In a new report aimed to once again scare all users of herbal supplements, the medical community has issued a warning indicating that taking certain herbs when on heart medication poses big-time risks. The report, published in the Journal of the American College of Cardiology, cautions that herbs like Echinacea, Gingko biloba and St. John’s wort can enhance the power of prescription drugs making them too strong; or alternatively, they can block their effects, or can exacerbate side effects, causing heart arrythmias, bleeding, and other dangerous conditions.
“We can see the effect of some of these herb-drug interactions — some of which can be life-threatening — on tests for blood clotting, liver enzymes and, with some medications, on electrocardiogram,” said Dr. Arshad Jahangir of the Mayo Clinic in Arizona. Dr. Jahangir does admit that it’s the interaction, not the herb, that’s the problem. “These products are not by themselves dangerous,” he says. “But when taken with medications for cardiovascular diseases, a relatively safe compound can become dangerous.” He tops off his position with the refrain so often heard emanating from mainstream medical quarters: “Natural does not always mean safe.” (Ah shucks, he was almost able to maintain an unbiased perspective — until his final statement.)
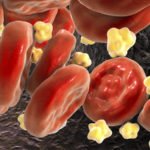
A total of 30 herbal remedies made it to the list of no-no’s for heart patients. Among the verboten are garlic, ginseng, ginkgo, grapefruit, black cohosh, St. John’s wort, hawthorn, saw palmetto, green tea, alfalfa, ginger, and Echinacea. Certainly, there’s plenty of evidence that herbs can make dangerous pharmaceuticals even more dangerous. Echinacea, for instance, can increase the risk of liver damage from statins. Garlic, ginger, gingko, and saw palmetto all increase the risk of bleeding when taking warfarin, an anticoagulant used to prevent heart attacks, strokes, and blood clots. The bottom line is that you can’t do herbs and meds at the same time without checking into the interactions first. But again, that doesn’t mean that the herbs involved are inherently unsafe — only that they may complicate the lack of safety inherent in the pharmaceutical drugs.
Unfortunately, this is not a trivial word game. In this case, perspective matters. From the medical perspective, the herbs are the problem and should be dropped to allow the pharmaceuticals to work — but in some cases, perhaps it’s the pharmaceuticals that need to go away to allow the natural remedies to do their job.
For instance, the big complaint against grapefruit juice and St. John’s wort is that they interfere with the effectiveness of certain medications, including statins, often prescribed for high cholesterol. Considering, as I’ve written before, that study after study shows that statins may do more harm than good, preserving their effect may not be the ideal point. A 2008 study found that patients taking statins reaped no benefit whatsoever from the drug unless they already had heart disease. Among the side effects associated with statins are severe muscle pain, severe memory loss, nerve damage, trouble talking, nausea, vertigo, and a fifty percent increased risk of cancer. Grapefruits have none of those side effects, plus they cost a whole lot less than statins do. In fact, a 2006 study published in The Journal of Agriculture and Food Chemistry found that red grapefruit can lower cholesterol in patients who had no success using statins. Plus, grapefruit offers a multitude of health benefits, from helping with weight loss to offering anti-carcinogenic effects.
But alas, the researchers see things very differently. For instance, Dr. Wallace Sampson, clinical professor emeritus of medicine at Stanford University, points to the periodic reports about the potential dangers of herbal remedies. “There are quite a number of them in the medical literature, targeted to different specialties…. Most controlled studies of alternative medications have not shown benefit [really?], but when you do enough studies you get a few positive results and that keeps the field alive.” Hmmm! I suppose that same logic applies to statins, Dr. Sampson. A few positive results achieved via industry-funded studies have kept statin drugs on the shelves, to the tune of $14 billion annually in profits for the drug companies in spite of overwhelming evidence that they’re next to useless.
Likewise, Dr. Elsa-Grace Giardina, a cardiologist at Columbia University, advises her patients to completely avoid herbal remedies. “Frankly, I would just avoid them all,” she says. “Go into your medicine cabinet and get rid of anything you bought in an herbal store that you take in a pill form. Save your money and go buy a pair of shoes.”
The press, as usual, has jumped all over the report reminding the public that herbal medications aren’t regulated by the FDA, rendering them unsafe, impure, and unreliable (unlike prescription medications, which reliably kill over 100,000 patients annually in the U.S. alone). “The public believes there is a check on everything, which is not true at all,” says Dr. Jahangir, reiterating the unregulated herbals warning. (But again, ignoring the fact that the FDA’s so-called careful regulation of prescription medications has done nothing to prevent them from becoming the fourth leading cause of death in the U.S.)
But in fairness, Dr. Jahangir does bring up some good points. For one thing, he notes that patients turn to herbals because, “Consumers of these products think they are not getting proper attention from their physicians. The typical hands-on communication between physician and patient is getting compromised, and they are seeking that type of relationship.”
And that’s true — such a lack of communication leads to problems like taking bad combinations of medicines and herbs. On the other hand, patients also turn to herbals because they’ve caught wind of the fact that pharmaceuticals are neither fail-proof nor safe. They believe, wisely, that herbals (at least if you get good quality products) in fact are safer, and in many cases, just as effective — and sometimes even more effective — than pharmaceuticals. They want the best of both worlds and simply don’t recognize that herbals and pharmaceuticals don’t necessarily mix.
Dr. Jahangir says that, “Anyone taking alternative medical and herbal products needs to bring it to the attention of their medical providers. Often they don’t, and physicians don’t actively seek that information.” Given that 15 million Americans use herbal remedies, and given the inherent dangers associated with pharmaceutical drugs, at least that particular piece of medical advice does indeed makes sense.
:hc








My husband’s cardiologist
My husband’s cardiologist when approached about what supplements can be taken while pt. is on Warfarin just waves his hand and says take none,as nobody needs vitamins or herbs and should “eat like doctors do: a good steak and salad every day.”…Cannot find accord anywhere, beyond some herbs to avoid. So frustrating and terrifying. Can anyone anywhere give accurate help?
Of course his cardiologist
Of course his cardiologist said no. Doctors will always say no to anything they don’t know. There’s no upside to them to say yes. If it helps, they get no credit. And if something goes wrong, they get the blame. In the future the way to ask a doctor goes something like:
“Doc, a number of people I know with similar conditions used this supplement(s) with their doctor’s permission and got spectacular results. Is it okay if I take it?”
Now the doctor has a problem. He/she still doesn’t know anything about it, but they also don’t want to look like an idiot in case it actually does help. So nine times out of ten you get a response along the lines of:
“Well, I don’t really know anything about this, but it doesn’t look like there’s anything here that can hurt you. Give it a try and we’ll monitor the results.”