- Exactly what is a virus, and how does it infect you?
- How does your immune system defend against viruses?
- How does your body know how to respond?
- What is interferon; what does it do; and what harm can it cause?
- How can you boost your immune system to prepare for the coronavirus?
- How to use an antipathogenic formula to support your body when you eventually come down with the virus.
How many times do you need to hear that you have to wash your hands, stay at home, and practice social distancing to defend against COVID-19? In fact, for a quick update, you can go back to the two newsletters I wrote last month.
- COVID-19: There’s No Need for Panic (3/12/20)
- More than Everything You Ever Wanted to Know about the New Coronavirus (2/27/20)
They still stand as accurate predictors of where we are today, with two small corrections.
- At the time, I said that the mortality rate would likely settle in at around 0.7%. As it turns out, we’re not there yet. In fact, the “official” mortality rate varies widely by country and is higher than I projected. In countries with at least 1,000 deaths, the mortality rate is as low is 2.1% in Turkey and 2.5% in Germany. But it’s as high as 12.8% in Belgium and Italy. The US mortality rate is 4.1%, and the global average is disturbingly high at 6%. But keep in mind, the official number may not be an accurate number. It’s calculated by setting the number of deaths against the number of tested and confirmed cases. For example, if 100 people are confirmed as having the virus and 5 of them eventually die, that’s a 5% mortality rate.
 But that doesn’t factor in all those people who never had any symptoms, mild symptoms, or flu-like symptoms they dealt with at home and so were never tested for the virus—and are thus not part of the official statistics. Considering that fewer than 1% of people have been tested in the U.S., the actual number of people who have had the virus could easily be four or five times higher than the official number, or more. Going back to our example, that would mean 5 deaths out 500 people who actually were infected VS the 100 who were officially tested. And that would mean a mortality rate of just 1%. But keep in mind that since the virus is brand new to the world, unlike the flu, no one anywhere on the planet has any immunity to it. Social distancing doesn’t change that. Ultimately, everyone in the world is potentially susceptible—and will remain so no matter how long they self-quarantine at home. That said, a low mortality rate applied to a large number of people is still a large number of deaths—eventually.
But that doesn’t factor in all those people who never had any symptoms, mild symptoms, or flu-like symptoms they dealt with at home and so were never tested for the virus—and are thus not part of the official statistics. Considering that fewer than 1% of people have been tested in the U.S., the actual number of people who have had the virus could easily be four or five times higher than the official number, or more. Going back to our example, that would mean 5 deaths out 500 people who actually were infected VS the 100 who were officially tested. And that would mean a mortality rate of just 1%. But keep in mind that since the virus is brand new to the world, unlike the flu, no one anywhere on the planet has any immunity to it. Social distancing doesn’t change that. Ultimately, everyone in the world is potentially susceptible—and will remain so no matter how long they self-quarantine at home. That said, a low mortality rate applied to a large number of people is still a large number of deaths—eventually.
- Back then I also mentioned that there was the possibility that warmer summer months might slow the virus’s progression, as it does with most flu viruses. That’s probably not true. Accumulating evidence indicates that COVID-19 is unaffected by seasonal temperature changes. What is slowing it down, however, is the worldwide lockdown. But as I mentioned, at the time, a general lockdown without sufficient testing may slow the virus, but it still leaves massive numbers of people susceptible to infection the moment they end their self-enforced quarantine. Then again, brand new evidence indicates that I might have been right in the first place as the most recent government lab experiments (not yet validated) show that the coronavirus does not survive long in high temperatures and high humidity, and is quickly destroyed by sunlight.1 Jana Winter and Sharon Weinberger. “Sunlight destroys virus quickly, new govt. tests find, but experts say pandemic could last through summer.” Yahoo News April 17, 2020. (Accessed 17 April 2020.) https://www.yahoo.com/news/sunlight-destroys-coronavirus-very-quickly-new-government-tests-find-but-experts-say-pandemic-could-still-last-through-summer-200745675.html
Anyway, as I said, who needs to hear yet again that they need to wash their hands, stay at home, and practice social distancing? So, in this newsletter, I want to do something different. It occurred to me that it might be extremely informative to focus on viruses in general–what they are, how they work, how they spread, and how your immune system defends against them–and not get bogged down in technical details about the immune system while doing it. And that is so easy to do since the immune system is so intricate in construct and intelligent in design and execution. (For those of you looking for a more detailed examination of the immune system, check out my four part series: Anatomy and Physiology of the Immune System.)
With our objective in mind, let’s begin by looking at…
What Is a Virus and How Does It Infect?
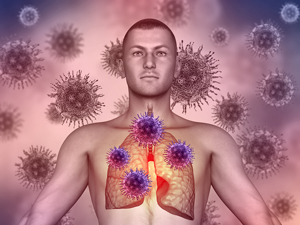 Viral infections can occur anywhere in your body, but since COVID-19 is essentially a respiratory infection, let’s focus our attention there.
Viral infections can occur anywhere in your body, but since COVID-19 is essentially a respiratory infection, let’s focus our attention there.
The respiratory tract is constantly exposed to the external environment and is therefore highly vulnerable to assault from pathogens. It, therefore, must be equipped to respond to and eliminate any invading viruses. Not an easy task. Clearing any viruses from the lungs and resolving all infections requires a complex, multi-faceted response initiated by:
- The cells that line your respiratory tract (epithelial cells).
- Your innate immune system. This includes the nonspecific defense mechanisms that come into play immediately or within hours of an antigen’s appearance in the body. These mechanisms include physical barriers such as skin, chemicals in the blood, and immune system cells that attack foreign cells in the body.
- And ultimately, by the cells of your adaptive immune system. Adaptive immunity refers to pathogen specific immune responses. The adaptive immune response is more complex than the innate. The antigen/pathogen first must be processed and recognized. Once an antigen has been recognized, the adaptive immune system creates an army of antibodies and immune cells specifically designed to attack that antigen. Adaptive immunity also includes a “memory” that makes future responses against a specific antigen more efficient.
It should be noted that although an effective immune response to eliminate viral pathogens is essential, a prolonged or exaggerated response can create prolonged inflammation and damage the respiratory tract. Damage to your pulmonary system caused by a prolonged immune response, which can be particularly problematic, is manifested clinically in a variety of ways depending on the location and extent of the injury. Thus, the antiviral immune response represents a balancing act between the elimination of any invading virus and any immune-mediated pulmonary injury.
So, what exactly is a virus?
A virus is an infectious agent comprised of RNA or DNA molecules that can only replicate inside a host organism (you, for example). They can infect a variety of living organisms, including bacteria, plants, and animals. When a virus particle is independent from its host, it consists of a viral genome comprised of a minimal number of RNA or DNA molecules surrounded by a protein shell called a capsid. In this form, it is known as a virion.
Viruses infect a human host by first gaining access to the body through the mouth, nose, or eyes; then using the bloodstream to travel around the body looking for ideal host cells. For COVID-19, and any other respiratory viruses, that usually means a cell inside the lungs. (Note: respiratory viruses can initially infect lung cells through direct contact when inhaled.) Once the virus finds what it’s looking for, it attaches to the chosen host cell using protein keys on its surface to open protein locks on the cell’s surface, allowing it to penetrate the cell wall and enter the cell. Once inside, it uncoats its genome from its protein shell and releases its genome into the host cell. Once freed inside the host cell, the viral genome hijacks the cell’s machinery, forcing it to replicate the viral genome and produce viral proteins to make new capsids. Next, the viral particles are assembled into new viruses. The new viruses/virions burst out of the host cell during a process called lysis, which kills the host cell.
- Note: COVID-19 appears to have a preference for two specific types of lung cells: goblet cells and ciliated cells. Goblet cells produce the mucus that both keeps your lungs moist and also captures particles, bacteria, and even viruses that you might inhale. Ciliated cells, on the other hand, have little hairs on them that move in a wavelike manner pushing the mucus (and anything it captured) up and out of the lungs into the back of the throat, where you can cough it out.
Following viral replication, the new virions can then either go on to exponentially infect and kill ever more cells in the host and/or escape the host and go on to infect new hosts. Note: although they act in every way like a thinking, purpose driven, parasitic lifeform, viruses are technically not alive as they lack essential systems necessary for metabolic functions that currently define life as we know it.
How a Virus Harms You
At this point, it’s probably worth explaining how COVID-19, or even the flu, makes you sick, sends you to the hospital, and may ultimately kill you. The first thing to understand is the virus itself is rarely responsible for directly killing you. A virus is not like cobra venom that is specifically designed to kill you–and does so. What harms you with a virus are the side effects as it simply goes about its business of replicating itself, coupled with your immune system’s response to that assault. In a sense, your health and life are simply collateral damage.
- When the virus is traveling through your bloodstream, it isn’t harming anything. It’s not until the virus takes over a cell in order to replicate itself and then bursts that cell to release its virion offspring that things start to happen.
- In the beginning, when there are just a few cells bursting and dying, the initial problem is inflammation. With COVID-19, since it’s primarily a respiratory disease, that means inflammation of your lung tissue. That can be felt as the “heaviness in the lungs” that people have described in the early stages of infection.
- In addition to lung tissue, there is strong evidence that COVID-19 is also comfortable invading both the liver and kidneys, where it can cause serious problems, including organ failure. Also, although the evidence is more preliminary, it looks like COVID-19 may also attack the heart muscle. One March 25 study from China published in JAMA Cardiology involving 416 patients sick enough to be hospitalized found that 20 percent had signs of heart damage.2 Guo T, Fan Y, Chen M, et al. “Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19).” [published online ahead of print, 2020 Mar 27]. JAMA Cardiol. 2020;e201017. https://jamanetwork.com/journals/jamacardiology/fullarticle/2763845 And of course, it can attack parts of the nervous system as evidenced by the loss of taste and smell in some patients.
- When the cells burst, and also as your immune system begins to respond by attacking viruses in the lungs, you end up with a lot of detritus from the exploded cells and destroyed immune cells, which your lungs try to wash away by creating more mucous and fluids. This leads to the shortness of breath people have described.
- As the virus continues to replicate exponentially, the number of dead cells, detritus, and bodily fluids created also increases exponentially making breathing much more difficult. This sends you to the hospital with the early stages of ARDS (Acute Respiratory Distress Syndrome).
- At this point, the stress on your immune system and the damage to your lungs makes you extremely vulnerable to secondary infections such as pneumonia, further exacerbating your situation. Pneumonia in a weakened body often leads to the pulmonary system damage we describe earlier or to ARDS.
- And finally, if your immune system can’t quickly shut down the virus it can get stuck in high assault mode, unable to turn itself off. This leads to the dreaded cytokine storm in which your own immune system inflicts huge damage on your lung tissue and sends you into critical ARDS and ultimately kills you.
- Note: For those who survive ARDS, a decreased quality of life is common.
And that, in very simplified terms, is how the virus impacts your body. By the way, it’s probably worth mentioning that if you have two viruses at the same time (COVID-19 and the Flu, for example) they can easily swap genetic material and create an entirely new virus, which potentially could be far worse than COVID-19, and for which, once again, no one has immunity.
How Your Immune System Defends Against Viruses
 From the description above, you should now understand that your immune system needs to attack and defend viruses in two separate locations.
From the description above, you should now understand that your immune system needs to attack and defend viruses in two separate locations.
- The first line of defense is the bloodstream before the virions have found a host cell. (Again: for many respiratory viruses, including COVID-19, the initial infection can bypass the bloodstream. Simply inhaling the virus from somebody else’s sneeze droplets, for example, can place a virus particle directly on a vulnerable lung cell–allowing it direct access into that cell. However, after the initial infection, as we will see, most virus particles have to travel through the bloodstream to reach the next round of lung cells for further infection–although some are released directly back into the lungs where they can escape the body in water droplets when sneezing or coughing and infect others. By the way, social distancing currently specifies six feet, but studies have shown that airborne particles from sneezes and coughs can travel upwards of 30 feet.3 Bourouiba L. “Turbulent Gas Clouds and Respiratory Pathogen Emissions: Potential Implications for Reducing Transmission of COVID-19.” [published online ahead of print, 2020 Mar 26]. JAMA. 2020;10.1001/jama.2020.4756. https://jamanetwork.com/journals/jama/fullarticle/2763852 Nevertheless, there have been a handful of studies that have shown that 6 feet of social distancing is enough to significantly slow the spread of a virus.4 Ahmed F, Zviedrite N, Uzicanin A. “Effectiveness of workplace social distancing measures in reducing influenza transmission: a systematic review.” BMC Public Health. 2018;18(1):518. Published 2018 Apr 18. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5907354/
- I use the term bloodstream metaphorically here. Macrophages can be found throughout the body especially in the lungs, liver, spleen, and lymph nodes, where their function is to free the airways, blood, and lymph of viruses, bacteria, and other particles. Macrophages also are found in all tissues as wandering amoeboid cells, The monocyte, a precursor of the macrophage, is the phagocyte that is literally found in the bloodstream.
- The second line of defense involves identifying any cells in your body that have been taken over by the virus and then eliminating them before they can spew their viral contents into the bloodstream. And for respiratory viruses, we’re obviously talking about lung cells here.
- If you don’t do both, the viral infection remains.
In your bloodstream, your immune system is capable of attacking the invading virus with both blind firepower (your innate immune system) and with targeted intelligent sharpshooters (your adaptive immune system).
The blind firepower consists primarily of the phagocytes (macrophages, monocytes, neutrophils, granulocytes, and dendritic cells) which attack and destroy or capture anything they sense as new or foreign. Although highly effective, they can be easily overwhelmed if the number of invaders is large, as happens once a virus begins exponentially replicating inside your body’s cells. One extremely powerful part of your adaptive defense that may be able to kick in simultaneously with your innate defense in the bloodstream can be found in the action of the antibodies–if the virus is one they are already programmed to attack. Antibodies are blood proteins (immunoglobulin) produced in response to a specific antigen such as COVID-19 and specifically designed to counteract that one particular antigen. So, where do antibodies come from and how do they work?
Antibodies
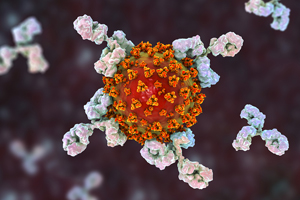 When your immune system encounters a foreign molecule (typically a protein) for the first time, the macrophages and dendritic cells that we’ve already talked about capture the molecule and begin breaking it down so that they can present these antigens (foreign substances) to B cell lymphocytes.
When your immune system encounters a foreign molecule (typically a protein) for the first time, the macrophages and dendritic cells that we’ve already talked about capture the molecule and begin breaking it down so that they can present these antigens (foreign substances) to B cell lymphocytes.
Once the B cell has locked onto the antigen, it begins coding for a new antibody that will contain a unique Antigen Binding Site capable of binding specifically to a vulnerable point (an epitope) on that particular antigen. Each B cell lymphocyte produces one unique antibody against one unique epitope on one specific antigen.
Once antibodies with sufficient specificity to the invader’s epitope can be encoded, the B cell begins to release antibodies into the bloodstream. These antibodies then bind with the specific foreign molecule found on the virus at its point of vulnerability (the epitope), marking the virus as an invader so that white blood cells canengulf and destroy it. After the foreign molecule has been eliminated, B cells remain in the bloodstream ready to quickly produce antibodies (bypassing the learning process) if the antigen is encountered again. But there is a catch. If you are encountering an antigen for the first time (can you say COVID-19), it can take your immune system anywhere from 9-14 days to analyze the invader and make an antibody blueprint and begin releasing those antibodies back into the bloodstream. In other words, it’s crucial that your innate immune system (your phagocytes) is strong enough to survive those first two weeks until your body can begin deploying the hordes of antibody sharpshooters that can ultimately clear the virus from your bloodstream. And it is here that natural immune boosters can come into play. If you are taking them regularly before a virus hits, your first line of defense will be at its maximum when needed and will likely carry you through those first 14 days. If you wait to take an immune booster until after you already have symptoms, it’s too late for immune booster to offer more than marginal help.
The Adaptive Immune System
Antibodies are an example of the adaptive immune system at work in the bloodstream. Your immune system has to study the invader and learn about its vulnerabilities before it can adapt your antibodies to defend against it. Once your system has identified an invader, it quickly develops a customized series of defensive weapons that specifically target the invader’s weak link. It then begins building cellular factories that produce these weapons en masse, in quantities sufficient to totally overwhelm and crush the invader. Then, once the invader has been defeated, the immune system has the awareness to “shut itself down” until needed at a later date. Also, your immune system has the ability to “remember” that invader and the defense that was used to defeat it. If that invader ever makes another appearance, even years later, your immune system can launch its defense much more quickly — and at a level 1,000 times stronger than when the invader first appeared.
Cytotoxic NK (natural killer) T-cells
As with the bloodstream, so with infected cells.
Now we’re going to look at how the adaptive immune system works to kill viruses that have set up camp inside your own cells–beyond the reach of phagocytes and antibodies. Simple logic says that only the adaptive immune system can do this since it requires that the immune system learn how to differentiate between a normal healthy cell and a cell that has been invaded by a particular virus so that it can adapt itself to target only the infected cells and not healthy cells.
As with antibodies, if your immune system has already been trained to recognize the virus that has invaded your cells, it kicks in with its strongest response, your T-cell defense, which is so strong that, if it has seen the virus before, it can often destroy the invader before you ever even know it’s there–or at worst, keeps the symptoms very mild and the sickness very short. It should be noted that we don’t store a lot of trained T-cells, just a few of each kind. Storage areas include the spleen, liver, and Peyer’s patches in the intestinal tract. The T-cells wait there, looking to see if they recognize the particular protein geometry of an invader they have been trained to identify (we’ll talk about how they do that in a moment) and then react to it. If so, they quickly set up factories in your body to produce replicas of themselves by the millions. Unfortunately, with COVID-19, no person on the planet has ever seen it before, so this line of defense is not available to most people. Instead, as with antibodies, your immune system needs to go through a learning, training, and adapting process.
The heart of this defense are the Cytotoxic NK (natural killer) T-cells, also known as Killer CD8+ T-cells. These are mainly T8 cells that have been activated by T4 cells and “transformed” into killer T-cells.
T4 cells have receptors on their surface that allow them to both identify the invading threat and then hunt down T8 cells to transform them into killers to crush the invader they’ve identified (in this case, the COVID-19 infected cells).
Once activated/transformed by a T4 cell, the T8 cell undergoes further growth and differentiation when stimulated by interleukin-2 released by the same T4 cell that locked onto it in the first place and activated it. This exponentially increases the number of NK cells programmed to identify a target antigen located on the surface of infected cells and then travel throughout the body in search of antigen-positive cells to destroy. This provides a failsafe two-step co-stimulation process for your immune system–that is stimulation by both direct contact with the T4 cell and stimulation by the interleukin-2 released by the T4 cell. This two-step process helps prevent the immune system from misfiring and attacking healthy cells in the body. Note: the exact same identify and destroy mechanism is used by NK T-cells to destroy both virus infected cells and cancer cells. I mention this because the following video shows a natural killer cell destroying a tumor cell. The way it does it is exactly the same as when identifying and destroying a COVID-19 infected lung cell.
How Your Body Knows to Respond
Pretty much every cell in the body can detect invading pathogens through what’s known as pattern recognition receptors (PRRs). These receptors can recognize the difference in molecular patterns found on the surface of invaders but are not found in the body’s own cells other than when cancer is present. This ability to recognize “non-self” and activate is, obviously, especially important in the epithelial cells that line the inside of the lungs when it comes to alerting the immune system to respond to the infection and limit the coronavirus from spreading.
The key here is that activation of PRRs triggers the production and release of interferons, cytokines, chemokines, and antimicrobial peptides which initiate your body’s innate and adaptive immune response–calling all of your defenses to rush to the site of infection. The overall response of your defenses against COVID-19, for example, as well as their ability to rush to your lungs, are determined by two things:
- The degree of PRR activation throughout the respiratory tract–in other words, how strong is the call to action for your immune system.
- The “readiness” of your immune system to respond, which ultimately determines the strength of its response. In other words, a strong call to a strong immune system elicits a strong response, whereas a weak call to a weak system or a strong call to a weak system sends you to the hospital.
If you’re interested, here’s a flow chart to help you visualize everything we’ve talked about so far.
Interferon
Before moving on, it’s worth spending a little time talking about interferon, which, as we mentioned above, is released by your cells at the site of infection. Interferons are categorized as cytokines, small proteins that are involved in intercellular signaling. Interferon is secreted by cells in response to stimulation by a virus or other foreign substance. It should be noted that interferon does not directly inhibit the ability of a virus to multiply but, rather, stimulates the infected cells and those nearby to produce proteins that prevent the virus from replicating within them. This inhibits any further production of the virus and, thus, stops the infection. Interferons also have immunoregulatory functions such as inhibiting B-cell activation, enhancing T-cell activity, and increasing the cell-destruction capability of natural killer cells. Typically, a virus-infected cell releases interferons–against the “wishes” of the virus–causing nearby cells to increase their anti-viral defenses.
When taken as a whole, what interferon does in the presence of viruses is pretty marvelous. The release of interferon actually has multiple impacts on your immune response.
- As already discussed, it draws your immune defenses to the site of infection.
- The release of interferon can cause hundreds of interferon stimulated genes, which primarily serve to limit further virus spread and infection, to activate.
- Interferon can also directly stimulate phagocytosis and dendritic cell maturation.
- It stimulates the production of chemokines and cytokines by respiratory cells. In other words, the release of interferon stimulates the production of more interferon, which further increases your immune system’s response, which releases more interferon…etc. And of course, if this process fails to trigger its own shut off–which it normally does–that’s what’s known as a cytokine storm, in which the immune system goes out of control and starts destroying lung tissue in a self-annihilating frenzy.
And that’s just the tip of the iceberg. There isn’t time to cover everything that interferon does such as inhibiting viruses from entering cells and replicating. It also directly inhibits the transcribing and translating of viral DNA inside your body’s cells.5 de Weerd NA, Samarajiwa SA, Hertzog PJ. “Type I interferon receptors: biochemistry and biological functions.” J Biol Chem. 2007;282(28):20053–20057. https://pubmed.ncbi.nlm.nih.gov/17502368/ And that should give you a hint as to how involved, intricate, and multifaceted interferon is.
Boosting your immune system
 For all the reasons we’ve mentioned above, having a strong immune system is one of your best defenses against viruses like COVID-19 and the flu. And scientists have known for years that it is possible to improve the functioning of both your innate and adaptive immune system. The conventional medical approach has been to use expensive, proprietary drugs, including concentrated cytokines such as interleukin and interferon. Unfortunately, that lacks the subtlety and second-by-second regulation of your body’s own interferon production, which can lead to serious side effects. Alternative healers, on the other hand, have adopted a more nuanced approach using natural substances to:
For all the reasons we’ve mentioned above, having a strong immune system is one of your best defenses against viruses like COVID-19 and the flu. And scientists have known for years that it is possible to improve the functioning of both your innate and adaptive immune system. The conventional medical approach has been to use expensive, proprietary drugs, including concentrated cytokines such as interleukin and interferon. Unfortunately, that lacks the subtlety and second-by-second regulation of your body’s own interferon production, which can lead to serious side effects. Alternative healers, on the other hand, have adopted a more nuanced approach using natural substances to:
- Stimulate and strengthen the immune system.
- Fight infection.
- Strengthen tissue against assault by invading microorganisms.
- Stimulate macrophage capability.
- Increase T-cell production and protect helper T-cells.
- Complement the action of your body’s own interferon and interleukin-1.
- Promote increased production of cytokines as called for by your body.
- Assist the cell-mediated immune response.
Note that what we’re talking about here goes beyond eating healthy and taking extra vitamin A, D, and C. Doing those things will optimize the “normal” state of your immune system. But “boosting your immune system” is something more than that. We’re talking about pushing your immune system into a heightened state of readiness, a state beyond normal. Think of it like running shoes. You can train for months and push your body to a maximum state of fitness, but if all you wear when you run, no matter how fit you are, is everyday sneakers, you’re only going to be able to run so fast. But wear some of the new, hi-tech running shoes, and you can push beyond the limits of what we think is humanly possible.6 Delia Paunescu. “Nike’s high-tech Vaporfly sneakers help athletes run 4 percent faster. Should they be banned for providing an unfair advantage?” Vox. Nov 3, 2019. (Accessed 13 Apr 2020.) https://www.vox.com/recode/2019/11/3/20944257 That’s what immune boosters can do for your immune system.
Ingredients to look for in an immune boosting formula include Echinacea, Pau d’arco, astragalus root, Suma root, and various mushrooms such as cordyceps. A bottle a month per person is all you need for this formula to provide optimum support for your immune system. There are three keys to using it.
- You need to use it before you are infected. Immune boosters don’t kill a virus once you have it. Instead, they help prepare your body in advance to better fight an invading virus if and when you are infected by one. Ideally, you want to be using an immune booster for at least a week before confronting an infection.
- Three 1 mL droppers per day is all you need. That means a 60 mL bottle will last 20 days, which provides a full month of immune system support as you will see in a moment..
- Since one of the primary modes of action of immune boosters is to trick your immune system into thinking it’s under attack so it heightens its defenses, you need to give your body a break from immune boosters every month. The problem is that after about 20-25 days your immune system begins to figure out that there really is no invader and begins to lessen its response to the immune booster. In other words, it begins to lose effect. But if you take five-10 days off every month, your immune system can be tricked into starting the cycle all over again. And don’t worry about taking the five-10 days off. It’s not like your immune system suddenly drops off a cliff when you stop taking the booster. The tail off is gradual–in fact, almost non-existent during the days you’re not using the booster.
Using an Antipathogen Formula
 One day in early March, Kristen and I both noticed the same symptoms. They were not severe, but they were enough so that we both commented on them.
One day in early March, Kristen and I both noticed the same symptoms. They were not severe, but they were enough so that we both commented on them.
- In the mid-afternoon, we were suddenly unusually tired.
- We both had low level muscle aches.
- And we both felt something “off” in the lungs and sinus cavities.
As I said, the symptoms were not severe. And if it weren’t for the virus being on our minds, we probably would have shrugged it off as the result of working too many hours several days in a row. In any case, we decided not to ignore it and each down a bottle of my antipathogen formula, as follows:
- We had approximately a third of a bottle (20mL) at a time–just eyeballing it as we poured it into a glass. We then added a couple of ounces of low-salt tomato juice, and a couple of ounces of water.
- Mixed it up and sipped it down over about five minutes.
- Repeated that two more times spaced throughout the rest of the day so that we ended up consuming the entire 2 oz bottle that day.
What we noticed was that within about 20 minutes of sipping down each glass, all symptoms disappeared, only to return in milder form before the next glass. After the third glass, we went to bed and woke up the next morning feeling fine. No symptoms of any kind. At that point, we passed off the previous day’s symptoms as just being tired and that we hadn’t had the virus. By the way, one of the advantages of having formulated the product is that I know why it makes sense to always have a good supply on hand for whenever we need it.
About three days later, the symptoms came back, but noticeably stronger than before, including a strong feverish feeling (although when we checked our temperatures, we both were 1 degree below normal). In any case, there was no question, whatever this was, it was very different than any cold or flu we had ever experienced (keeping in mind I’ve only had the flu once in the last seven years). At this point, we were pretty sure it was COVID-19. If I were to guess what had happened, we had destroyed most of the virus in our bloodstream but hadn’t touched the viral factories in our cells. When the infected cells burst open over the next several days and the virions poured out in greater numbers than before, the symptoms returned stronger than ever. We weren’t worried at all since we knew that the formula had worked the first time we took it; we just hadn’t taken it long enough. In any case, we knew it was now time to take whatever we had seriously.
- We then repeated the bottle a day routine for the next four days (three days probably would have been enough, but what the heck, better safe than sorry). Oh, and since we were out of tomato juice, we used diluted orange juice, which also tastes just fine with all the garlic in the formula. (And from past experience, we know that apricot juice and peach juice are also winners.)
- All symptoms were gone by the third day. Again, the fourth bottle was just to let the virus know who was boss.
- Then for the next six days (days 5-10), we finished off a fifth bottle doing 10 droppers a day in diluted juice just to make sure we covered the virions released by any surviving cell factories before they could infect any new cells. By itself, this may have eliminated the virus. And if not, it bought us the time for our adaptive immune system to learn all about the virus and take over with both antibodies in the bloodstream and NK cells to find and destroy any remaining infected cells as needed.
- Based on this description, it should be obvious that trying to save money or stretch the formula or share the same bottles among several people is counterproductive. Using just one or two bottles and stopping may make the symptoms go away briefly, but it allows the virus to come back as soon as any infected cells burst. In that sense, it’s like using antibiotics. Your symptoms may go away after a couple of days, but if you don’t complete the full program as prescribed by your doctor, the infection will simply return in a few days–more aggressive than ever.
- Anyway, since completing our five bottle, 10-day program, the symptoms have not returned.
Now Please Keep the Following Caveats in Mind
 This is our personal, real-life experience with the formula and may not reflect the experiences of anyone else who uses it. And yes, I realize that personal anecdotal experience is not the best way to evaluate efficacy–without substantial corroboration.
This is our personal, real-life experience with the formula and may not reflect the experiences of anyone else who uses it. And yes, I realize that personal anecdotal experience is not the best way to evaluate efficacy–without substantial corroboration.- Let me be clear that I believe both Kristen and I had the COVID-19 virus. But thanks to the dearth of available testing, we couldn’t verify infection at the time. So, it’s possible we may never have had COVID-19 in the first place. But again, the symptoms, although relatively minor, were unlike anything we’d ever experienced before. And we both had the same symptoms. Bottom line: we’re pretty sure we had the virus. Nevertheless, we won’t know for sure until the long-promised antibody tests arrive. They will tell us if we have antibodies to COVID-19 in our bloodstream, which we could only have if we’ve had the virus.
- Also, let me be clear. We’re not saying that the formula cured anything. It didn’t have to. All we’re saying is that the all-natural ingredients in the formula supported our innate immune system’s efforts in holding down the viral load until the stronger and more targeted adaptive immune system could take over and eliminate the virus.
- And finally, we cannot be sure the formula actually did anything at all? Many people who have the virus have either no symptoms or very mild symptoms. Perhaps my formula had no effect, and the virus simply followed its normal course in our bodies. Who is to say? My answer to that would be:
- There are eight ingredients in the formula that have each independently demonstrated strong antiviral activity in studies.
- It would be a remarkable coincidence if the course of the virus “naturally” followed the absolutely identical timeline in disappearing from both our bodies without some outside influence affecting the outcome.
- It also should be noted that Kristen and I both have over two decades of experience with this formula when it comes to dealing with colds and flu–both preventing them from going beyond the incubation phase and cutting their normal cycle in half on those rare occasions when we’ve actually come down with anything.
- Over the years, we’ve received hundreds of testimonials from people who have used the formula to similar effect. And yes, they too could have been mistaken, but as the numbers add up, that looks less and less likely.
- And finally, if the CDC would like to test the formula, we’d be happy to send them samples. They could start with in vitro testing to see if the formula can kill the COVID-19 virus in a lab. There are any number of assay tests that could verify efficacy inexpensively in a matter of hours.7 “In Vitro Antiviral Testing.” IBT BioServices. (Accessed 10 April 2020.) https://www.ibtbioservices.com/bioservices/antiviral-testing/ If it passed muster in the lab, considering the current pandemic environment, in vivo testing could then be quickly instituted and results verified.
By the way, this brings up a festering problem. Once you’ve had the virus and are no longer in danger of catching it or communicating it to others, how do you once again emerge in public without having to wear a mask or terrify any who accidentally enters your six-foot safety zone.
- The Federal Government is considering issuing Americans certificates of immunity from the coronavirus that they can carry in their wallets to show to anyone who needs to see it. That presents several problems. First, think how many times a day you’d have to show it if you were back to work and out and about. But more importantly, if you now went maskless when shopping in a story because you legally could, how would anyone else in the store know that you were legal and safe and not just thoughtless and putting everyone else at risk. It could lead to many unpleasant confrontations, with some being violent.
- Of course, in China they’re beginning to require citizens to use software on their smartphones that dictates whether they should be quarantined or allowed into subways, malls, and other public spaces. More disturbingly, it also uses geo-tracking to monitor every move you make and every single person you interface with (through their phones) as you go about your day. And then all the people they interface with, etc.–ultimately tracking the lives of every single person in the country who owns a cell phone.Again, the software still requires you to pull out your phone countless times a day to identify yourself to others. And you still could be subject to confrontations from people who didn’t know your status. But the software would always be tracking your movements whether you pulled the phone out or not. Look, I know many of you out there are concerned about the idea of forced vaccination for COVID-19 when a vaccine is finally approved–and you should be since I consider that to be a likely eventuality down the road–much like smallpox and polio vaccinations. But, and let me be perfectly clear about this, I consider the danger from forced vaccination to be far less than the potential danger from tracking software installed on everyone’s phones. Look, if used as promised, there should be no problem, and it will undoubtedly save lives. But that said, when have governments ever limited their “oversight” of their citizenry to the “promised” boundaries? Just sayin.
So, with that in mind, Kristen and I had the following T-shirt made for ourselves. We’re just waiting for the antibody test to confirm our status as COVID-19 survivors so we can wear them. Feel free to make up your own. Or for that matter, any T-shirt company should feel free to run them off by the thousands and sell them to as many people as possible. We put the TM on the shirt merely to prevent anyone else from trying to claim a trademark and preventing anyone else from making the shirts. Anyway, if you see any of the shirts appearing in the months ahead, you’ll know where it all started.

References
| ↑1 | Jana Winter and Sharon Weinberger. “Sunlight destroys virus quickly, new govt. tests find, but experts say pandemic could last through summer.” Yahoo News April 17, 2020. (Accessed 17 April 2020.) https://www.yahoo.com/news/sunlight-destroys-coronavirus-very-quickly-new-government-tests-find-but-experts-say-pandemic-could-still-last-through-summer-200745675.html |
|---|---|
| ↑2 | Guo T, Fan Y, Chen M, et al. “Cardiovascular Implications of Fatal Outcomes of Patients With Coronavirus Disease 2019 (COVID-19).” [published online ahead of print, 2020 Mar 27]. JAMA Cardiol. 2020;e201017. https://jamanetwork.com/journals/jamacardiology/fullarticle/2763845 |
| ↑3 | Bourouiba L. “Turbulent Gas Clouds and Respiratory Pathogen Emissions: Potential Implications for Reducing Transmission of COVID-19.” [published online ahead of print, 2020 Mar 26]. JAMA. 2020;10.1001/jama.2020.4756. https://jamanetwork.com/journals/jama/fullarticle/2763852 |
| ↑4 | Ahmed F, Zviedrite N, Uzicanin A. “Effectiveness of workplace social distancing measures in reducing influenza transmission: a systematic review.” BMC Public Health. 2018;18(1):518. Published 2018 Apr 18. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5907354/ |
| ↑5 | de Weerd NA, Samarajiwa SA, Hertzog PJ. “Type I interferon receptors: biochemistry and biological functions.” J Biol Chem. 2007;282(28):20053–20057. https://pubmed.ncbi.nlm.nih.gov/17502368/ |
| ↑6 | Delia Paunescu. “Nike’s high-tech Vaporfly sneakers help athletes run 4 percent faster. Should they be banned for providing an unfair advantage?” Vox. Nov 3, 2019. (Accessed 13 Apr 2020.) https://www.vox.com/recode/2019/11/3/20944257 |
| ↑7 | “In Vitro Antiviral Testing.” IBT BioServices. (Accessed 10 April 2020.) https://www.ibtbioservices.com/bioservices/antiviral-testing/ |











You stated “You need to use it before you are infected. Immune boosters don’t kill a virus once you have it. Instead, they help prepare your body in advance to better fight an invading virus if and when you are infected by one. Ideally, you want to be using an immune booster for at least a week before confronting an infection.” Yet you guys used it after you were infected and it still helped!
Two different formulas. What Jon and Kristen took once they thought they were infected was his antipathogen formula, not his immune boosting formula.
Please consider the following: (research article 1) “most common cold viruses, attach to receptors in cells of the mucus membranes of the upper respiratory tract and then replicate out of control.9,10 When taken as a slow-release lozenge, zinc binds to those same cell receptors, preventing the rhinovirus from entering cells and establishing a common cold infection. This makes it uniquely effective in warding off colds.11
Zinc is a mineral that has functions throughout the body, including support for the immune system. But its unique effect in the throat (blocking viruses from entering cells) is what makes the occasional use of zinc lozenges so beneficial. … a team of researchers led by pioneering scientist George Eby published the results of the first double-blind, human study on zinc lozenges for common colds. They discovered that after seven days, cold symptoms vanished in 86% of people taking zinc, compared to 46% taking placebo lozenges.2
The form of zinc that most effectively binds to cell receptors, blocking the cold virus, is ionic zinc.3
This type of zinc has acquired a positive charge by losing electrons.
There are significant differences in the amounts of ionic zinc released from the different zinc forms. Scientists have now calculated these amounts, and they found that:3
Zinc acetate releases 100% of its zinc as ionic zinc,
Zinc gluconate releases 72% of its zinc as ionic zinc,
Zinc gluconate-glycine releases 57% or less of its zinc as ionic zinc, and
Zinc gluconate-citrate releases no ionic zinc.”
(me) The above information shows that ionic zinc can block the rhinovirus from entering mucus membranes. Could it also help to block coronaviruses from entering mucosal cells? I think it most likely does.
I have been using one zinc lozenge per day after breakfast . The zinc lozenge distorts my sense of taste for a few hours (just like the COVID19 symptom).
We know that viral infections usually begin in the upper respiratory systems, hence the advice to NOT touch your face. I have come to find out that COVID19 infection does it’s most significant damage by entering Type 2 Pneumocytes in the lungs via a receptor. Type 2 Pneumocytes are a type of mucosal cell. Once inside, the virus multiplies rapidly and destroys the cell causing many more viruses to be realeased and an immune response that then causes more damage to the lungs and damage to Type 1 Pneumocytes. These cells are the ones that exchange gases (oxygen into the blood and CO2 out of the blood).
If you could block coronavirus from entering some or even most of the type 2 Pneumocytes then the immune system would have the time needed to produce the antibodies that actually kill the virus before it kills you, or causes significant lung damage.
Now consider this: (research article 2) “A South Korean research paper has demonstrated in Vitro that by increasing the Zinc concentration in cellular cytoplasm, that viral replication is inhibited. As intracellular levels of Zinc are increased the inhibition of viral replication can reach 100% according to charts within the paper. The researchers used two antimalarial drugs which are Ionophores. Ionophores are molecules that can carry a charged ion like Zinc across a cellular membrane. South Korea has been treating high risk, Critically I’ll COVID-19 patients with the drug Hydroxychloroquine. It is likely the single clinical reason that South Korea has the lowest death rate in the world for COVID-19 victims of 0.6% Hydroxychloroquine is a pharmaceutical drug that requires a prescription. However there is a nutritional supplement called Quercetin that is a Zinc Chelator and Ionophore and requires no prescription.”
(me): It’s seems that ionic zinc would likely be more useful if it were already in your system than waiting for a critical infection to use it. The previous information (research article 1) shows that certain forms of zinc already release zinc as ionic zinc. I am using zinc lozenges on a hunch. One per day isn’t going to put me over the RDA of 15mg per day of Zinc. I won’t go above the recommended dosage if I begin to use them more frequently. I also take quercetin in a “resveratrol/quercetin” supplement every day and have been for a long time. I also have two bottles or Super Viragon saved, that I am prepared to use for myself or a family member should I suspect an infection. I’m also thinking that if I had an infection and then recovered that I would want to use your Blood Support, KGP Flush, Liver Flush and Colon Detox to help remove the leftover junk.
Great article that informs individuals how important it is to have your immune system in a healthy and ready mode.
I also felt similar symptoms a few weeks ago which I didn’t have your Immune Formula to use. But what I did use was Silver and Zinc. I took one teaspoon each, three times each day. The symptoms went away within one to two days so I discontinued use. About one week later the symptoms returned so I restarted the Silver and Zinc as before, but stayed with it for a week even though my symptoms disappeared after about a day. So far I have felt normal.
I also do this routine if I feel a cold coming on with that fatigue and scratchy throat feeling, which with me doesn’t happen often. All I can say is I haven’t had the flu in many years even though people within my household have gotten real sick. So I do believe in the Silver and Zinc mineral as a viral killer, but I will order your Immune Formula to cover all aspects of my immune system.
Please continue your very informative Health Articles, they help me learn how my body functions which is a miracle in itself.
always enjoy your articles,what do you think of the rumors that people who had the virus,overcame it and have it again is this a real possibility or a testing snafu.thanks
In New Zealand the government teaches pigs to cough into their elbow. So what do they do? They cough over the police & checkout operators.! unbelievable training pigs to be pigs. If women used man sized handkerchief they would not have a attitude to using handkerchiefs, I use a handkerchief so you do not get my gems when I cough or sneeze, I have never been hospitalized for using a handkerchief.
But there is some evidence that coronavirus may spread from aerosols produced from simply talking and breathing. If so, it doesn’t matter how big your handkerchief is if only used when you cough or sneeze; you might still be a super spreader. https://www.youtube.com/watch?v=aT50eE5jxvg
So fat chance coughing into your elbow is going to any good then. It is worse than using a handkerchief
well what is the point in coughing into your elbow like a pig that would seem worse than using a handkerchief
Oh my! We are feeling feisty today, aren’t we? Unfortunately, your understanding of how viruses transmit from person to person is slightly flawed. As it turns out, there is one huge difference between coughing into your elbow and coughing into a handkerchief. And it’s the hand part. When you cough or sneeze into a handkerchief that you are holding, inevitably, some of that spray is making its way onto your hand. From there, you transfer the germs to the cash with which you pay the checkout clerk, thus infecting them; or you transfer the germs to the electronic pen you use to sign the credit card machine if you pay that way, which, of course, infects the next person who uses the machine. And then, of course, there’s all the packaging you touch while shopping , which then infects the healthcare worker who follows you down the aisle two minutes later and touches the same packaging. Unfortunately, she then brings the infection, while displaying no symptoms, to her job at the nursing home, where she infects the entire population, eventually killing 36 residents. So, there is that—which doesn’t happen when you cough into your elbow.
I just read that with covid-19 (ARDS) the lungs create a detritus of protein based edema fluid and extra fibrin in the lungs. Why could we not then take your proteolytic enzymes which love to digest both proteins and fibrin in the body? I initially ordered an extra bottle of those enzymes to try and get a head of the Corona virus and kill it by digesting the protein shell around the virus.
Then it was said that the virus has a fatty shell around it rather than a protein one so I thought it likely that the Proteolytics wouldn’t work to deactivate and kill the virus. It’s hard as a lay person to take all the information given and absorb it and see all the patterns in a given disease and it’s mitigation and cure. Would love to know how proteolytics can help with covid-19 or if they do not.
Yes, any proteolytic enzymes formula that contains Seaprose-S is likely to help assist your body in clearing excess mucus, fluids, and protein detritus from the lungs. It can’t hurt.
Excellent information beyond the washing your hands mantra. I appreciate everything you have put into this piece of work, but I am so sad that even information such as your is causing people to politicize the virus. I have deep appreciation for all your work and integrity. Please keep educating us as only you can.
As always Jon, excellent and articulate educational commentary on why’s and what’s to help us lead safe, healthy and active lives. I am always impressed with the fact that you make all your health articles and reports available to all without a subscription, unlike many of my other mentors. Your selfless sharing is not only commendable, but a real altruistic benifit to all who read your reports. Thanks so much for the wonderful work you do.
TY Jon and Baseline staff for your reliable info. I have posted a url of your jonbarron web-page as well as Mike Adams pandemic.news on my Facebook page.
From the news today: “coronavirus symptoms thus far have presented chiefly within the respiratory system, the infection is swiftly showing to be an all-out, system-wide assault that reaches far past the lungs. … (including) an unexpected prevalence of blood clot(s).”
I’m thinking use of your pHI-Zymes would help to minimize this danger. As well as your Blood cleanser, Kidney flush, Liver flush, Colon Detox and just for good measure some extra Psyllium fiber until the Coronavirus junk yard is cleaned out.
What would you recommend doing to clean up the mess the Coronavirus is leaving behind?
This is a copy of the letter addressed to the WHO on COVID-19 by me recently
The Director General
World Health Organisation
Sir,
There are lots of misconceptions hovering around novel corona virus infection. I think, media has given exaggerated hype, though it is true it is more infectious than any other viral infections. Just go by its fatality rate, which speaks volumes about its nature and character, because it shuttles between two and four percent and not more in the world, because not all are likely to be infected. Here lies the clue in terms of arresting this infection. With good immunity in body, it fails to last long. So taking this aspect into view we can develop such supplements, which could restore our sagging immunity. In fact, the WHO talks a lot about developing immunity, but I don’t think it has any clear cut theory about immunity, say what is bad or good immunity? What is the yardstick of measuring one’s immunity? I think, it is still not clear to many why some individuals infected with the disease remain asymptomatic, there are others who develop mild or moderate symptoms and some get critically ill and succumb to disease. If I am correct, the WHO has also no satisfactory answer against this phenomenon. But it’s answer is very simple, that is the immunity itself. An individual with good immunity will remain asymptomatic, provided he is not suffering any other acute symptoms. Second, even with good immunity one may develop mild symptoms if he is suffering from any other acute symptoms such as diarrhea, upset digestion or has recuperated recently from any acute infection etc. Third, some get critically ill, because either he has comorbidities or has very low immunity level for some failed diagnosed reason. This subject has been elaborately explained below.
Now I shall discuss here on the bad effects of oxyhydrochloroquine, though it has many, yet it triggers some other fatal effects in the system, which I have found in course of my studying the ill effects of quinine in the body of some patients, who were on quinine therapy for some time for malaria, and since oxyhydrocholoroquine has also the same effects, though it is a synthetic drug, yet crude quinine (cinchona bark) is far superior in its effectiveness than a synthetic one. Administration of quinine for a long time as preventive medicine against malaria slowly diminishes the platelets count, which means it abnormally thins out the blood that may trigger internal bleeding also. Next, it also plummets down the WBC count, which makes the body prone to every kind of opportunistic infection for example UTI etc. Quinine also triggers splenomegaly, this I had detected not in one but in several patients, who had been ultimately cured by me. These patients were taking choloroquine for a pretty long time as a preventive medicine against malaria on their doctors’ advice. So, we can rule out its use in corona virus infection, but it is still being used by some countries, because there is no other alternative.
Next, some researchers are contemplating to try out BCG vaccine, unfortunately it seems these people have not monitored the candidate, who has been inoculated once with the BCG vaccine for a long time, for a BCG vaccinated person in the long run becomes prone to tuberculosis, particularly pulmonary. Once inoculated with BCG, the person always displays positive result against Mantoux test, which means he becomes a carrier of latent tuberculosis in his system. In the event of creation of right environment, he is most likely to be quickly infected with tuberculosis. Moreover, his WBC count also always remains on the lower side, for which frequent bouts of colds and cough become a part of his life. All these conclusions I have drawn monitoring hundreds of patients for years. My findings can be searched out on internet. This is only one or two findings of mine. There are many more findings, which have been ignored by researchers, or any medical journal. Similarly any fistula, if operated upon, then in the patient there is every possibility in future he may develop cancer of any internal organ. I think, this has also not been researched so far. But this situation will not arise, if in fistula treatment is given by administering anti-tubercular drugs, which means there is definitely some link between TB and any fistula. Even there is a latent relation between incorrigible ear infection and tuberculosis; in such a case howsoever medicines are administered the ear continues to ooze out pus, and even if cured the infection recurs again and again. In such a case administration of anti-TB remedies gives good result. I don’t think anybody is aware of all these facts. Similarly, multi-drug-resistant TB of late has become incurable, even simple MDR case, keep aside XDR or TDR tuberculosis, the fatality is more than 50% in the world, yet the WHO or any other researcher has failed to find out a safe remedy that can assure cent percent guarantee of recovery. Similarly trying out Remdesivir or any anti-AIDS remedies or ezithromycin is like throwing an arrow in the dark or turning a suffering human being into a guinea pig. All these meaningless trials should not be acceptable to a sane doctor, unless there is one hundred percent guarantee, otherwise such trials are crime against humanity, I feel. A poor infected soul will reluctantly always give his tacit consent with a hope that the medicine may click, unfortunately it is never, and his death is hastened. In some cases, they may display some result, but I think it is not due to medicine, but by due to good immunity of the patient. After all these all are unproven remedies. Under present situation vaccine is a far cry, unfortunately the world will never have any reliable vaccine against corona infection, because it’s virus also mutates like AIDS virus. Billions of dollars unnecessarily have been wasted so far in finding out a vaccine against AIDS without success, likewise the world will never have any vaccine against SARS-CoV-2, it is my conclusion, because more than ten strains of corona virus have already been identified. Therefore, there are plenty of cases, when in a cured patient of COVID-19 the infection has once again recurred. Then what does this indicate? It is a clear case that the patient has been infected second time by the different strain of virus.
Then what? If we do not contain the disease, then in coming years death toll will go on burgeoning into millions, may be into a billion or two in future, this is just the beginning. I was studying the case of USA, why there is so much of fatalities, neither the CDC or the FDA has any answer, nor the WHO has. What more could we tell, in so many years the modern researchers have even failed to find out a cure against simple Asthma, then just think, what more could be disgraceful than this for the humanity. On the whole modern science has failed on many counts to provide relief to ailing humanity, but it does not admit its discomfiture.
One more finding of mine I want to discuss here for the benefit of humanity, for example any thing bitter in taste, no matter whether it is a beverage or some food, causes an adverse reaction in the production of leukocytes, WBC count start falling, though its pace of fall is very slow. Now, I am coming to my finding, say beer, which is bitter in taste, has a similar effect in the leukocytes triggering leukocytopenia in blood, though nobody has conducted any research into this phenomenon so far. Margosa leaves have similar reaction in the body, if consumed for a long time, though it is also a good remedy to cure malaria. As we know, beer acquires its bitter taste due to hops. In view of this, more number of deaths will take place in the USA in coming years due to SARS-CoV-2 infection, and also in other European countries, where people are in the habit of consuming beer more than water. I am pretty sure, if WBC count of most of the healthy Americans is taken at present, it will display less than 6700 per micro litre, of course if they are in the habit of consuming at least a bottle of beer (650 ml) every day. But the result may be different also if the candidate takes plenty of citrus fruits daily simultaneously, but it is yet to be researched by me. Plus most of the Americans develop comorbidities with age, therefore, for blood pressure over the counter sale of aspirin is more than all countries of the world taken together. Cancer is also common in American society due to over dependence on non-veg items.
So in order to strike the adverse impact of novel corona infection from the reverse or to reduce the number of mortality rate, then we have to increase the WBC count in the patient, in a healthy person it should not be below 6700 and not above 9000 per m-litre. In my opinion, according to my studies for years between 6700 and 9000 per micro litre should be the standard WBC count in the body, not as projected say between 4000 and 10000 in the medical text book, because above 9000 the candidate begins to feel feverish sometime or other, though at early morning he may feel better, and below 6700 per micro litre, the person becomes prone to cough and colds, and other opportunistic infections. If the WBC reading in a person is above 6700 then even if infected with any viral infection, including corona, the duration of infection will be extremely short, it will simply touch and cause some uneasiness and vanish without causing much damage to the system provided he is not suffering or has suffered recently from any acute infection, which has lowered his WBC count. Below 4000 the patient is not likely to overcome the disease easily even if he has no earlier chronic symptoms, such as renal disease, or severe liver dysfunction like Hepatitis B or C or jaundice, or has recently recuperated from any chronic disease or for some reason he is under steroids or he has some serious blood disorder etc. With WBC count above 6700 per micro litre, but below 9000 has a chance of complete recovery of any COVID-19 patient, provided he has no other acute symptoms, even the patient may remain asymptomatic in many cases and within a few days he will be free from COVID-19 virus, there is not an iota of doubt. Second, having same WBC count in the blood, even if rendered physically weak by some acute infection, then he would develop mild symptoms. but his chances of prognosis remains very good. Third, the patient having comorbidities and other debilitating disease or all along his WBC count is below 6700 per micro litre, then his chances of recovery is very slim, he may develop serious symptoms.
For the benefit of all, once again I am disclosing here the name of a remedy, which triggers quick leukocytosis in the system, this remedy was used by me in almost all cancer patients who were undergoing chemotherapy to raise their WBC count, because in chemotherapy WBC count quickly falls, and this remedy was also used by me in AIDS patients to restore to normal their falling T cell counts , in both the cases the results were excellent. The name of the remedy is: Baryta Iodata, general name. We have to have at least 2X potency of Barayta Iodata, its formula is: it is mixed up with milk sugar in 1:10 proportion at first, which means one part crude remedy and ten parts of milk sugar, and then take one part of this mixture (1X) and again dilute it with ten parts of sugar of milk. Simple one gram of this remedy dry tongue once a day quickly restores the falling WBC count to the normal level. This dose can be increased to one gram dose thrice a day also when the WBC count is abnormally low to obtain quick result as in a cancer patient who is undergoing chemotherapy.
Now a few lines on Cytokinesis Storm Syndrome (CSS), and how to tackle this situation. The high response of one’s own immunity in the body is also a disease. because there is abnormal flare-up of WBC in the system. This will occur in a patient, who is for some reason under immune suppressive drugs or under steroids therapy, immediate withdrawal of such drugs may trigger high immune response. But there may be some idiopathic cause also, though I do not believe in using such term, because behind such blood abnormality some cause always remains hidden, though that might not have been diagnosed yet. This is just like using the term allergy randomly to dispose of a case, when a doctor fails to pin point a cause.
I do not know, how a doctor will try to tackle this situation, but I used a single remedy in such cases with very good response. The name of this remedy is Echinacea Q. Simple administration of this remedy taking ten-drop as a dose in little water two hourly will quickly arrest this symptom within a few days.
Covid-19 is a complicated disease, therefore it is to be tackled carefully. What other remedies we could use, and how to take care of a patient, I have discussed at length in the attached paper.
The researchers at least till now have no antidote in their kitty worthy its name against COVID-19 (SARs-CoV-2). At random, physicians are using different remedies and on recovery of a patient or two (unfortunately they do not elaborate in detail the condition of the patient or his immunity level when admitted) place a claim before the medical world that they have found an authentic remedy. In this trial and error game many patients may die also, whether the cause of such death has ever been clearly stated any time in detail by any doctor in a death certificate, I doubt. The attachment will clearly elaborate all these facts. As I have explained above, most of the patients with good immunity level will recover on their own whether or not any medicine is administered, like any viral infection.
For the sake of saving innocent lives, please do not ignore this letter like my previous mails, because if read thoroughly you will discover many facts, which have hitherto remained unexplored in the world of diagnosis.
May God bless mankind!
Yours faithfully
Dr.P.K.Chhetri