Christina Banister, Edward Spitznagel, Jay F. Piccirillo. “Amoxicillin for Acute Rhinosinusitis – A Randomized Controlled Trial.” JAMA. 2012;307(7):685-692. http://jama.ama-assn.org/content/307/7/685.short |
| ↑3 | William E. Boden, M.D., Robert A. O’Rourke, M.D., Koon K. Teo, et al. “Optimal Medical Therapy with or without PCI for Stable Coronary Disease.” N Engl J Med 2007; 356:1503-1516. http://www.nejm.org/doi/full/10.1056/NEJMoa070829#t=article |
| ↑4 | The BARI 2D Study Group. “A Randomized Trial of Therapies for Type 2 Diabetes and Coronary Artery Disease.” N Engl J Med 2009; 360:2503-2515. http://www.nejm.org/doi/full/10.1056/NEJMoa0805796 |
| ↑5 | American Heart Association Rapid Access Journal Report. “Most heart attack patients needing angioplasty treated within recommended time.” 22 Aug 2011. American Heart Association. (Accessed 18 Feb 2012.) http://newsroom.heart.org/pr/aha/most-heart-attack-patients-needing-213626.aspx |
| ↑6 | Barbara Alving. “NIH Asks Participants in Women’s Health Initiative Estrogen-Alone Study to Stop Study Pills, Begin Follow-up Phase.”2 Mar 2004. NIH (Accessed 19 Feb 2012) http://www.nhlbi.nih.gov/new/press/04-03-02.htm |
| ↑7 | Million Women Study Collaborators. “Breast cancer and hormone-replacement therapy in the Million Women Study.” The Lancet, Volume 362, Issue 9382, Pages 419 – 427, 9 August 2003. |
| ↑8 | Francine Grodstein, JoAnn E. Manson, Meir J. Stampfer, Kathryn Rexrode. “Postmenopausal Hormone Therapy and Stroke – Role of Time Since Menopause and Age at Initiation of Hormone Therapy. Arch Intern Med. 2008;168(8):861-866. http://archinte.ama-assn.org/cgi/content/full/168/8/861 |
| ↑9 | Ellen Løkkegaard1,Anne Helms Andreasen, Rikke Kart Jacobsen, et al. “Hormone therapy and risk of myocardial infarction: a national register study.” Eur Heart J (2008) 29 (21): 2660-2668. <http://eurheartj.oxfordjournals.org/content/29/21/2660.full.pdf+html> |
| ↑10 | Rowan T. Chlebowski, Lewis H. Kuller, Ross L. Prentice, et al. “Breast Cancer after Use of Estrogen plus Progestin in Postmenopausal Women.” N Engl J Med 2009; 360:573-587February 5, 2009. http://www.nejm.org/doi/pdf/10.1056/NEJMoa0807684 |
| ↑11 | “A rapid decline in the incidence of breast cancer following cessation of menopausal hormone therapy: sense or nonsense?” 21 Jan 2009. International Menopausal Society. (Accessed 19 Feb 2012.) http://www.imsociety.org/updates_view_open.php?menopauseliveID=141&SESSID=bj47hkpr8ghipqh5iv22t5kcu1 |
| ↑12 | “Hormone Therapy Statistics (Updated June 2011).” North American Menopause Society. (Accessed 19 Feb 2012.) http://www.menopause.org/hormonetherapystats.aspx |
| ↑13 | Tricoci P, Allen, JM, Kramer JM, Califf RM, Smith SC JR. “Scientific evidence underlying the ACC/AHA Clinical Practice Guidelines.” JAMA. 2009;301:831-841. http://jama.ama-assn.org/content/301/8/831.full |
| ↑14 | “Assessing the Efficacy and Safety of Medical Technologies.” Sept 1978. OTA Congress of the United States. http://www.fas.org/ota/reports/7805.pdf |
| ↑15 | Roxanne Nelson. “Dr. Potti and Duke University Sued Over Faulty Research.” 13 Sept 2011. Medscape Today News. (Accessed 19 Feb 2012.) http://www.medscape.com/viewarticle/749577 |
| ↑16 | Chris DeFrancesco. “Scientific Journals Notified Following Research Misconduct Investigation.” 11 Jan 2012. UCONN Today. (Accessed 19 Feb 2012.) http://today.uconn.edu/blog/2012/01/scientific-journals-notified-following-research-misconduct-investigation/ |








Dear Jon Barron , Thank you !
Dear Jon Barron , Thank you ! “Illness” isn’t always a medical problem . For example , if a person is mentally depressed about people being homeless , taking a pill will not make homes for these people . Thank you . John
What can one say? Brilliant!!
What can one say? Brilliant!! I really appreciate your powers of reasoning, Jon. Praise God who gave you this talent.
Kind regards
Johanita Louw
South Africa
Thank you once again, Jon,
Thank you once again, Jon, for giving me a chance to comment on your comments.
Colds and flus are already the healing phases and it is evident, that one cannot speed up healing. Thank God the doctors are so ignorant and in many cases stupid!
There are NO viruses! What is commonly referred to as viruses, are bits of protein, created by the bodies’ cells for use as a re-building substance to rebuild the ulcerations in the sinuses and nasal membranes. They were ulcerated to enhance airflow through them, following a conflict shock event called a “stink” conflict. All so called illnesses occur in two phases, a conflict active phase and a conflict resolved phase. That automatically means, that there are only half the number of illnesses commonly thought to exist.
Nature’s purpose of creating an ill feeling in the healing phase is, to make an individual take a rest in order for Nature to have a better chance to heal more effectively and more efficiently. Therefore it is folly to try and create a drug to heal a healing phase! (the same goes for vaccines).
Yes, I’m delighted about the “cream puff” events too.
Glandular breast cancer is caused by an unexpected shock event involving a worry about a family member and ductal breast cancer is caused by an unexpected forcible separation conflict.
Heart attacks are suffered in the healing crisis of right handed males and post menopausal right handed females, due to the edema in the right temporal lobe of the brain getting squeezed out, flooding the slow heart beat center in this location, preventing the beat signal from reaching the heart. It has nothing to do with narrowing the arteries per se, although this is part of the picture, because the arteries are being repaired, following a territorial loss conflict event, which caused the coronary artery to become ulcerated in order to have more blood flow to the heart in the likely attempt to win the territory back. If the conflict stays active for more than nine months, it is fatal.
Thanks Jon and Harald! This
Thanks Jon and Harald! This truth deserves to go viral! "Disease" is such a racket in Western Medicine! Especially if we realize that most healing symptoms do not need medical treatment. It is only through our ignorance and a conditioned belief system (both perpetrated by "modern" "medicine") that people have allowed the medical cult to become what it is today. The "New Medicine" is a paradigm shift whose time has come and it is my divine pleasure to support this shift to the nest of my ability! I am so grateful for learninggnm.com Thank you Jon and All for this lead article! I appreciate the subject matter and strongly agree that the idea that "conventional medicine is backed by science" is essentially a false belief. I very recently sent a message to the CDC asking for more information regarding their quality of statistics and whether there is a government-mandated quality standard that they follow and if so what do they actually do to assure the highest quality in their process up to and including presenting health statistics. The FDA clams that people who drink raw milk are playing "Russian Roulette". That phrase was actually repeated by a presenter at the recent raw milk debate that was hosted by the Harvard Food Law Society". curezone.com/blogs/fm.asp?i=1912116 The "debate" got me thinking about the soundness of statistics. That brought me to wonder whether there is any oversight for "quality control" at the CDC for statistics regarding the incidences of raw milk contamination. That's my "mission" now and I am looking forward to hearing back from CDC about that! According to Mark McAfee "The CDC has really done a public service to us all. By publishing extreme bias and miscalculated illness data on raw verses pasteurized milk … again the government has stimulated conscious consumers to buy raw milk. Those that the CDC has attempted to scare off from raw milk…now clamber for it." Mark is featured in "Raw Milk: The Whole Truth" Cheers!
Thank you for making tangled,
Thank you for making tangled, murky issues so much clearer. I am so grateful I found your site years ago and even more grateful that you continue to advocate for ordinary folks. The most authentic health advice is so often the simplest…we simply refuse to “hear”. Like: moderation, a positive outlook, practicing kindness and patience, eating nourishing, vibrant meals with family every day, doing all you can every day to honor the magnificent gift of your physical body thru joyful exercise, abstaining from harmful habits and activities. And remembering how many, many vexatious health problems can be eradicated by changes in behavior, outlook, and multitudes of effective alternative methods. God bless you and your work.
Sincerely, Patricia
I have Sjogren's and have had
I have Sjogren’s and have had lots of sinus issues. I have found that Amoxicillin has never been strong enough to take care of my sinus infections. I always need a stronger one. So, now we skip the Aoxi and go to something stronger and it always takes care of the problem.
I used to have many sinus
I used to have many sinus infections until I eliminated dairy from my diet. Then a blood test showed that I was intolerant to gluten as well. If you cut down on those, increase your vitamin D3 (I take 10,000 iu’s per day) you may never see a sinus infection, cold or flu again. But if you do, organic apple cider vinegar works instantly every time. Good luck.
Jon,
Good reading, but I beg
Jon,
Good reading, but I beg to differ with you on the cause of sinus infections . . . not all are caused by bacterial infections, in fact most are caused by an over growth of yeast in the body from eating sweets or too many carbs. Yeast infections also show up on the skin in many people. May I suggest for your enjoyment and to add to your wealth of knowledge that you do a bit more research on the subject of yeast overgrowth and see what you’ll find.
I personally know a lady who had on going sinus problems treated with antibiotics only to have several surgeries that didn’t help either. It wasn’t until she changed her diet and went on a Yeast Cleanse program that she was well rid of it.
Thanks for your wonderful newsletter . . . I always enjoy it and pass it along to my friends. Keep up the good work.
re: Unproven Medicine, Came
re: Unproven Medicine, Came across this article written about a year ago that supports many of your comments. Thought your readers might like another take on the subject. Thanks. Love your "essays' on the "medical dynasty" of today!! Jim Comp
I am not a fan of
I am not a fan of antibiotics, but I would like to comment that, in your analysis of the study using amoxicillin, is it not possible that the “usual” bacteria targeted when treating SI might have developed resistance to amox? OR could there be an atypical source of SI that is being seen more frequently these days? Thank you, though, for your general thoroughness and insistence on asking the right questions about our medical research and our medical system. Indoctrination to current paradigm is still very much the case in the health care field, as it is in other “well-accepted” areas of science.
(not verified)isn't that what
(not verified)isn’t that what we learned about the drugs that are given to our children? Fear is why any doctor can’t sound off.Coda wants to have international clout. Much power in a not so veiled glove.Bill of Rights verses corporate clout. What can money buy? Or in the eyes of amoral corporations, what can’t money buy? Your right to include (ESSENTIAL VITAMINS AND MINERALS)in your diet is at stake.Be heard get active.Now, Now, Now, thank you.
Very interesting especially
Very interesting especially the part about angioplasty.
But do you recommend an alternative treatment to clear blocked arteries or
hardening or calcification?
The comment by Harald is
The comment by Harald is based on the Evidence Based medical research of Oncologist Dr.Geert Hammer, very few, in the Medical community especially, have been able/willing to accept true evidence based -science. The issue at hand here is not so much to prove the ‘disprovable..’ but, the trained western mind in how it perceives reality… Also, his research is, especially here in the US, taken up by the ‘Alternative Community of ‘Quacks,” who upon reading the Evidence recognized the validity of the very lengthy research done by Dr. Hammer.
The very thought process behind medical science depends on the ability to isolate chemical compounds or reactions in A CONTROLLED ENVIRONMENT. The problem with that premise is that the body does not represent a controlled environment. The millions of things happening at the same time requires a much broader and larger perspective in order to recognize the bodies innate wisdom in shutting down, redirecting, repairing and Surviving.
The body is always looking to live. You give it the Right fuel, it will find a way to use it. Our ability to adapt to the varied influences that are harmful to us, actually stands in the way of paying mind to the myriad of stupid things we do to ourselves and that influence the function. You cannot isolate an Emotional Influence in a petri dish and call it ‘science.’ You can recognize the many physical changes that take place when a person expresses an emotion. How do you compensate for that in a petri dish and then prove the thousands of chemical reactions that take place at once…? Only Logical thinking and observation shows you the reality of such an event and the reasonable conclusion that- wow – where is the science that shows that the lack of oxygen flowing to my brain as a result of this fit is giving me a headache, is not allowing me to digest my food, is causing rotting food in my digestive tract, is resulting in bacteria doing the clean up, mmm, maybe I should get some anti-biotics..ha ha ha
So true….
There is another
So true….
There is another great piece of sophistry that goes to the belief that traditional medicine is the basis of all….. It is the sophistry of stating that if any “alternative” medicine works it is simply a placebo effect because the patient believes in it…
Now, does that mean that the patient does not believe in the “real” medicine peddled by the doctor? Does that mean the the so-called positive reactions to the real medicine in double-blind, placebo tests is NOT ALSO PLACEBO…?
In short, I am claiming that if any big pharma medicine works it is due to the placebo effect (if it does not kill the patient first)
The whole notion of Placebo is pure and utter bollocks… and is mainly used to attempt to debunk inexpensive remedies that cannot be patented and that do work….
Pure and utter sophistry…..