MRSA, a virulent form of staph infection, has been giving the medical community a workout as new, antibiotic-resistant strains keep developing. Recently a new strain of MRSA has demonstrated resistance to the antibiotic Zyvox, which was considered to be the one solution that would work when all other antibiotics failed — until now. Although “isolated” cases of Zyvox-resistance have been reported in the past, in this case, 12 patients in the intensive care unit of a hospital in Madrid, Spain, all developed MRSA that failed to respond to the drug.
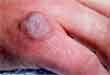
MRSA stands for methicillin-resistant Staphylococcus aureus, which indicates a staph infection that has become resistant to penicillin. While other staph infections easily succumb to antibiotics, MRSA infections don’t. Although staph bacteria live on the skin and typically cause no problems, infection can occur when someone with a compromised immune system either breathes in the bacteria or gets a skin wound through which staph bacteria enter the bloodstream. If the invading bacteria happen to be antibiotic-resistant, the victim is in trouble.
One out of every five patients who develops an MRSA infection dies from it. In 2007, 95,000 new cases of MRSA were reported in the US, and 19,000 people lost their lives from it. Eighty-five percent of those new MRSA infections originated in hospital settings, where people with surgical wounds and compromised immune systems crowd together, passing bacteria from one bed to the next.
The scientific community keeps working away to create a super-antibiotic that MRSA won’t become resistant to. Each time a new drug comes to market with promises of invulnerability, it ends up like its predecessors — powerless against MRSA (or at least the next mutation of it). Although Zyvox-resistant MRSA has so far manifested only in a very small number of patients, it’s a good bet that now that the bacteria has developed a resistant strain, it will spread. That’s certainly what’s happened in the past. Before Zyvox, vancomycin was the miracle drug that eventually stopped working.
Of course, it’s no surprise that Zyvox has hit the therapeutic wall, though the media and the medical world might act stupefied. As I’ve written before, where antibiotics and bacteria collide, resistance is inevitable. Any population of bacteria includes countless variants, so when an antibiotic kills the vulnerable variants, those few strains that are resistant to the antibiotic multiply and become stronger. The very act of using an antibiotic creates the opportunity for strains resistant to it to flourish. Add to that the fact that bacteria can swap genes, meaning that bacteria not only can develop a defense to antibiotics, but they can mutate and teach other bacteria (of entirely different strains) how to do the same thing. (That’s actually very scary if you think about it.)
Because bacteria have a simple structure, they don’t need to go through sophisticated mutations to outsmart antibiotics, which are one-dimensional weapons. If bacteria undergo just a simple change in a cell wall or in an internal structure, the antibiotic no longer works. That’s why combinations of antibiotics sometimes work better than just a single drug. But combinations merely delay the inevitable; they don’t eliminate it. All of this means that the more use an antibiotic gets, the more opportunity bacteria have to mutate and become resistant.
It seems obvious that if bacteria can make simple changes that render antibiotics useless, a more complex solution might work better — something more complex than combination shots, that is. Natural remedies usually contain scores of active biochemicals that work together in countless combinations. For instance, garlic contains allicin, a natural antibiotic that breaks down into over 100 biologically active compounds. Any two of those compounds is the equivalent of using two antibiotics — any three compounds, three antibiotics — etc. The bottom line is that using garlic alone is equivalent to using a combination of 100 different antibiotics all at once. When you combine garlic with other natural anti-pathogens such as ginger, onion, grapefruit seed extract, olive leaf extract, and liquid ionic zinc, you create thousands and thousands of combinations far too complex for a bacterium to evolve around.
But the pharmaceutical companies seemingly aren’t that interested in complex, effective, powerful natural remedies that lack side effects. Rather, they’re busily creating the next all-powerful antibiotic to replace Zyvox. So far, PTK 0796 leads the pack of potential new drugs, after demonstrating 98-percent effectiveness against MRSA. There’s also something called Iclaprim with a 93-percent success rate against MRSA skin infections, and ceftaroline, at 95 percent. All of these drugs are in experimental stages; all hold great promise right now and will potentially wipe out a large number of staph infections before becoming obsolete. But make no mistake, they will all become obsolete for sure in short order, and will cause health-compromising side-effects along the way.
Better to keep your immunity levels high by taking an immunity-boosting formula. Stay out of hospitals if at all possible, and if you do feel an infection coming on, take a natural antibiotic cocktail.
:hc










Thank God, there is one person on earth who is speaking out. Most doctors and nurses think its a joke. They are still living in an illusion that a miracle drug will be available soon to combat these bugs.
We need to join hands and at least educate people more about these bacteria.
It looks as if these bacteria are one step ahead of us in gene manipulation and technology transfer, a true “”Alien of Intellectual ability””
The sad thing is that many different essential oils rose,oregano, eucalyptus globulus, sandalwood, rosemary etc.. Have all been shown in the lab to kill it very quickly. Of course these are only Bella Mira Essential Oils that the test were done on. Other very effective solutions are colloidal/ ionic silver, copper, and gold, ozone and hydrogen peroxide.
The worse thing is that doctors are routinely prescribing Vancomycin and Cipro to some patients for cuts or pimples out of fear. Or others are jumping to these super antibiotics in patients with frequent antibiotic usage out of fear of resistance; further exacerbating the problem.
I believe it is medical malpractice to use antibiotics unless all other proven natural methods fail. Even then, lab tests should be done to match the least effective antibiotic that will do the job.
Thank you for a great article! I first learned of antibiotic resistant strains from Natasha Trenev (Natren). Her words are echoed in your writing.
The natural remedies you mentioned are all very important weapons. I would add probiotics from a reputable company such as Natren or Dr. Ohirras.
One of the worst things doctors do, for which I blame drug company sponsored medical schools, is prescribe antibiotics for a fungal problem.
Doug Kaufmann (Know the Cause) read an e mail about a lady who delivered a baby. The process was so quick that the doctor didn’t have time to give her her dose of antibiotics, reason being all that bacteria in the vaginal tract couldn’t possibly be good for the infant. INSANE!
Good post, Jon.
One thing MRSA has not been able to beat is top quality colloidal and ionic silver and colloidal silver (which is why MRSA is almost non-existent in hostpitals that use silver extensively – such as in their air vents)
The colloida silver is best internally and the ionic silver best externally. If you use a quality product and use enough of it, MSRA will be defeated. (Utopiasilver.com is the best source I know of for both)
Oil of oregano is another good natural alternative for MRSA.
Taking good anti-virals and pathogen destroyers like the ones you recommend and keeping a strong immune system will help avoid MRSA in the first place.