The May 19th issue of The Economist ran TWO stories debunking alternative medicine. First, it ran what they call a “Leader.” These are the five or six most important stories of the week that get featured in a special section at the front of the magazine. In this section, the story carried a subheading that read, “Virtually all alternative medicine is bunk.”1”There is no alternative.” 19 May 2011. The Economist. 26 May 2011. <http://www.economist.com/node/18712290> And then later on in the issue, it expounded on the same theme as the main science story of the week, with the subheading, “Alternative medical treatments rarely work. But the placebo effect they induce sometimes does.”2”Think yourself better.” 19 May 2011. The Economist. 26 May 2011. <http://www.economist.com/node/18710090>

Wow!
Personally, I love The Economist, but these stories are way off base and filled with innuendo, not to mention a good bit of distortion. Shame on them! They are normally better than this. Unfortunately, their comments are highly representative of the opinions held by a vast majority of the mainstream medical community, not to mention the media at large. Therefore, they need to be addressed. So, with that in mind, let’s take a look at what they said, why they said it, and why it’s “mostly” a total crock.
Alternative medicine is bunk, but the placebo effect is interesting
The trigger for the articles was the retirement of Edzard Ernst, the world’s “first professor of complementary medicine.” Over the last 18 years, Dr. Ernst and his research team have “pioneered the rigorous study of everything from acupuncture and crystal healing to Reiki channeling and herbal remedies.”
Their conclusion is that:
“Alternative and complementary medicine are mostly quackery…A few treatments (mostly herbs containing active drug molecules) do have proven benefits. A few others look worthy of further investigation. But from acupuncture, via homeopathy, to “quantum healing”, the vast majority, some 95%, offer nothing more than the placebo effect.”
 And:
And:
“According to his “Guide to Complementary and Alternative Medicine”3 Reviewed by Celia Moss. “The Desktop Guide to Complementary and Alternative Medicine: an Evidence-based Approach.” J R Soc Med. 2001 December; 94(12): 650–651. <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1282307/ >, around 95% of the treatments he and his colleagues examined — in fields as diverse as acupuncture, herbal medicine, homeopathy and reflexology — are statistically indistinguishable from placebo treatments. In only 5% of cases was there either a clear benefit above and beyond a placebo (there is, for instance, evidence suggesting that St. John’s Wort, a herbal remedy, can help with mild depression), or even just a hint that something interesting was happening to suggest that further research might be warranted.”
And let me say “Wow” again. If true, this would be hugely disappointing to a lot of people. But in truth, these conclusions are at best misleading and at worst out-and-out incorrect. First, they minimize the impact of herbal remedies by “implying” that they represent only a small part of alternative health and suggesting that the benefits are modest at best. And then they totally dismiss all other forms of alternative treatments as “nothing more than the placebo effect.”
Quite simply, both suppositions are utterly false. Herbal remedies are far and away the largest portion of the alternative health industry, with sales approaching US$60 billion dollars a year worldwide.4Jon C Tilburt, Ted J Kaptchuk. “Herbal medicine research and global health: an ethical analysis.” Bulletin of the World Health Organization. Volume 86, Number 8, August 2008, 577-656. <http://www.who.int/bulletin/volumes/86/8/07-042820/en/> And in some countries, such as Germany, it is estimated that as much as 80% of the population regularly uses traditional herbal medicines.5 Molly Meri Robinson, Xiaorui Zhang. “THE WORLD MEDICINES SITUATION 2011.” World Health Organization. WHO/EMP/MIE/2011.2.3. <http://www.who.int/medicines/areas/policy/world_medicines_situation/WMS_ch18_wTraditionalMed.pdf> It should also be noted that many of the practitioners (acupuncturists, chiropractors, etc.) so quickly dismissed by Dr. Ernst and The Economist, incorporate herbal remedies as part of their practice.
But how effective are herbal remedies? Are they really as minimally effective as Dr. Ernst implies?
According to the Journal of Natural Products,6David J. Newman and Gordon M. Cragg, “Natural Products as Sources of New Drugs over the Last 25 Years.” J. Nat. Prod., 2011, 74 (3), pp 305–309. <http://pubs.acs.org/doi/full/10.1021/np068054v> around 70% of all new drugs introduced in the United States in the past 25 years have been derived from natural herbal products. Some well known drugs that are either herbal based (or were initially discovered in natural sources) include taxol, aspirin, digitalis, quinine, morphine, pseudoephedrine, and vinblastine. In fact, according to the researchers, “half of all anti-cancer drugs introduced since the 1940s are either natural products or medicines derived directly from natural products.”
The bottom line is that not only are many herbal remedies highly effective, but without them, the pharmaceutical industry would barely exist. As Stephen Colbert might say, “A tip of the hat and a wag of the finger.” That’s a tip of the hat to herbal remedies and a wag of the finger to Dr. Ernst for grossly understating their value. (That said, it’s important to understand that the effectiveness of herbs is entirely dependent on the quality of the herbs used, the quantity used (most supplements use too little), and whether or not the herb retains the optimum ratios of bio-actives or has been compromised in the name of standardization.)
But now let’s take a look at some of those “other forms of alternative treatments” that Dr. Ernst refers to as “nothing more than the placebo effect.”
Chiropractic
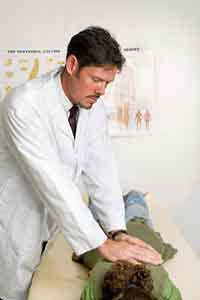 Although Dr. Ernst actually gives some credence to chiropractic — at least as a diagnostic tool, The Economist articles grant it no such legitimacy. But contrary to both opinions, numerous studies have shown that chiropractic treatments really do work. For example:
Although Dr. Ernst actually gives some credence to chiropractic — at least as a diagnostic tool, The Economist articles grant it no such legitimacy. But contrary to both opinions, numerous studies have shown that chiropractic treatments really do work. For example:
A 1991 study conducted by Dr. Paul Shekelle, Director of the Southern California Evidence-Based Practice Center site at the RAND Corporation found that spinal manipulation is safe, effective, and surprisingly well documented in numerous research articles. To quote Dr. Shekelle: “I would say that there’s considerably more randomized controlled trials which show benefit for this (chiropractic care) than there is for many other things which physicians and neurosurgeons do all the time.”7Paul G. Shekelle. “Changing Views of Chiropractic…and a National Reappraisal of Nontraditional Health Care.” Rand Health. RB-4539 (2001). <http://www.rand.org/pubs/research_briefs/RB4539/index1.html>
A 1990 study, conducted at 11 hospitals and chiropractic clinics and published in The Lancet, found that chiropractic treatment of low back pain is superior to the standard regimen administered by medical doctors. And according to T.W. Meade, the doctor who headed the study, “Chiropractic almost certainly confers worthwhile, long-term benefit in comparisons with hospital outpatient management.”8 T.W. Meade, A.O. Frank, Cecily Partridge, Director, Philip Brien and MarkA.P. Cashley. “Chiropractors and low back pain.” The Lancet. Volume 336, Issue 8714, 1 September 1990, Pages 572-573. <http://www.sciencedirect.com/science/article/pii/0140673690921344>
And in 1994, a panel of 23 doctors headed by Dr. Stanley Bigos, MD, Professor of Orthopedic Surgery, studied 3,900 medical articles on low back pain. Their conclusions were that “Chiropractor’s manipulation of the spine was more helpful than any of the following: traction, massage, biofeedback, acupuncture, injection of steroids into the spine, back corsets, and ultrasound.” And “Surgery was beneficial only in 1 out of 100 cases.”9Bigos S., Bowyer O., Braen G., et al. “Acute Low Back Problems in Adults.” Clinical Practice Guideline No.14. AHCPR Publication No. 95-0642. Rockville, MD: Agency for Health Care Policy and Research, Public Health Service, U.S. Department of Health and Human Services, December, 1994. <http://www.ncbi.nlm.nih.gov/books/NBK16662/>
In other words, saying that chiropractic treatments are purely placebo runs contrary to a great deal of scientific evidence. In fact, the biggest problem with chiropractic today is finding a chiropractor that actually still performs real spinal manipulation. Most are now so afraid of law suits that they rely more on “no-touch” techniques or “energy devices” — all less proven than true chiropractic.
Homeopathy
It’s not that there aren’t a lot of studies that support the efficacy of homeopathy — there are. The problem is that all of these studies are automatically dismissed by the medical mainstream because a number of homeopathy’s key concepts are not “consistent with the established laws of science (particularly chemistry and physics).” According to the National Center for Complementary and Alternative Medicine (NCCAM), “Critics think it is implausible that a remedy containing a miniscule amount of an active ingredient (sometimes not a single molecule of the original compound) can have any biological effect — beneficial or otherwise. For these reasons, critics argue that continuing the scientific study of homeopathy is not worthwhile.”10”Homeopathy: An Introduction.” NCCAM Publication No. D439 Created July 2009 Updated August 2010. <http://nccam.nih.gov/health/homeopathy/>
The fundamental problem that scientists have with homeopathy, then, is that it doesn’t make sense to them since most homeopathic remedies are so diluted that no molecules of the original healing substance remain. Ipso facto, according to “science,” any benefit must be a result of the placebo effect. Or as The Economist says, “Ultra-dilute solutions applied to the patients are, by themselves, completely useless.” But that misses the point of homeopathy, and brings up a huge blind spot in the scientific analysis of complementary medicine that nullifies most of science’s conclusions.
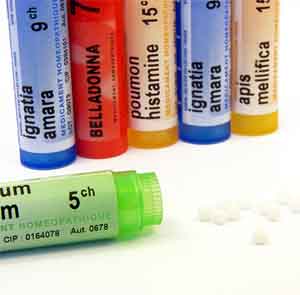 The essence of homeopathy is in the transferring of various substances’ frequencies into water — and then using that water to manifest the properties of the original substance. As I’ve explained in previous newsletters, water can absolutely be “changed” when exposed to electro-magnetic forces and that it can remember those forces for a period of time. We know that energy altered water can significantly change the way irrigated plants grow, for instance. We may not know exactly how water holds this information, but observation and experiment prove that it absolutely does. Based on this fact, you cannot dismiss homeopathy out of hand just because it doesn’t fit into your preconception of what should be. In fact, being ruled by preconceptions is the antithesis of science; it’s dogma. If scientists, and The Economist for that matter, want to evaluate homeopathy, they have to evaluate it on its own terms. You can’t impose your own explanation for how something works and then dismiss it because of the holes found in that explanation. That’s sophistry, and using that technique, you can make light of anything.
The essence of homeopathy is in the transferring of various substances’ frequencies into water — and then using that water to manifest the properties of the original substance. As I’ve explained in previous newsletters, water can absolutely be “changed” when exposed to electro-magnetic forces and that it can remember those forces for a period of time. We know that energy altered water can significantly change the way irrigated plants grow, for instance. We may not know exactly how water holds this information, but observation and experiment prove that it absolutely does. Based on this fact, you cannot dismiss homeopathy out of hand just because it doesn’t fit into your preconception of what should be. In fact, being ruled by preconceptions is the antithesis of science; it’s dogma. If scientists, and The Economist for that matter, want to evaluate homeopathy, they have to evaluate it on its own terms. You can’t impose your own explanation for how something works and then dismiss it because of the holes found in that explanation. That’s sophistry, and using that technique, you can make light of anything.
On the other hand, I’m not necessarily saying that homeopathy works. In my personal experience, I have seen some homeopathic treatments that are literally stunning in their efficacy; but I have seen many more that have no discernible effect at all. But that’s just one person’s observation over time, not a formal study. The key point in this observation, however, is that if even one homeopathic treatment truly works, then it means that there is gap somewhere in mainstream science’s understanding of the world, since it is unable to allow for that efficacy…in even one formula.
Acupuncture
The knock against acupuncture is that skeptics consider the evidence unconvincing since the benefits associated with acupuncture don’t appear to be any different than those associated with placebo effects. They say that larger, more well designed studies using real placebo or sham acupuncture techniques, have increasingly shown that acupuncture does not function any better than placebo in human beings (and sometimes even worse).
And yet…
A couple of years ago, researchers out of Duke University took a comprehensive look at all of the data recorded to date concerning the use of acupuncture for the relief of headache pain. Using only the 31 most rigorously executed studies, they found that acupuncture is more effective than even medication in reducing the severity and frequency of chronic headaches.11 Yanxia Sun, MD and Tong J. Gan, MB, FRCA. “Acupuncture for the Management of Chronic Headache: A Systematic Review.” Anesthesia & Analgesia. December 2008 vol. 107 no. 6 2038-2047. <http://www.anesthesia-analgesia.org/content/107/6/2038.full> 62%of the acupuncture patients reported headache relief compared to only 45% of people taking medication. Amusingly, then, the study found no correlation between the effectiveness of acupuncture and placebos, but rather a correlation between medication and placebos. In comparative studies, both the placebo groups and the medication groups had the same percent of responders improving — forty-five percent. Acupuncture, on the other hand, showed a significant benefit over both medication and placebos as a treatment choice. It should be noted that the study also found that correct technique is important as well. Sham acupuncture, which was done on parts of the body not associated with the ancient Chinese principles, was less effective than traditional acupuncture.
And then of course, there are the surgeries that have been performed using acupuncture as the analgesic of choice. Watch for yourself. We’re talking one heck of a placebo effect in this video.
Magnetic therapy
The Economist also refers to magnetic therapy as “completely useless.” Again, as with homeopathy, this is a prejudicial pronouncement. The problem is not that magnetic therapy is not supported by studies (it is), but rather, according to NCCAM, no scientific theory about “how magnets might work” has been conclusively proven. Once again, as with homeopathy, since the mechanisms by which magnets might affect the human body are not yet known, any studies supporting their efficacy are invalid ipso facto. (As we will discuss a little later, this kind of logic actually represents a huge double standard within the medical community.)
In addition, according to NCCAM, researchers face challenges when studying magnets in clinical trials:
- Something other than the magnet may relieve a study participant’s pain. For example, relief could come from a placebo effect or from a warm bandage or cushioned insole that holds the magnet in place.
- It can be difficult to design a sham magnet that participants cannot distinguish from an active magnet. If participants know whether they are using an active magnet, study findings may be less reliable.
- It is possible that the magnetic properties of low-strength magnets, which are sometimes used as shams, can actually have a therapeutic effect.
- Opinions differ about how to administer magnet therapy, including what strength magnet to use, where to place the magnets on the body, and how long to use them. These factors have not been fully studied in humans. Clinical trials that look at these factors are needed.
 So again, it’s not that magnets have not demonstrated beneficial results in some studies; it’s that those studies must be rejected by definition. That makes for a rigged game.
So again, it’s not that magnets have not demonstrated beneficial results in some studies; it’s that those studies must be rejected by definition. That makes for a rigged game.
In truth, the scientific community is continually confirming the effect of magnets on the human body — even if they still struggle with the theory as to why they work. For example: according to the Harvard Gazette, researchers at Harvard Medical School are experimenting with a technique that uses electromagnetic pulses to treat depression. Called transcranial magnetic stimulation, or TMS, it involves holding a figure-of-eight-shaped wand near a person’s head. Two coils of wire on the wand generate a strong magnetic field that induces electric currents in brain cells. “We believe that TMS works by normalizing disturbed levels of brain activity,” says Alvaro Pascual-Leone, an associate professor of neurology at Harvard Medical School. In experiments at Beth Israel Deaconess Medical Center in Boston, he and his colleagues lifted the spirits of depressed patients who are resistant to anti-depressant drugs.12William J. Cromie. “Depressed get a lift from MRI.” Harvard University Gazette. January 22, 2004. <http://www.news.harvard.edu/gazette/2004/01.22/01-depression.html> Even better, clinics have since opened at major hospitals around the country featuring TMS for treating depression.13”TMS Therapy Comes to Los Angeles.” UCLA Depression Research & Clinic Program. 24 May 2011. <http://www.tmslosangeles.com/>
And then there’s the MIT study published in The Proceedings of the National Academy of Scientists that discovered that by applying a magnet to a subject’s head, researchers could alter that person’s moral judgment, almost instantly. According to the lead researcher, “To be able to apply (a magnetic field) to a specific brain region and change people’s moral judgments is really astonishing.”
But Dr. Joshua Greene of Harvard University thought that it was anything but astonishing, “Moral judgment is just a brain process. That’s precisely why it’s possible for these researchers to influence it using electromagnetic pulses on the surface of the brain.”
So why is it that when magnetic therapy is used for pain relief, it’s a placebo, and when it’s used by medical doctors to treat depression and alter moral judgment it’s “science?” Oh yes, of course. Silly me! Its use in pain relief is by alternative health practitioners.
Huge amounts of money are wasted on nonsense
One of the biggest problems The Economist has with alternative health is the amount of money wasted on nonsense. “Globally, the industry is estimated to be worth some $60 billion a year. That is a lot to pay for placebos.” However, as we’ve already seen, despite Dr. Ernst’s conclusions, the money is not necessarily wasted. And even if that money is being spent on placebos, what’s the complaint — at least it’s producing a beneficial result with minimal chance of a catastrophic side effect. Can the same be said for modern medicine?
I have explained on numerous occasions how modern medicine is far less scientific than you think — and how many of the benefits attributed to highly dangerous surgical techniques and pharmaceutical drugs are the result of the placebo effect. Here are just a few examples of money wasted on “medical science.”
 Statin drugs
Statin drugs
In January of 2008, I wrote about the results from a study sponsored by Merck and Schering-Plough that found that after several years on two types of cholesterol-lowering medications, patients reduced their cholesterol level, but they reaped no significant health benefit at all unless they already had heart disease. (Note: Merck delayed releasing the results for two years, and only when finally pressed to do so.) Worldwide this ineffective class of drugs accounts for revenues exceeding $26 billion in 2008 alone. And they are hardly without risk, having been associated with a 50% increased risk of cancer of all kinds, structural damage to muscles, and cataract and kidney risk.14Michelle Fay Cortez. Cholesterol-Cutting Statin Drugs Raise Cataract, Kidney Risk in U.K. Study. 20 May 2010. Bloomberg. 24 May 2011. <http://www.bloomberg.com/news/2010-05-20/cholesterol-cutting-statin-drugs-raise-cataract-kidney-risk-in-u-k-study.html>
Angioplasty
And then of course, there’s angioplasty. In 2007, researchers found that angioplasty did not save lives or prevent heart attacks in non-emergency heart patients. According to the study, angioplasty gave only slight and temporary relief from chest pain, the main reason it’s done. “By five years, there was really no significant difference” in symptoms. And how much money is spent on this dangerous procedure that produces such minimal benefits? Every year in the US, doctors perform about 1.2 million angioplasties at an average cost of $40,000. That works out to $48 billion wasted every year in the US alone — just on this one medical procedure!!!!
Antidepressants
 And then there are the multiple studies, such as the one published in PloS Medicine,15Irving Kirsch, Brett J. Deacon, Tania B. Huedo-Medina, et al. “Initial Severity and Antidepressant Benefits: A Meta-Analysis of Data Submitted to the Food and Drug Administration.” PLoS Medicine. February 2008. (http://www.plosmedicine.org/article/info%3Adoi%2F10.1371%2Fjournal.pmed.0050045> that have shown that the best selling antidepressants don’t work much better than placebos for many depressed patients. The researchers came to their conclusions by examining not only published studies but also unpublished data submitted to the FDA. Curiously, the FDA had decided not to publish any of the negative data. Naturally, there was a response published in the New England Journal of Medicine arguing that doctors and patients may not have been able to see the full antidepressant picture. Well, that certainly explains away the results in a scientific manner! But my favorite comment was quoted by the study’s lead author in a subsequent article published in the McGill Journal of Medicine, discussing the blowback the researchers had received from their study equating the efficacy of antidepressant drugs to placebos. “Finally, some have argued that even if the drugs don’t work, it was wrong of my colleagues and me to publish our studies. We shouldn’t tell patients that the drugs don’t work because it will undermine their faith in treatment.”16Irving Kirsch. “Challenging Received Wisdom: Antidepressants and the Placebo Effect.” Mcgill J Med. 2008 November; 11(2): 219-222. <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2582668/>
And then there are the multiple studies, such as the one published in PloS Medicine,15Irving Kirsch, Brett J. Deacon, Tania B. Huedo-Medina, et al. “Initial Severity and Antidepressant Benefits: A Meta-Analysis of Data Submitted to the Food and Drug Administration.” PLoS Medicine. February 2008. (http://www.plosmedicine.org/article/info%3Adoi%2F10.1371%2Fjournal.pmed.0050045> that have shown that the best selling antidepressants don’t work much better than placebos for many depressed patients. The researchers came to their conclusions by examining not only published studies but also unpublished data submitted to the FDA. Curiously, the FDA had decided not to publish any of the negative data. Naturally, there was a response published in the New England Journal of Medicine arguing that doctors and patients may not have been able to see the full antidepressant picture. Well, that certainly explains away the results in a scientific manner! But my favorite comment was quoted by the study’s lead author in a subsequent article published in the McGill Journal of Medicine, discussing the blowback the researchers had received from their study equating the efficacy of antidepressant drugs to placebos. “Finally, some have argued that even if the drugs don’t work, it was wrong of my colleagues and me to publish our studies. We shouldn’t tell patients that the drugs don’t work because it will undermine their faith in treatment.”16Irving Kirsch. “Challenging Received Wisdom: Antidepressants and the Placebo Effect.” Mcgill J Med. 2008 November; 11(2): 219-222. <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2582668/>
Okay, Economist, where’s the science in that statement? I guess different rules apply to “science based medicine” than you and Dr. Ernst call for when dealing with alternative therapies. By the way, how much do we pay for all this placebo-like efficacy provided by antidepressants? According to some estimates, it works out to about $12 billion a year, or about $120 billion over ten years — in the United States alone.
The bottom line is that if your concerns are wasted money and danger, then you have far more to look at in the medical community than in the world of holistic medicine.
Is alternative medicine scientific?
The Economist states: “The world’s advertising-standards offices should thus crack down on bogus claims — including the idea that there is such a thing as “alternative medicine” in the first place. If it works, it is a medicine and should be regulated like one. If it doesn’t work, it isn’t a medicine.”
This is actually one of the most disturbing statements in The Economist articles. I suppose I could give the sarcastic response and say that the alternative health industry would love to be able to make the same claims that antidepressant drugs do on television, have doctors prescribe them to millions of patients, have insurance companies pick up the tab, and get paid outrageous amounts of money per prescription — all for something that performs the same as a placebo. Yes, I’m all in favor of having those high “medicine” standards applied to alternative health. Unfortunately, although it feels good, sarcasm doesn’t really get us anywhere.
Instead, I would like to talk about the more important issue underlying The Economist’s statement — and in fact, the articles as a whole — that there is a single scientific method that must be applied equally to all forms of healing. Quite simply, that is utter nonsense. In fact, medicine and alternative healing have diametrically opposite approaches to health and therefore need to be evaluated in diametrically opposite (but equally scientific) ways. I have covered this issue many times before, but needs demand I repeat it yet again.
Subtractive Vs Additive
Medicine is “subtractive” by definition. All drug development, all drug patents, all efficacy testing are designed to reinforce this concept. By subtractive, I mean that all medicine is based on the idea that you need to “subtract” out anything that is irrelevant until you can isolate out the “one thing” left that “works.”
For example, the star anise plant has a long history as a healing herb — for digestive problems, women’s health, and for treating colds and flus. The Swiss pharmaceutical company, Roche, focused in on the cold and flu benefit and then “subtracted out” all of the “extraneous” biochemicals in the plant until they settled on one component, shikimic acid, that they said was responsible for the star anise plant’s ability to help with colds and flus. From shikimic acid, they synthesized oseltamivir (for patent purposes), and thus was born Tamiflu. This is the subtractive process. You eliminate everything “extraneous” and get down to the one single active ingredient. (Of course, there are major problems with the magic bullet approach — in this case, that Tamiflu doesn’t really work that well and that flu viruses are easily able to mutate around the single magic bullet ingredient in Tamiflu.)
In any case, everything in medicine is built around the “subtractive” concept. Drugs, such as Tamiflu, are developed using it. Patents are issued based on it. And all drug testing depends on it. But this is not the only way, nor necessarily the best way, to develop and test effective treatments. You can, for example, try an “additive” approach. This is the approach used by most holistic treatments. Instead of using a single “drug,” most alternative therapies involve multi-part protocols (combining diet, supplements, treatments, etc.). Alternative practitioners don’t care which component does what, or even if one or more of the components ultimately prove to be non-essential, as long as the overall protocol itself produces the desired result. This approach makes medical doctors apoplectic. For doctors, it doesn’t matter if an alternative treatment produces clear results. If you can’t isolate it down to a single component and explain exactly why it does what it does (in a way that fits within already defined scientific parameters), then “results be damned.” The therapy cannot work — even if the results might indicate it does. This leads to some bizarre contradictions when it comes to testing alternative therapies.
 It is at this point in the discussion that I usually dust off my football (American style) analogy for trying out a rookie quarterback by putting him on the field with no one else playing offense. The “alternative approach,” of course, would be to put him on the field with an entire team and see how he plays. If he scores, if he leads the team to victory, if he wins the Super Bowl, we would say he is a good quarterback. To many people, that would seem to make sense — unfortunately, not to the medical community.
It is at this point in the discussion that I usually dust off my football (American style) analogy for trying out a rookie quarterback by putting him on the field with no one else playing offense. The “alternative approach,” of course, would be to put him on the field with an entire team and see how he plays. If he scores, if he leads the team to victory, if he wins the Super Bowl, we would say he is a good quarterback. To many people, that would seem to make sense — unfortunately, not to the medical community.
The “medical approach” is quite different. “How can we really tell if he’s any good if there are other players on the field? Great receivers could catch lousy passes, and we’d never know. A great offensive line could make the quarterback look good by blocking so well that he has all the time in the world to find his receivers. No! The only way to truly tell if he’s any good is to put him on the field alone against an entire all-pro defensive team, and then see how he does.” And, of course, the moment the ball is hiked, he’s swarmed over and killed.
This approach to testing, of course, is equally absurd when evaluating an alternative health protocol, which like a football team, is additive by nature. An alternative treatment that was part of a protocol would be dismissed as ineffective if testing showed it to be only 10% effective in isolation. And yet, it might actually be an invaluable part of a comprehensive holistic program that contained seven such 10% components — giving you a 70% chance of overcoming your illness. Or the component might have zero benefit by itself but serve to make another component ten times more effective than it would be if used by itself. Unfortunately, the medical establishment deliberately chooses not to test alternative therapies in this way — thus condemning all seven components to bear the “quackery” label. So the only way you hear about effective alternatives is by word of mouth or anecdotal evidence. Fortunately, the effectiveness of some of these programs is so strong that it is impossible, even for The Economist, to suppress their success.
So how do drugs pass this kind of testing? How do they do it? Quite simply, drugs are designed to be “magic bullets.” Returning to our football analogy, we can indeed put our quarterback out on the field all alone to test his skills — but this time armed with an AK-47 assault rifle. As soon as the ball is hiked, he shoots the entire defensive team and walks across the goal line. He wins! Unfortunately, although he scores, there are side effects (like with most pharmaceutical drugs). The other team (the patient, if you will) is dead and the game is over — but he did score (he didn’t die from the cancer, just the side effects of the chemotherapy).
Just like football is a team game (with the team only as strong as its weakest link) so too are most holistic protocols. On occasion, you may get good results using just one component or another, but overall, you will get the best results when you run the program as a whole. To isolate components of a program out from the whole is to treat them as drugs. That’s not what they are, and they will fail that test by definition.
The Economist concludes this part of the discussion by stating, “Whenever scientifically challenged celebrities, such as the Prince of Wales, waffle on about it in ways that suggest it is outside the realm of scientific scrutiny, they too should be denounced by academics and proper doctors.”
But in fact, what the “scientifically challenged celebrities” are talking about (badly as it turns out) is this fundamental difference in paradigm between alternative therapies and medicine — additive VS subtractive. It doesn’t mean that alternative therapies can’t be tested scientifically; it just means that you have to use a different methodology that recognizes that difference. Quite simply, all you have to do is change the order of testing. Instead of eliminating everything from the get-go and testing each piece of a holistic protocol in isolation, one at a time, start by testing the entire protocol as a whole without worrying about what part does what. Verify that the protocol as a whole works, then start removing pieces one at a time to see which parts are essential and which parts are not. Then you can figure out which of the components need to be present.
And to be sure, when tested this way, many alternative therapies and supplements, as currently offered, will turn out to be totally ineffective, but at least they will have been evaluated properly, on their own terms. I fully understand that much of what is available in the world of holistic medicine is pure woo woo claptrap, but then, as we’ve already seen, so are many “accepted” medical treatments. Beyond that, though, it also needs to be understood that much that “appears” to be woo woo claptrap actually works — just not for any reason currently understood…by anyone. That doesn’t mean it doesn’t work, or can’t work…just that we don’t yet know why it works. Our “science” is not yet wise enough to understand it. But is that really any different than much of medicine? Take electroconvulsive therapy (aka electroshock therapy) which has been around since the 1930’s. No one knows for sure why it does what it does — only that it does it. There are theories, of course, that have appeared and been discarded over the years. And yet, with no understanding of why it works, electroconvulsing continues apace as an accepted part of science-based medicine. Why is that less woo woo than homeopathy, Economist?
In addition, I am not opposed to regulation and oversight for alternative health treatments. Indeed, I think it’s absolutely necessary. However, what I do question is who is doing the regulating. Expecting medical doctors and government agencies run by medical doctors to give a fair hearing to alternative therapies is like asking American football owners to oversee world soccer. Yes, they’re both games and both played with balls, but American football owners (as a rule) don’t understand soccer, don’t particularly like it, and in fact view it as a competitor (both for money and athletic talent) — to be kept marginalized and, as much as possible, outside the country. If alternative health is to be regulated, it needs to be regulated by those who understand it…and appreciate it.
Conclusion: placebo benefits
The Economist articles can essentially be summarized in the following quote:
 “That [the conclusion that most alternative therapies are quackery] should not, however, blind those proper doctors to the one thing, among all the claptrap, the so-called alternative does have to offer. Placebos can bring relief, especially from nerve-related problems like pain and depression. They may also reach further than that. There is growing evidence that the strength of a person’s immune system is affected by his mental state, too: a healthy mind really does count, especially in an unhealthy body.”
“That [the conclusion that most alternative therapies are quackery] should not, however, blind those proper doctors to the one thing, among all the claptrap, the so-called alternative does have to offer. Placebos can bring relief, especially from nerve-related problems like pain and depression. They may also reach further than that. There is growing evidence that the strength of a person’s immune system is affected by his mental state, too: a healthy mind really does count, especially in an unhealthy body.”
And if you throw out the quackery and placebo parts of their analysis, they are absolutely right. Holistic medicine deals, by definition, with the whole body — including the mind. Science based medicine, since it is defined by subtractive reductionism, does not. Therefore, holistic medicine will indeed, in some cases, outperform traditional medicine. Ultimately, then, The Economist articles do a terrible job at trying to brand alternative therapies as quackery. Despite the work of Dr. Ernst, alternative therapies actually hold up quite well to scientific scrutiny…if you choose to evaluate them on their own terms. On the other hand, the articles do a much better job at pointing out the ultimate failure of science based medicine — that it views the body as a series of independent parts rather than as an integrated whole — including what we think. And for pointing that out, we ultimately owe The Economist a hearty, “Quack! Quack!”
References
| ↑1 | ”There is no alternative.” 19 May 2011. The Economist. 26 May 2011. <http://www.economist.com/node/18712290> |
|---|---|
| ↑2 | ”Think yourself better.” 19 May 2011. The Economist. 26 May 2011. <http://www.economist.com/node/18710090> |
| ↑3 | Reviewed by Celia Moss. “The Desktop Guide to Complementary and Alternative Medicine: an Evidence-based Approach.” J R Soc Med. 2001 December; 94(12): 650–651. <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1282307/ > |
| ↑4 | Jon C Tilburt, Ted J Kaptchuk. “Herbal medicine research and global health: an ethical analysis.” Bulletin of the World Health Organization. Volume 86, Number 8, August 2008, 577-656. <http://www.who.int/bulletin/volumes/86/8/07-042820/en/> |
| ↑5 | Molly Meri Robinson, Xiaorui Zhang. “THE WORLD MEDICINES SITUATION 2011.” World Health Organization. WHO/EMP/MIE/2011.2.3. <http://www.who.int/medicines/areas/policy/world_medicines_situation/WMS_ch18_wTraditionalMed.pdf> |
| ↑6 | David J. Newman and Gordon M. Cragg, “Natural Products as Sources of New Drugs over the Last 25 Years.” J. Nat. Prod., 2011, 74 (3), pp 305–309. <http://pubs.acs.org/doi/full/10.1021/np068054v> |
| ↑7 | Paul G. Shekelle. “Changing Views of Chiropractic…and a National Reappraisal of Nontraditional Health Care.” Rand Health. RB-4539 (2001). <http://www.rand.org/pubs/research_briefs/RB4539/index1.html> |
| ↑8 | T.W. Meade, A.O. Frank, Cecily Partridge, Director, Philip Brien and MarkA.P. Cashley. “Chiropractors and low back pain.” The Lancet. Volume 336, Issue 8714, 1 September 1990, Pages 572-573. <http://www.sciencedirect.com/science/article/pii/0140673690921344> |
| ↑9 | Bigos S., Bowyer O., Braen G., et al. “Acute Low Back Problems in Adults.” Clinical Practice Guideline No.14. AHCPR Publication No. 95-0642. Rockville, MD: Agency for Health Care Policy and Research, Public Health Service, U.S. Department of Health and Human Services, December, 1994. <http://www.ncbi.nlm.nih.gov/books/NBK16662/> |
| ↑10 | ”Homeopathy: An Introduction.” NCCAM Publication No. D439 Created July 2009 Updated August 2010. <http://nccam.nih.gov/health/homeopathy/> |
| ↑11 | Yanxia Sun, MD and Tong J. Gan, MB, FRCA. “Acupuncture for the Management of Chronic Headache: A Systematic Review.” Anesthesia & Analgesia. December 2008 vol. 107 no. 6 2038-2047. <http://www.anesthesia-analgesia.org/content/107/6/2038.full> |
| ↑12 | William J. Cromie. “Depressed get a lift from MRI.” Harvard University Gazette. January 22, 2004. <http://www.news.harvard.edu/gazette/2004/01.22/01-depression.html> |
| ↑13 | ”TMS Therapy Comes to Los Angeles.” UCLA Depression Research & Clinic Program. 24 May 2011. <http://www.tmslosangeles.com/> |
| ↑14 | Michelle Fay Cortez. Cholesterol-Cutting Statin Drugs Raise Cataract, Kidney Risk in U.K. Study. 20 May 2010. Bloomberg. 24 May 2011. <http://www.bloomberg.com/news/2010-05-20/cholesterol-cutting-statin-drugs-raise-cataract-kidney-risk-in-u-k-study.html> |
| ↑15 | Irving Kirsch, Brett J. Deacon, Tania B. Huedo-Medina, et al. “Initial Severity and Antidepressant Benefits: A Meta-Analysis of Data Submitted to the Food and Drug Administration.” PLoS Medicine. February 2008. (http://www.plosmedicine.org/article/info%3Adoi%2F10.1371%2Fjournal.pmed.0050045> |
| ↑16 | Irving Kirsch. “Challenging Received Wisdom: Antidepressants and the Placebo Effect.” Mcgill J Med. 2008 November; 11(2): 219-222. <http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2582668/> |










Sir: Thank you for the BEST
Sir: Thank you for the BEST explanation of alternative (holistic) medecine..vrs traditional medicine. Quack Quack
From the state of the
From the state of the economy, it is apparent that the dogma and theories of practicing economists neither produced a healthy economy, nor healed a sick one. Now these people want to tell health practitioners how to maintain and heal human bodies? How funny is that?! Their article merits a different version of a classic response: “Economist, heal thyself.” When some people cannot do their own work well, they go to unusual efforts to criticize others’ work. Health and medicine are far outside economists’ expertise. Any benefit from their article would be very much a placebo effect.
O sure, "Economist". After
O sure, “Economist”. After billions of years, nature doesnt know what she’s doing.
Uh-huh. O btw, your wallet is showing.
I could not have written it
I could not have written it so eloquently, but it expresses my sentiments and understanding of the two faces of health therapy exactly.
Thanks!!
Ralph Watson
Thank you Jon, excellent
Thank you Jon, excellent article. For those interested in the state of modern “scientific” medicine I enthusiastically recommend this long but insightful article from The Atlantic.
http://www.theatlantic.com/magazine/archive/2010/11/lies-damned-lies-and-medical-science/8269/
Hi Jon, One would think that
Hi Jon, One would think that with all the fines, due to wrong information, people would realise that the medical branch need to put their own house in order, before criticising others.
Doctors and surgeons perform miracles, but cannot help trying to grab it all, wanting also to treat problems that are best left to alternative therapists.
While treating a patient with reflexology, I have advised them to go immediately to the hospital to check. On one occasion, I learnt later, that another day, and he would have probably died. The consultant wanted to how I knew!
I absolutely loved the
I absolutely loved the article, very informative. However, I must take exception to your terminology. What M.D.s and the modern conventional medical industry practice is modern and/or conventional medicine. The term they use to marginalize traditional therapies is CAM (complementary and alternative medicine). By referring to traditional therapies as CAM we marginalize ourselves.
The article would be credible
The article would be credible if they had shown that synthetic medicines had cured diseases that the science of modern medicine consider incurable.
Those diseases remain incurable to their methodologies because they insist on using them on sick people who had firmly believed every lie that drug manufacturers and so-called medical professionals had untiringly told them for reasons that are too obvious.
Sir: Thank you for this
Sir: Thank you for this explination. May I add, that with the new understanding of epigenitics and the introduction of bichemical tests for systemic change, it is now possible to test all forms of medicine with the same scientific method.
from your article it is
from your article it is almost impossible what is best foor any given individual. to solve this problem , for 20 years i have used a pendulum to decide what is good or bad for me and my wife. it saves a lot of mony and making bad choices. i have found it to be about 95% accurate.
Once again–as always, from
Once again–as always, from my perspective anyway–you have written a most articulate, knowledgeable and honest explanation in answer to big questions regarding the state of healthcare/health maintenance. I have not read the article in the Economist, but having read similar drivel in other mainstream publications about holistic healing I’m sure I would have been shaking my head over their negative portrayal of ages old, traditional medical practice. I just wish that anyone reading such crap would be able to see it in the same way. Unfortunately, there is still so much ignorance in the general public.
To be talking about something as important as health care and SCIENCE you would think that the writer would have done better RESEARCH.
Thanks Jon for giving us so much of your time and attention to detail.
Willow bark was also used to
Willow bark was also used to calm an acidic stomach as well as for pain relief, unfortunately the active isolate taken from the willow bark called aspirin actually causes stomach acid to rise, I found that whereas apirin would make me throw up willow bsark doesn’t
typical media medical
typical media medical propaganda we see every day.
the big nail in their coffin is vitamin C for infections, and you will notice they never EVER mention it, as there are 1,200 citations backing up it’s use JUST FOR INFECTIONS AND POISONS that Dr Levy documents in his book.
Just that ONE Vitamin would SINK vaccination and allopathy.
Vitamin C, Infectious Diseases, and Toxins: Curing the Incurable by Thomas E. Levy, M.D., J.D.
“Many viral infectious diseases have been cured and can continue to be cured by the proper administration of Vitamin C. Yes, the vaccinations for these treatable infectious diseases are completely unnecessary when one has the access to proper treatment with vitamin C. And, yes, all the side effects of vaccinations…are also completely unnecessary since the vaccinations do not have to be given in the first place with the availability of properly dosed vitamin C.”—Dr Thomas Levy M.D., J.D. (Vitamin C, Infectious Diseases and Toxins p30)
“Amazingly, vitamin C has actually already been documented in the medical literature to have readily and consistently cured both acute polio and acute hepatitis, two viral diseases still considered by modern medicine to be incurable.” – Thomas E. Levy, MD, JD
All three children had different doctors. The little girl under Klenner’s care was given 10,000 mg of vitamin C as a slow intravenous “push” with a 50 cc syringe every eight hours for the first 24 hours and then every 12 hours for two more doses. Following this she was given 1,000 mg of vitamin C every two hours by mouth. Klenner also notes that a 40,000-unit dose of antitoxin was injected into the little girl’s abdomen. The other two children received the antitoxin as well, but they did not receive any vitamin C. They both died but Klenner’s patient survived, later becoming a nurse. —Vitamin C, Infectious Diseases, and Toxins: Curing the Incurable by Thomas E. Levy, M.D., J.D.
“Acute viral hepatitis…is easily and completely curable with treated promptly with adequate doses of vitamin C …some evidence indicates that a high dose of vitamin C for a long enough period of time would probably resolve (chronic hepatitis) as well in many of the cases…….A significant benefit of properly dosed vitamin C would be the elimination of any need or reason to vaccinate people against hepatitis.”—Dr Thomas Levy M.D., J.D. (Vitamin C, Infectious Diseases and Toxins pgs 60, 66)
Great article as usual, Jon,
Great article as usual, Jon, but this passage in your quarterback analogy has zinged me too many times that I have to point out the mathematical error:
“An alternative treatment that was part of a protocol would be dismissed as ineffective if testing showed it to be only 10% effective in isolation. And yet, it might actually be an invaluable part of a comprehensive holistic program that contained seven such 10% components — giving you a 70% chance of overcoming your illness.”
Although your point stands anyway, it is not the case that adding seven 10%-effective components is 70% effective. If that were the case then taking ten of those components would be 100% effective, but of course that is not how it is. Hence the whole “additive” notion, taken as literally adding percents, is misleading. Better just to say it is additive and that combining many components that are 10% effective will add up to far more than a 10% total effect. This is just something the allopaths would make fun of or use to dismiss this otherwise outstanding refutation.
Hi Amano,
As you say, it is
Hi Amano,
As you say, it is an analogy, not a literal congruency. And yes, there are many variables such as duplicated efficacies that could make the overall efficacy less than 70%. But keep in mind, there might be synergies that make the overall efficacy higher than 70% — even 100%. In any case, point taken, and we will pass it along to Jon.