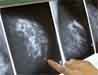
If there’s one thing most women agree on, it’s the fact that going for the routine mammogram is about as distasteful as doing the annual tax return — which may be one reason fewer and fewer women show up for it. Back in 2000, 70 percent of women in the US had regular mammograms, but that figure slipped to 66 percent by 2005, and the downward trend continues. Plus, a huge study reviewing Medicare records of 146,669 women nationwide found that far fewer actually had mammograms than claimed they did, dropping the real percentage to more like 61 percent — which leaves almost 40 percent of women without screening.
The fact that so many women forego mammograms has experts worried. To counter the trend, researchers at Kaiser Permanente’s Research Center in Portland, Oregon, instituted a program of intensive reminders, including postcards, automated phone calls, and personal calls reminding women to make an appointment. The approach worked, with women hounded by the “mammogram police” 1.5 times more likely to book their exam than those who got no special reminders.
“If this was widely used we believe we would be able to detect 25,000 additional early breast cancers in the U.S.,” said study director Dr. Adrienne Feldstein. And yes, from the standpoint of garnering participation, the effort seems encouraging, but the real question is whether or not mammograms actually are as important as the medical establishment makes them out to be.
Actually, mammograms are nowhere near as foolproof as the doctors would have women believe. A 2006 study found that fully one-third of all women interviewed were convinced that mammograms could invariably detect all cancers, no matter how small. But the truth is that 20 to 30 percent of the time, the mammogram can miss tumors. Sometimes it’s because of size, and sometimes, according to radiologist Dr. Marilyn Roubidoux of the University of Michigan, “The issue isn’t that these cancers are small, but that they are hard to see. Some breast cancers just hide. You can’t see a seagull in a cloudy sky.” Plus, the rate of false positives, by some estimates, is as high as 90 percent or greater.
It’s this reality that provoked Emory University Assistant Director of Imaging, Mary S. Newell, to say, “I think we have oversold mammography to some degree. It is a good test. It has decreased breast cancer deaths in women who get annual screening, but it is not a perfect test. We need to be very upfront with people about that.”
You can bet that’s not the message given to the women getting hounded by the reminder notices. Nor do they get told about the fact that studies show mammograms may actually trigger breast cancer in women with susceptible genes. The study, out of Johns Hopkins in Baltimore, found that women who carry the BRCA gene, which puts them at increased risk for breast cancer early in life, sharply increased their chances of developing cancer if they followed the recommended protocol of having annual mammograms early in life. For every 10,000 women who underwent five mammograms between ages 24 and 29, an extra 26 developed breast cancer. The risk declined as the women aged: between ages 30 and 34, mammograms triggered an extra 20 cancers and an extra 1 for women in their late 30s. The experts say that mammograms would have to reduce breast cancer mortality by 51 percent to counterbalance the risks of the screening for women between the ages of 24 and 29, and they don’t come close, leading to the conclusion that the risks far outweigh the benefits for this age group. And even for older women into their 30s, the benefits appear marginal. In fact, when you combine the increased risks of breast cancer from regular mammograms with the increased risk of cancer from hormone replacement therapy, you come to the unmistakable conclusion that much of the increase we’ve seen in breast cancer in the last 50 years is a direct result of medical intervention. That’s unsettling!
What about those who don’t carry the BRCA gene? At least some experts think mammograms, in addition to being unreliable, pose a danger to all women. The four films shot during a mammogram expose women to 1000 times more radiation than they would get during a chest x-ray. Experts warn that pre-menopausal women increase their risk of cancer by two percent for each mammogram, so a woman having annual screenings over a 10-year period reaps significant exposure to radiation, increasing cancer risk by 10 percent. Also, where early breast cancer exists, the compression applied during the mammogram can disperse cancer cells and make the cancer spread. Plus, studies have shown that the incidence of a common form of breast cancer known as ductal carcinoma in situ (DCIS) has skyrocketed by 328 percent since 1970, with 200 percent of that figure as a direct result of the introduction of mammography. And, mammograms often detect cancers too late, because the tumor grows so fast once detected, or grows too slowly to be detected early enough. In fact, a 2001 study found that “there is no reliable evidence that screening decreases breast cancer mortality — not even a tendency towards an effect.”
The fact is that safer options exist. Instead of mammography, women can have screenings using thermography, which is superior at finding early tumors and at detecting risk. The procedure is relatively safe, though not foolproof, and many insurance companies still won’t pay for it. Still, it’s a relatively cheap procedure averaging about $200, and if you have the money and want to be screened, it’s a less risky option than mammography.
But the truth of the matter is that when it comes to breast cancer, you may have a lot more control of the situation than doctors would have you believe. To learn more, check out Breast Cancer Observations.
:hc









Why don’t you submit this to Washington DC, and have this procedure paid or by the insurance companies now that the Healthcare Reform is being worked on.
If it is cheaper and less invasive for women, why do the insurance companies not want to pay for it?
Wow ! it seems very good to
Wow ! it seems very good to see this post of yours. Terrific work have done by you I like your passion through this post thank..very much.