In this issue of the newsletter, we wrap up our series on the cardiovascular system as we explore blood types and blood tests. Once again, the goal is not to help you graduate medical school, but to help you learn enough so that you are not clueless in your doctor’s office and understand the options (particularly the non-medical ones) that are available to you. Specifically you’re going to learn about:
- The importance of blood type.
- How it affects diet.
- What doctors test for when they check your blood and what the results mean to you.
Blood type
At face value, blood type probably is not that important to you. Its value is primarily to doctors when doing transfusions. But if you scratch below the surface, an exploration of blood type reveals a great deal about the nature of blood and the human organism in general. It also, thanks to the popular blood type diet program, serves as a launching point for a discussion of the proper human diet. With that in mind…
There are two primary systems for classifying blood type: the ABO system and the Rhesus system. They are similar, just governed by different antigens.
ABO system
Your blood type is inherited from your parents. You receive one gene from your mother and one from your father, which combine to establish your blood type. These two genes determine type by causing certain molecules such as sugars, proteins and glycoproteins (a combination of both sugars and proteins) to appear on the surface of your blood cells. The genes also cause defenders that protect against similar (but not identical antigens) to appear in your plasma. These defenders are known as antibodies. Your plasma recognizes your personal glycoprotein/antigens (also known as agglutinogens) as part of your “self,” as belonging in your blood. But the antibodies in your plasma will treat non-identical glycoproteins as allergens and attack the blood, causing the cells to clump together—thus the need to match blood types when getting a transfusion. Let’s explore this concept further.
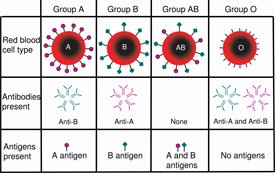
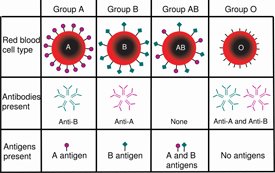 People are divided by blood type into one of four categories: A, B, AB, and O. People with type A blood have the A antigen, while people with type B blood have (surprise) the B surface antigen. Those with blood type AB have both antigens, and type O blood types have no antigens on their surface. Someone with type A blood, for example, will reject a type B blood transfusion because the antibodies in their blood will recognize that the antigens attached to the donated blood are outsiders—not part of the “self.” All blood types can accept type O blood transfusions since it has no antigens on the surface of its blood cells so it doesn’t trigger any antibodies.
People are divided by blood type into one of four categories: A, B, AB, and O. People with type A blood have the A antigen, while people with type B blood have (surprise) the B surface antigen. Those with blood type AB have both antigens, and type O blood types have no antigens on their surface. Someone with type A blood, for example, will reject a type B blood transfusion because the antibodies in their blood will recognize that the antigens attached to the donated blood are outsiders—not part of the “self.” All blood types can accept type O blood transfusions since it has no antigens on the surface of its blood cells so it doesn’t trigger any antibodies.
For more detailed information on ABO blood types and how they get inherited, check out Wikipedia.
Rhesus system
The Rhesus system is the second significant blood group system used in human blood transfusion. Of the different Rhesus antigens found on the surface of blood cells, the primary one is the RhD antigen because it is the most likely to stimulate an immune response in the body. The name Rhesus comes from the type monkey that was used in the first studies that identified this factor. When the Rhesus antigen is present, the blood group is described as positive. When it’s absent, the blood group is described as negative. In other words, you either have, or do not have, the Rhesus factor on the surface of your red blood cells. This means that every ABO blood type has a corresponding positive or negative Rhesus suffix attached, as in:
- Positive—you have the RhD antigen (as in Type O positive).
- Negative—you don’t have it (as in Type AB negative).
Problems
Problems with transfusions are more likely to occur with mismatches in the ABO system than the Rhesus system. If you are exposed to a blood group antigen that is not recognized as belonging in your body, the antibodies in your blood plasma will bind to those blood cells causing them to clump together and die.
A different problem can occur in pregnant women. About 12% of pregnant women carry a fetus with a different blood type from their own (remember, the child’s type is the result of pairing genes from both parents, not just the mother), and sometimes the mother forms antibodies against the red blood cells of the fetus, which can lead to low fetal blood counts, a condition known as hemolytic disease of the newborn, with less than 1% significantly affected. But even at less than 1%, because of the total number of births involved, the numbers of affected children is actually quite large.
Separating out blood’s components
A certain amount of donated blood is actually separated into pieces (fractionated) in order to maximize its benefits and extend shelf life. These pieces/products include:
- Red blood cells
- Plasma
- Platelets
- Clotting factors (Although clotting factors are now mostly synthesized using recombinant DNA techniques to eliminate the risk of disease transmission to hemophiliacs who are dependent on a regular supply of clotting factors.)
The blood type diet
So why are we talking about diet in the middle of a discussion about blood? Well, a couple of reasons. First, people want to know. We receive several dozen questions a month at the Foundation asking what we think of the blood type diet. But more importantly, in answering questions about the diet, we get to explore some of the evolutionary history of blood—which can be very helpful when it comes both to understanding it and optimizing it.
 The premise behind the blood type diet combines the principles of the ABO groupings explained above and the evolutionary theory of blood groups first proposed in the 1950’s. The basic idea is that blood types evolved from the lifestyles and diets of different groups of humanity; therefore, you need to eat the diet natural to the group of humanity from which you are descended. In other words:
The premise behind the blood type diet combines the principles of the ABO groupings explained above and the evolutionary theory of blood groups first proposed in the 1950’s. The basic idea is that blood types evolved from the lifestyles and diets of different groups of humanity; therefore, you need to eat the diet natural to the group of humanity from which you are descended. In other words:
- Type O evolved from early hunters who lived primarily on meat. Thus, type O’s should eat lots of meat.
- Type A came from early farmers. Thus, type A’s should eat mostly a vegetarian diet.
- Type B evolved from nomadic tribes associated with a strong immune systems and flexible digestive systems. This is the only type that can thrive on dairy products.
- Type AB is the most recently evolved type and should eat a cross between the nomadic diet and the vegetarian diet.
So does the diet hold up to scrutiny?
Perhaps, not so much. First, it’s important to remember that the evolutionary theory of blood groups is only a theory that is unlikely to stand the test of time. It turns out that environmental factors probably play a much bigger role in the evolution of blood types and also explain why certain types are concentrated in certain geographical areas.
The evolution of blood types
Nature is filled with trade offs. A person with lots of body fat has insulation in cold latitudes, but sweats unbearably in the tropics. A large muscular person is stronger, better able to fight and conquer, but also requires many more calories to maintain themselves than a smaller person. The same traits have advantages and disadvantages depending upon the circumstances, and so with blood types. Each type is protective against certain diseases and conducive to others.
 As we’ve already discussed, blood types are genetically inherited, but the environment can influence which blood types are passed on. An example is seen with the Black Plague, which killed millions of people in Europe in the 13th and 14th centuries. As it turns out, the Black Plague was caused by a bacterium that is covered by sugar molecules that closely resemble the B marker on red cells. That means that since people who were blood type B back in the plague years didn’t make antibodies to that antigen, they didn’t have any antibodies in place to protect them against the plague. Hence they died in greater numbers than the other blood types which carried the antibodies.
As we’ve already discussed, blood types are genetically inherited, but the environment can influence which blood types are passed on. An example is seen with the Black Plague, which killed millions of people in Europe in the 13th and 14th centuries. As it turns out, the Black Plague was caused by a bacterium that is covered by sugar molecules that closely resemble the B marker on red cells. That means that since people who were blood type B back in the plague years didn’t make antibodies to that antigen, they didn’t have any antibodies in place to protect them against the plague. Hence they died in greater numbers than the other blood types which carried the antibodies.
And, in fact, by the 15th century, fatalities from the plague had decreased significantly as type B blood was systematically phased out in that part of the world. The bottom line is that the distribution of blood types in Europe (low percentages of Type B as opposed to Asia) is not so much the result of diet and occupation, but of natural selection based on disease.
Other examples abound. For example, people with type O blood are susceptible to certain bacteria and viruses that can cause diarrhea and ulcers, but have a decreased susceptibility to SARs. With that in mind, we would expect to see, based on natural selection, a greater concentration of type O blood in Asia, where respiratory diseases such as SARs tend to be more common, than in Europe. And, indeed, such is the case. As you can see, a particular blood type may predispose you to one disease while simultaneously protecting you against another.
Variation in the blood type distribution throughout the world reflects these environmental factors coupled with the tendency of populations to marry and reproduce within their own groups. As people throughout the world intermingle to a greater extent, the distribution of the different blood types is likely to become more uniform throughout the world.
Back to the blood type diet
The evolutionary theory of blood types aside, the cornerstone of the diet is the premise that certain proteins/glycoproteins in food, called lectins, ape the glycoproteins on red blood cells, thus triggering immune reactions from the matching blood type. This premise does not actually require the evolutionary theory to be correct to work. Even if the theory is wrong, the effect can be true. So is it?
Again the answer is probably, not so much.
Yes, there is no question that different foods definitely have high allergy potential for many people, but the problem appears to be less with the lectins, than with the ability of the digestive tract to fully break down the proteins in the food. As I’ve discussed in several newsletters, the use of digestive enzymes with meals and proteolytic enzymes between meals can often help reduce food allergies dramatically.
In fact, there is little evidence that lectins, other than a handful of exceptions such as ricin, present a problem for the human body of any blood type.
But doesn’t it work for some people?
Absolutely!
Simple math works in its favor. If you tell an O, an A, or an AB not to eat dairy because they don’t have the right blood type, then you’ve just told the vast majority of people in the world not to eat dairy. Considering all of the problems associated with homogenized, pasteurized, commercial dairy, a whole lot of people are going to feel significantly better on the diet…regardless of blood type. (Chalk that up in the win column for the diet.) On the other hand, you’ve also just told a lot of Asians (they have the highest percentage of type B’s in the world) that they’ll thrive on dairy. Probably not such a good thing since about 90% of all Asians suffer from lactose intolerance. (And that would need to be chalked up in the loss column.)
Anyway, I’ve detailed my feelings that diet should be based on comparing the teeth, stomachs, and digestive tracts of humans to other animals in Chapter 6 of Lessons from the Miracle Doctors. That kind of comparison will give you a more accurate (make that more objective) read on what the body was actually designed to eat. You can download a free copy at www.jonbarron.org/detox/free-natural-health-book-lessons-miracle.
But enough on the blood type diet. Let’s get back to the issue at hand: blood. More specifically, let’s talk about blood tests—how to understand them and what they mean to you.
Blood tests
Blood tests are the number one tool doctors use to understand the state of your health. Since blood flows throughout your entire body, it picks up bits and pieces of everything and gives clues not only to its own condition, but to the presence of disease in organs such as the liver, kidneys, thyroid, pancreas, and endocrine system.
Since blood tests are so wide ranging, I’m going to limit my discussion in this newsletter to those tests that impact the cardiovascular system itself. We’ll save discussion of enzyme tests for the liver and creatinine tests for the kidneys, and all of the other organ specific tests for later newsletters when we actually focus on those organs and systems. Before we look at some of these tests in detail, it is important to realize that results can fall outside the “normal range” for many reasons that have nothing to do with illness. Age, race, sex, diet, level of exercise, supplements, drugs, etc. can all impact blood test results and move them outside the normal range. In other words, the definition of what is normal is somewhat arbitrary. In fact, most labs set their ranges so that some 5% of healthy people will fall outside the acceptable levels on any given test. Since a normal blood workup will usually include 20-30 tests, falling outside the range on one or two of them does not necessarily indicate a problem—unless other factors are present. It’s also worth noting that the “normal range” is now being “redefined” by the blood test results of ever increasing numbers of people who eat badly, don’t exercise, and are actually very unhealthy. When you consider that sperm counts have dropped by more than half in the last 50 years, falling outside the norm on many tests may not be such a bad thing.
Let’s now take a look at some of the blood tests your doctor runs. Note: I’m not going to give numbers for the most part since they would just be information overload at this time. Instead, I’ll just talk about what high and low numbers might mean. It will be easy enough for you to see where your numbers fall when you get your results back from your doctor.
Complete Blood Count (CBC)
There are actually many tests that can be performed as part of a CBC. In most cases, they should all be done after fasting for at least 12 hours. The most important are:
- Hemoglobin (Hgb) and Hematocrit (Hct): We covered this in the last newsletter . Hematocrit tests reference the number of red blood cells you have. Hemoglobin tests reference the oxygen carrying capacity of those cells. Low numbers suggest anemia. High counts can be suggestive of anything from abnormal bone marrow function to lung disease—or living at high altitudes or athletic blood doping for that matter.
- Platelet Count (PLT): Again, as covered in the last newsletter, platelets are a marker of your body’s ability to initiate blood clots. Low values can be caused by immune system problems, certain cancers, side-effects from drugs, viruses, antigen/antibody problems that cause the platelets to stick together, or even certain B vitamin deficiencies. High platelet counts are often seen in rheumatoid arthritis.
- Mean Corpuscular Volume (MCV): This is a measure of the average red blood cell volume and is used to support a diagnosis of anemia.
- White Blood Count: And once again, as covered in the last newsletter , white blood cells are the front line soldiers in your immune system. High counts are indicative of infection and leukemia. Low counts are indicative of bone marrow and spleen problems.
Electrolytes: These are your potassium, sodium, chloride, and CO2 levels.
- Potassium is controlled very carefully by the kidneys. High levels of potassium are markers for kidney problems, certain medications such as ACE inhibitors, adrenal exhaustion, and excessive use of potassium supplements. Low levels can indicate poor diet, diarrhea, excess water intake, and excessive alcohol consumption.
- Sodium is also regulated by the kidneys and adrenal glands. Low sodium is indicative of diuretic usage, excessive water consumption, and athletic workouts without replacing electrolytes. High levels are often related to dehydration and diet .
- CO2 reflects the acid status of your blood. Low CO2 levels can be due either to increased acidity from uncontrolled diabetes, kidney disease, or high acid forming diets. Low CO2 is a marker for chronic hyperventilation.
Minerals
- Calcium is controlled in the blood by the parathyroid glands and the kidneys. An elevated level is usually associated with parathyroid problems. Excess vitamin D can also be a factor. Low calcium too can be caused by parathyroid problems, drugs like Fosamax and diuretics, and a high acid forming diet (which draws calcium out of the bones to serve as a buffer.
- Phosphorus is also largely stored in the bones. It is regulated by the kidneys, and high levels may be due to kidney disease or parathyroid problems.
Proteins
Albumin and Globulin tests measure the amount and type of protein in your blood. They are a general index of overall health and nutrition. Low gamma globulin levels are seen in people who donate blood too often or have immune system problems. Low albumin may be caused by liver disease, kidney disease, burns, malnutrition, late pregnancy, genetic variations, and even bad posture. High albumin is often caused by dehydration.
Blood fats
These are the tests for cholesterol and triglyceride levels.
- Cholesterol: The overall cholesterol level matters less than the cholesterol ratio of HDL cholesterol to LDL cholesterol. The ratio is obtained by dividing the HDL cholesterol level into the total cholesterol. For example, if a person has a total cholesterol of 200 mg/dL and an HDL cholesterol level of 50 mg/dL, the ratio would be 4:1. The goal is to keep the ratio below 5:1; the optimum ratio is 3.5:1. That said, cholesterol is probably a less significant marker than most doctors believe.
- Triglycerides, on the other hand, are a big deal. Triglycerides are the body’s storage form for fat. They are primarily regulated by the liver. Most triglycerides are found in your body’s fat tissue. Some, however, circulates in the blood to provide fuel for muscles to work. Elevated levels have been associated with heart disease, especially if over 500 mg/dL. High triglycerides are also associated with pancreatitis.
Blood sugar
We’ll cover this in more detail in a future newsletter when we talk about the pancreas, but for now.
- Glucose: This is a measure of the current sugar level in your blood. High values are associated with eating before the test, and diabetes. The normal range for a fasting glucose is 60 -109 mg/dl. Diabetes is diagnosed when you see a fasting plasma glucose of 126 or more. Note: Europeans tend to test for blood sugar just 2 hours after eating, rather than using a fasting level. This tends to increase the number of people who are classified as diabetic.
- A1c (Glycohemoglobin): This test measures the amount of glucose chemically attached to your red blood cells. Once the sugar is attached, it stays there (except under very unusual circumstances) for the life of the cell. That means it doesn’t move up and down multiple times a day and is not dependent on what, or when, you last ate. Since blood cells live about 3 months, it tells us your average glucose for the last 6 – 8 weeks. A high level suggests poor blood sugar control.
Enzymes
Most enzyme tests relate to other parts of the body, particularly the liver, but one—the CPK test—is indicative of heart health.
- CPK is the first enzyme to be elevated after a heart attack (3 to 4 hours). If CPK is high in the absence of heart muscle injury, it’s a strong indication of skeletal muscle disease.
Other cardiac risk factors
- C Reactive Protein (CRP): A high or increasing level of CRP in your blood suggests that you have an acute infection or inflammation. In a healthy person, CRP is usually less than 10 mg/L. High levels also turn out to be a great indicator of heart disease, significantly outperforming LDL cholesterol as a predictor of cardiovascular risk.
- Homocysteine is an amino acid normally found in small amounts in the blood.
High levels of homocysteine are related to the early development of heart and blood vessel disease. In fact, it is considered an independent risk factor for heart disease. High homocysteine is associated with low levels of the methyl donor nutrients: B6, B12, folic acid, trimethylglycine, and SAMe. Methyl groups convert homocysteine, into methionine, which is an essential amino acid. Methylation is inhibited by poor diet (excessive protein and fat intake or inadequate nutrition), alcohol, caffeine, smoking and genetic predisposition. - Lipoproteins are tiny particles that circulate in the blood. They contain cholesterol, fat, and protein in varying amounts depending on the body’s needs. The lipoprotein molecule is similar to LDL cholesterol. Both lipoprotein (a) and LDL are rich in cholesterol and contribute to atherosclerosis of the blood vessels. Test results that show abnormalities in the amounts or kinds of lipoproteins in the blood are predictors of an increased risk of atherosclerosis.
Again, blood tests are wide ranging and can help in determining the health of almost every organ and system in the body. All we covered above are those tests that relect on the health of the cardiovascular system itself. We’ll save the other tests for when we discuss the particular organs and systems in question. The next time your doctor wants to run a blood panel on you, this should give a head start in understanding what he/she is looking for. It should also give you a head start in understanding what you can do about any “odd” results you may get.
Conclusion
That’s it. That finishes our mini-series on the blood and our longer series on the cardiovascular system as a whole. For specifics on how to improve the quality of your blood and the health of your cardiovascular system, you will want to read back over the series, but particularly the last newsletter.
And now for something completely different
Let’s close with a bit of a mindbender—something that takes us out of the mundane world of blood tests and back into the magical world of the body.
Earlier, when we talked about the evolution of blood types, we discussed how nature makes trade offs—how certain blood types can have advantages or disadvantages depending upon circumstances. This also turns out to be true for one of the world’s major blood “disorders”—sickle cell anemia.
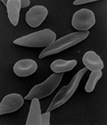 Certain people have a type of blood that appears deflated and shaped like a sickle. People in this group are predisposed to sickle-cell anemia. You might wonder what possible advantages there could be to sickle cell anemia, why nature has chosen to pass this blood “disorder” down through the ages. We certainly know what the disadvantages are, but what possible benefits could there be to sickle cell anemia? And the answer is that deflated, sickle-shaped blood cells actually protect you from malaria. And the very people who possess this type of blood have ancestors who used to live in places where malaria was a major cause of death, such as central Africa. In other words, what we call a genetic disease in the United States and Europe actually started out as a life saving benefit in tropical climates.
Certain people have a type of blood that appears deflated and shaped like a sickle. People in this group are predisposed to sickle-cell anemia. You might wonder what possible advantages there could be to sickle cell anemia, why nature has chosen to pass this blood “disorder” down through the ages. We certainly know what the disadvantages are, but what possible benefits could there be to sickle cell anemia? And the answer is that deflated, sickle-shaped blood cells actually protect you from malaria. And the very people who possess this type of blood have ancestors who used to live in places where malaria was a major cause of death, such as central Africa. In other words, what we call a genetic disease in the United States and Europe actually started out as a life saving benefit in tropical climates.
The body is truly amazing, is it not?
Read more about Cardiovascular Health