In this newsletter, we’re going to talk about skin health. In our last issue, we explored the anatomy of the skin. With that as a background, we’ll now discuss the physiology of the skin…and more particularly, some of the diseases and problems commonly associated with it. In turn, we’ll explore some natural alternatives for dealing with these problems and also discuss how to optimize skin health. As a bonus, we’ll also cover the nature of aging in the skin and talk about some of the things you can do to slow that down.
Pseudo Skin Conditions
A rash is not really a skin condition. It’s a general description for any area of reddening on a person’s skin; it’s also sometimes accompanied by raised spots. Most rashes are from simple skin irritation or allergic responses. Others, though, can result from fever, illness, or other medical conditions.
- In general, the best approach for dealing with a rash is to eliminate the underlying condition, although skin crèmes or even hydrocortisone crèmes can be helpful in resolving short term conditions.
Like the word “rash,” dermatitis does not refer to a specific skin condition, but rather, is another general descriptor, but this time for inflammation of the skin.
- As with rashes, you want to deal with the underlying cause of the inflammation rather than merely applying topical ointments. That means proteolytic enzymes, omega-3 fatty acids, and immunomodulators are a good place to start.
With those general terms covered, let’s now look at some specific skin conditions and how to reverse them and achieve optimal skin health.
Seborrhea
Seborrhea (or seborrhoea) is the name given to excessively oily skin. It is caused by overactive sebaceous glands producing too much sebum, and it can affect both men and women. Its causes are generally unknown, but hormonal imbalance (either excessive estrogen or progesterone) is the most likely culprit. Although most people with seborrhea have no other health problems, it is sometimes a sign of underlying Parkinson’s disease.
- Premenopausal women are likely to benefit from progesterone crème, as estrogen dominance is a more likely problem than excessive progesterone.
- Menopausal and post-menopausal women are likely to benefit from a bio-identical estriol crème, as they are more likely to be suffering from low estrogen levels. Estriol is the gentle estrogen in the body that’s also cancer protective.
Dandruff
Dandruff is a catchall term for a common chronic scalp condition marked by itching and flaking of the skin on your scalp. Its causes can be all over the map from simple dry skin to the exact opposite–irritated oily skin, known as seborrheic dermatitis. Other causes can include localized eczema, psoriasis, and even an overgrowth of a particular yeast known as malassezia, which is found on most adult scalps, but at reduced levels.1 Clavaud C, Jourdain R, Bar-Hen A, Tichit M, et al.”Dandruff is associated with disequilibrium in the proportion of the major bacterial and fungal populations colonizing the scalp.” PLoS One. 2013;8(3):e58203. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3590157/ Malassezia overgrowth can be caused by chlorine in the shower killing off beneficial bacteria on your scalp that normally keep the malassezia in check, combined with excessive sebum in the scalp that the malassezia actually feeds on.
 Sometimes dandruff shampoos can take care of the symptoms, but not usually the underlying causes. This means that the moment you stop using the dandruff shampoo, the condition returns.
Sometimes dandruff shampoos can take care of the symptoms, but not usually the underlying causes. This means that the moment you stop using the dandruff shampoo, the condition returns.- Getting your hormones balanced with progesterone or estriol crèmes, depending on age, is a good place to start.
- Getting a good chlorine filter for your shower so you can stop killing off beneficial bacteria on your scalp that hold the malassezia in check…and on the rest of your body too, for that matter.
- Supplementing with a good proteolytic enzyme formula and omega-3 fatty acids to control systemic inflammation can be useful.
- Using immunomodulators such as L-carnosine, CMO, and colostrums to control overactive immune systems as seen in eczema and psoriasis is also probably a good idea.
Acne
Acne is actually the most common skin condition, affecting over 85% of people at some point in their lives. It is related to seborrhea and dandruff in that overactive sebaceous glands play a major role… along with bacteria that live on the skin’s surface. Acne occurs when hair follicles become plugged with excess sebum and dead skin cells. This plug provides a perfect environment for bacteria to set up camp and multiply. If the plug causes the follicle wall to bulge, it produces a whitehead. If the plug opens to the skins surface, it often darkens, producing what is appropriately termed a blackhead. Pimples, on the other hand, develop when blocked hair follicles become inflamed or infected. Recent research has actually identified the bacteria involved.2 Fitz-Gibbon S, Tomida S, Chiu BH, Nguyen L, Craft N, et al. “Propionibacterium acnes Strain Populations in the Human Skin Microbiome Associated with Acne.” J Invest Dermatol. 2013 Jan 21. http://www.ncbi.nlm.nih.gov/pubmed/23337890 Inside the oily depth of the subjects’ pores, the researchers found two strains of bacteria called Propionibacterium or P. acnes. They found bad strains of the bacteria in the acne patients and good strains in healthy patients. They even identified a third strain that apparently protects the skin from acne.
Primary triggers for acne are the sex hormones, which tell your oil glands to “pump up the jam” so to speak and stress. Not surprisingly, then, acne tends to be most problematic during the teenage years and during pregnancy, when androgenic hormones and stress are raging. So, until new miracle products are developed from the Propionibacterium research, you might want to take some immediate steps.
- Keep your skin clean.
- Avoid chlorinated water as it kills off the entire microbiome on the face, leaving an open environment for bad bacteria to colonize.
- Use immune boosters and pathogen destroyers internally to help control the bad bacteria systemically.
- Supplement with real vitamin A and zinc to help the body resist infection and inflammation.
- Supplement with Omega-3 fatty acids for their antibacterial and anti-inflammatory effects.
- Use probiotics to rebuild intestinal bacteria, particularly if you’ve been on any antibiotics or if you drink chlorinated water.
- Take up meditation or some similar activity to reduce stress.
- And use an all natural progesterone crème (men’s or women’s) to help balance out at least some of the hormonal issues that are most often the root of acne problems.
- Note: adult acne can be triggered by food allergies, most notably dairy.
Rosacea
Rosacea is a common age-old skin disorder with multiple clinical variants. Symptoms include acne-like pimples, exaggerated facial flushing, and persistent redness along with enlarged blood vessels and (sometimes) oil glands.
Last year, research confirmed what many alternative healers have known for years–that the most likely culprit for rosacea is a skin mite, Demodex folliculorum–or more specifically, a bacterium found inside it.3 Jarmuda S, O’Reilly N, Zaba R, Jakubowicz O, et al. “Potential role of Demodex mites and bacteria in the induction of rosacea.”J Med Microbiol. 2012 Nov;61(Pt 11):1504-10. http://www.ncbi.nlm.nih.gov/pubmed/22933353 For years, dermatologists have danced around this fact when they noted that patients with rosacea often improved when given oral antibiotics such as doxycycline and topical antibiotics such as metronidazole. But until this year, a causal link between bacteria and rosacea had never been conclusively established. Because of this, many medical experts had attributed the rosacea improving effects of antibiotics to their anti-inflammatory properties.
But in research published last year, and as reported in our blog, the bacterium, Bacillus oleronius, was identified within the gut of the common skin mite Demodex folliculorum. These mites are generally much more numerous in rosacea sufferers. Because these mites build up all their metabolic waste internally, without the benefits of defecation (talk about constipated), the levels of this bacterium in older, engorged and dying mites are typically very high. When the mites die, their resident bacteria remain in the skin pores and appear to stimulate an immune response within the skin that clinically manifests as rosacea. The antibiotics that are effective against Bacillus oleronius are associated with improvement in rosacea symptoms. Armed with this information, we can recommend:
- Cleaning the face with Chang Sheng Herbal Rejuvenating Soap, or an equivalent, which has been used successfully for over 30 years to dramatically reduce Demodex populations on the skin.4 http://www.amazon.com/Chang-Sheng-Herbal-Rejuvenating-Beauty/dp/B005VTZZUA/ref=sr_1_1?ie=UTF8&qid=1372303798&sr=8-1&keywords=Chang+Sheng+Herbal+Rejuvenating+Soap
- Avoiding chlorinated water when washing the face so as not to wipe out the beneficial bacteria which would normally compete with B. oleronius.
- Progesterone crème to reduce the production of excess sebum, which the mites thrive on.
- Systemic immune boosters and pathogen destroyers that ultimately make their way to the skin to help control the B. oleronius.
Warts
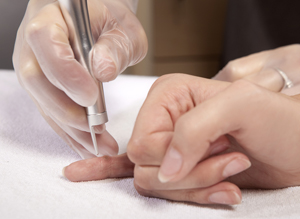 A virus infects the skin and causes the skin to grow excessively, creating a wart. Or to put it another way, a wart is a hard benign growth on the skin caused by a virus. Warts may be treated at home with salicylic acid solutions (but that’s only moderately effective), freezing (quite effective if you’re persistent), or removed by a physician. Personally, I’m not so big on the popular duct tape approach, which supposedly works by irritating the skin. In reality, it doesn’t seem to work as well as advertised–and in fact, studies have confirmed as much.5 Wenner R, Askari SK, Cham PM, Kedrowski DA, Liu A, Warshaw EM. “Duct tape for the treatment of common warts in adults: a double-blind randomized controlled trial.” Arch Dermatol. 2007 Mar;143(3):309-13. http://www.ncbi.nlm.nih.gov/pubmed/17372095
A virus infects the skin and causes the skin to grow excessively, creating a wart. Or to put it another way, a wart is a hard benign growth on the skin caused by a virus. Warts may be treated at home with salicylic acid solutions (but that’s only moderately effective), freezing (quite effective if you’re persistent), or removed by a physician. Personally, I’m not so big on the popular duct tape approach, which supposedly works by irritating the skin. In reality, it doesn’t seem to work as well as advertised–and in fact, studies have confirmed as much.5 Wenner R, Askari SK, Cham PM, Kedrowski DA, Liu A, Warshaw EM. “Duct tape for the treatment of common warts in adults: a double-blind randomized controlled trial.” Arch Dermatol. 2007 Mar;143(3):309-13. http://www.ncbi.nlm.nih.gov/pubmed/17372095
Repeatedly, applying a band aid soaked in a strong antiviral pathogen destroyer overnight can also remove a wart in a few days. And the same trick done with an essential oil blend made from various cedar oils, melaleuca, and lavender oil can also be effective.
Skin Tags
Skin tags affect almost half the population. They are small flaps of benign tissue that hang off the surface of the skin in places like the face, neck, chest, back, armpits and groin area. They commonly occur after midlife. As to what causes them, there are several theories. According to some experts, they are caused by bunches of collagen and blood vessels which are trapped inside thicker bits of skin, which themselves are believed to be the result of skin rubbing against skin. That is why they are generally found in skin creases and folds. Obesity is also associated with skin tags, which lends further support to the rubbing theory. On the other hand, diabetes is a known risk factor, leading some to suspect that insulin resistance plays a role. Additional risk factors include:
- Pregnancy, most likely because of hormonal changes.
- Herpes HPV 6 and HPV 11.
- Illegal steroid use, which can cause the collagen fibers in the skin to bond, allowing skin tags to be formed.
- And there may be a genetic component, as it tends to appear in families. Then again, families usually share the same lifestyle and many of the same dietary habits.
Standard medical treatments include.
- Removal with a scalpel or medical scissors
- Freezing or burning them off
- Laser surgery
- Topical medications
More natural treatments include:
- Cutting off the blood supply, depending on size and location, using rubber bands or dental floss to tie off the tag at its base.
- Natural topical treatments include:
- Apple cider vinegar. Soak the pad of a band aid with Bragg’s Apple Cider Vinegar, or an equivalent. Then apply the bandage over the tag and leave on overnight. Repeat each night. The tag usually peels off in 10-14 days. This is the same idea as in the wart treatment described earlier.
- There’s a commercial natural product sold in many pharmacies called Tag Away that uses oil from an evergreen tree to achieve the same result.
- An essential oil based on the same ingredients as the wart formula we talked about above can also help.
- And since insulin resistance is a suspected factor in the development of skin tags, taking a sugar metabolic enhancement formula 10 minutes before each meal–especially any meal or snack that contains high glycemic carbs– makes sense.
Eczema
Eczema is a form of dermatitis (inflammation of the epidermis) that causes an itchy rash. The word itself comes from the Greek word for “boil over,” which is somewhat descriptive of an eczema rash, which is characterized by dry, red, flaking skin, inflammation, and in more severe cases, even blistering, cracking, oozing, and sometimes bleeding. The actual cause is unknown, but is likely the result of multiple factors all coming together. Leaving eczema caused by an allergic response–which is more accurately covered under the contact dermatitis label–out of the discussion, contributing factors probably include:
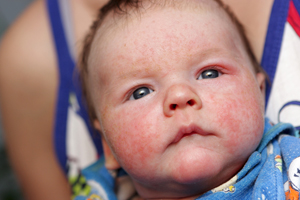 Aging and newborns.
Aging and newborns.- Genetic predisposition.
- Poor circulation in the limbs–and thus the skin covering those limbs.
- Dry weather.
- An overactive immune system
Common pharmaceutical treatments include prednisone, betamethasone, and antibiotics (for their anti-inflammatory properties)–all of which have significant side effects. If possible, it’s best to deal with eczema naturally. That means that no matter what the trigger (an environmental factor, an allergic reaction to dust mite excrement, or internal physiological factor), eczema ultimately depends on an overactive response from your immune system leading to inflammation and redness. That would suggest that any treatment for eczema should include:
- The use of immunomodulators such as L-carnosine, CMO, and colostrums to control an overactive immune system.
- Supplementing with proteolytic enzymes and omega-3 fatty acids to control systemic inflammation.
- Dealing with the trigger, whether it be improving vitamin circulation, using a humidifier in the house, or using dust mite covers on your bed–assuming you can figure out what the trigger is.
Psoriasis
Psoriasis is defined as a non-contagious inflammatory skin disease characterized by recurring reddish patches covered with silvery scales. The word comes from the Greek word for itch. It is a common skin condition that affects the life cycle of skin cells. Psoriasis causes cells to build up rapidly on the surface of the skin, forming thick silvery scales and itchy, dry, red patches that are sometimes painful. Psoriasis is a chronic, long-lasting (usually lifelong) condition. You may have periods when your psoriasis symptoms improve or go into remission alternating with times your psoriasis worsens. For some people, psoriasis is just a nuisance. For others, it’s disabling, especially when associated with arthritis (psoriatic arthritis). It has also been linked to an increased risk of heart attack, stroke,6 Armstrong EJ, Harskamp CT, Armstrong AW. “Psoriasis and major adverse cardiovascular events: a systematic review and meta-analysis of observational studies.” J Am Heart Assoc. 2013 Apr 4;2(2):e000062. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3647278/ and even a 56% higher risk of cancers.7 Charlene Laino “Psoriasis Linked to Heart Disease, Cancer.” WebMD March 15, 2010. (Accessed 26 June 2013.) http://www.webmd.com/skin-problems-and-treatments/psoriasis/news/20100315/psoriasis-linked-to-heart-disease-cancer There’s no medical cure, but psoriasis “treatments” may offer significant relief. Lifestyle measures, such as using a nonprescription cortisone cream and exposing your skin to small amounts of natural sunlight, can improve your psoriasis symptoms. (But be careful of the cortisone crèmes. Withdrawal of topical steroid cream can aggravate psoriasis due to the ‘rebound effect’ associated with corticosteroids.) And recent studies have found that losing weight can also dramatically reduce the level of symptoms. Note: hardcore pharmaceutical drugs for psoriasis are not necessarily that effective and can be quite dangerous.
Psoriasis does appear to have a genetic component, as it tends to run in families. But it is ultimately an immune system mediated disease, driven more by an overactive immune system than anything else. Natural approaches for dealing with psoriasis, then, include:
- Full body detox to clean out any possible antagonists.
- Immunomodulators as described earlier to help regulate an overactive immune system.
- Systemic proteolytic enzymes to reduce any inflammation.
Shingles
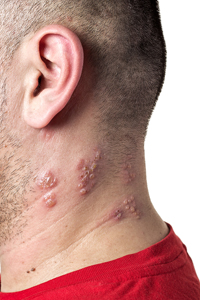 Chickenpox is a viral illness caused by the herpes zoster virus (also known as the Varicella-Zoster virus). It is a common viral infection. The problem is that after an infection, some of the virus may stay in the body, hiding out in nerve cells, lying dormant for years, and just waiting for your immune system to weaken so that the virus can become active again…causing shingles. The reason that shingles is so closely associated with aging is that aging is so closely associated with a weakened immune system.
Chickenpox is a viral illness caused by the herpes zoster virus (also known as the Varicella-Zoster virus). It is a common viral infection. The problem is that after an infection, some of the virus may stay in the body, hiding out in nerve cells, lying dormant for years, and just waiting for your immune system to weaken so that the virus can become active again…causing shingles. The reason that shingles is so closely associated with aging is that aging is so closely associated with a weakened immune system.
The easiest way to deal with shingles is not to get it–assuming you had chickenpox as a child and already have the virus in you. In other words, don’t let your immune system weaken, even as you age. Regular practice of the Baseline of Health® Program, which means regular detoxing and using supplements and natural immune boosting formulas that keep your immune system optimized, is likely to keep the virus from ever reactivating. And if you do get shingles, a topical application of the same immune boosting formula can quickly kill the active virus and dry up the sores.
Hives
Hives are raised, red, itchy patches on the skin that appear suddenly. They usually result from an allergic reaction. Treatment typically involves taking an oral antihistamine and/or using a topical steroid cream. If you get hives, those are valid treatments. But perhaps a better alternative is to reduce the chances of getting hives in the first place. This can be done by:
- Using digestive enzymes with every meal as digestive enzymes help break down many food allergens, which are almost always protein based.
- Supplementing regularly with systemic proteolytic enzymes as that helps reduce the amount of circulating immune complexes, the presence of which contributes greatly to allergic responses.
Cellulite
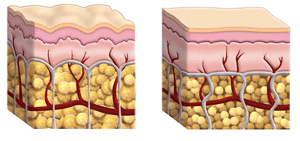 Cellulite is a condition in which the skin appears to have areas with underlying fat deposits, giving it a dimpled, lumpy appearance. It is most noticeable on the buttocks and thighs, and usually occurs after puberty. Over 80% of all women over the age of 20, regardless of their weight or size, eventually have visible cellulite. Its immediate cause is irregularly located enlarged packets of fat below the skin that push upward against the surrounding connective tissue which is there to hold that fat in place, eventually creating the visibly dimpled appearance in the skin itself. But what causes those fat pockets to appear in the first place is not so well understood; nevertheless, several theories have been put forward. Among these are:
Cellulite is a condition in which the skin appears to have areas with underlying fat deposits, giving it a dimpled, lumpy appearance. It is most noticeable on the buttocks and thighs, and usually occurs after puberty. Over 80% of all women over the age of 20, regardless of their weight or size, eventually have visible cellulite. Its immediate cause is irregularly located enlarged packets of fat below the skin that push upward against the surrounding connective tissue which is there to hold that fat in place, eventually creating the visibly dimpled appearance in the skin itself. But what causes those fat pockets to appear in the first place is not so well understood; nevertheless, several theories have been put forward. Among these are:
- Hormonal factors. Hormones likely play an important role in cellulite development. The fact that over 90% of all cellulite cases are found in women lends support to this cause. Many believe estrogen, insulin, noradrenalin, thyroid hormones, and prolactin are part of the cellulite production process.
- Genetics. Certain genes are required for cellulite development. Genes may predispose an individual to particular characteristics associated with cellulite, such as gender, race, slow metabolism, distribution of fat just underneath the skin, and circulatory insufficiency.
- Diet. People who eat too much fat, carbohydrates, or salt and too little fiber are likely to have greater amounts of cellulite.
- Lifestyle factors. Cellulite may be more prevalent in smokers, those who do not exercise, and those who sit or stand in one position for long periods of time.
- Clothing. Underwear with tight elastic across the buttocks (limiting blood flow) may contribute to the formation of cellulite.
One common misconception about treating cellulite is that liposuction can get rid of it. It can’t. Although liposuction surgically removes fat from the body, it doesn’t affect cellulite. In fact, liposuction can make the appearance of cellulite more apparent. So what options are available?
Any approach to dealing with cellulite has to deal with both components: the fat pockets and the connective tissue that holds those pockets in place.
- Eating a healthy, balanced diet and exercising are the first steps you want to take so as to reduce the fat content in cells immediately below your skin and thus reduce the appearance of cellulite.
- Full body detoxing. Toxins circulating in the blood damage both the capillaries and connective tissue surrounding the fat pockets. Regular detoxing minimizes that damage and allows the tissue an opportunity to repair itself.
- Regular use of a far infrared sauna reduces the appearance of cellulite both by stimulating the fat cells to purge their fat content and by improving circulation in the connective tissue, allowing it to become less thick and hard.8 Conrado LA, Munin E. “Reduction in body measurements after use of a garment made with synthetic fibers embedded with ceramic nanoparticles.” J Cosmet Dermatol. 2011 Mar;10(1):30-5. http://www.ncbi.nlm.nih.gov/pubmed/21332913
- As we get older, collagen production in our skin lessens, which results in an increase of wrinkles and fine lines, and decreasing smoothness and suppleness of the skin. Thinner, less supple skin also means that any cellulite you have will be more visible. Increasing collagen levels in your skin, then, can help reduce the appearance of cellulite. Collagen can’t be absorbed through the skin, so it has to be taken orally. Unfortunately, the collagen molecules in most supplements are too big to be well absorbed in the intestinal tract. So what’s the alternative?
- Supplements based on collagen peptides are one alternative as the peptides are small enough to be absorbed.
- Even better is vitamin C. Vitamin C is fundamental in every step of collagen production.9 Alexander J. Michels. “Vitamin C and Skin Health.” September 2011. OSU Linus Pauling Institute. (Accessed 1 July 2013,) http://lpi.oregonstate.edu/infocenter/skin/vitaminC/ Studies have shown that skin cells exposed to vitamin C demonstrate an eightfold increase in collagen production. Scurvy, in fact, results from a precipitous decline in collagen synthesis resulting from a lack of vitamin C. Topical vitamin C appears to be an effective route for delivering ascorbic acid to the skin if the delivery system incorporates an acidic pH. And of course, there’s always supplementation which benefits the entire body, not just the skin.
Vitiligo
Vitiligo is relatively common and is caused by the destruction or weakening of the melanocytes, resulting in the pigment or melanin being destroyed or no longer produced. Although the exact causes are unknown, in most cases, vitiligo is believed to be an autoimmune-related disorder. That said, direct damage to the skin, such as caused by excessive sun exposure or melanoma may also serve as triggers. Medical treatments are limited and include topical corticosteroids and topical pharmaceutical immunomodulators.
Given that, it makes all the sense in the world to first try:
- Natural immunomodulators, as already discussed.
- Systemic proteolytic enzymes to reduce circulating immune complexes, which are a major trigger in autoimmune disorders.
Varicose Veins, Spider Veins, Excessive Bruising
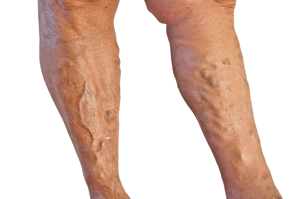
These are not actually skin issues; they’re vascular issues, but since the symptoms appear in the skin, we’ll cover them here.
The cause for all of these is essentially the same: degradation in the integrity of the small capillaries and veins just under the surface of the skin. This results in dilation, bulging, and twisting in those veins or capillaries–like a bubble on a bicycle tire. The same degradation can actually so weaken the tissue that the small vein or capillary bursts open and hemorrhages blood, which results in frequent spontaneous bruising.
Varicose veins are more common in women than in men, and may possibly have an hereditary component. More immediate triggers, however, include pregnancy, obesity, menopause, aging, prolonged standing, leg injury, and abdominal straining (i.e. constipation). But underlying it all is a degradation in the strength and integrity of the venous tissue itself. Medical treatments range from the aggressively surgical to “learn to live with it” elastic stockings. Spider veins are the capillary equivalent of varicose veins. They are common among children and pregnant women.
Spontaneous bruising is a little more complex in that there can be several causative factors, many associated with pharmaceutical medications–can you say blood thinners–or symptomatic of a more serious health condition such as cancer. Aging can also be a reason for spontaneous bruising. As we age, the layer of fat under the skin becomes thinner causing the skin to offer less protection. Capillaries under the skin also become more fragile with age and can break easily. In most cases, it is more cosmetic than serious. Note: some natural supplements, if taken in excess, can also contribute to spontaneous bruising. These include things like gingko biloba, fish oil, proteolytic enzymes, and even garlic. If that’s the case, then simply reduce your dosage.
If you want to deal with these conditions naturally, then you want to address the underlying issue–the structural integrity of the vascular system, rather than merely dealing with the symptoms as do the medical options. This would include:
- Vitamin K taken both as a supplement and applied topically. A number of studies have linked vitamin K to better vascular health10 Cranenburg E.C.M. · Vermeer C. · Koos R. · Boumans M.-L. et al. “The Circulating Inactive Form of Matrix Gla Protein (ucMGP) as a Biomarker for Cardiovascular Calcification.” J Vasc Res 2008;45:427–436. http://www.karger.com/Article/Pdf/124863 and reduced symptoms of bruising.11 Shah NS, Lazarus MC, Bugdodel R, Hsia SL, et al. “The effects of topical vitamin K on bruising after laser treatment.” J Am Acad Dermatol. 2002 Aug;47(2):241-4. http://www.ncbi.nlm.nih.gov/pubmed/12140470 Make sure you use a supplement comprised of K1 and K2–not synthetic K3. Also, do not take vitamin K if you’re on pharmaceutical blood thinners or if you’ve experienced stroke, cardiac arrest, or are prone to blood clotting.
- Horse chestnut seed extract contains a natural bioactive compound called aescin, which a number of studies have shown helps maintain blood vessel integrity.12 Montopoli M, Froldi G, Comelli MC, Prosdocimi M, Caparrotta L. “Aescin protection of human vascular endothelial cells exposed to cobalt chloride mimicked hypoxia and inflammatory stimuli.” Planta Med. 2007 Mar;73(3):285-8. Epub 2007 Feb 19. http://www.ncbi.nlm.nih.gov/pubmed/17310430
- The bioflavonoids hesperidin and diosmin, derived from citrus fruit, help prevent inflammatory responses in the vascular system. This is verified in numerous studies, including one published as recently as May of 2013.13 Belczak SQ, Sincos IR, Campos W, Beserra J, Nering G, Aun R. “Veno-active drugs for chronic venous disease: A randomized, double-blind, placebo-controlled parallel-design trial.” Phlebology. 2013 May 16. http://www.ncbi.nlm.nih.gov/pubmed/23761871
- Full spectrum antioxidant. When it comes to antioxidants, it’s not just the bioflavonoids; the proanthocyanidins, particularly the OPCs as found in grape seed extract and pcynogenol, also play a major role in supporting vascular health.14 Okudan N, Bariskaner H, Gökbel H, Sahin AS, Belviranli M, Baysal H. “The effect of supplementation of grape seed proanthocyanidin extract on vascular dysfunction in experimental diabetes.” J Med Food. 2011 Nov;14(11):1298-302. http://www.ncbi.nlm.nih.gov/pubmed/21663473 ,15 Wang L, Zhu LH, Jiang H, Tang QZ, Yan L, et al. “Grape seed proanthocyanidins attenuate vascular smooth muscle cell proliferation via blocking phosphatidylinositol 3-kinase-dependent signaling pathways.” J Cell Physiol. 2010 Jun;223(3):713-26. http://www.ncbi.nlm.nih.gov/pubmed/20175116 And recent studies have shown that resveratrol plays a role in reducing oxidative stress and inflammation in your vascular system.16 Zhang J, Chen J, Yang J, Xu CW, Pu P, Ding JW, Jiang H. “Resveratrol attenuates oxidative stress induced by balloon injury in the rat carotid artery through actions on the ERK1/2 and NF-kappa B pathway.” Cell Physiol Biochem. 2013;31(2-3):230-41. http://www.ncbi.nlm.nih.gov/pubmed/23428596
- Heavy metal detoxes can remove a major factor that, if left in place, will produce negative changes in proliferation and morphology of vascular tissue. Mercury is a primary culprit, but virtually all of the heavy metals have some negative impact.17 Aguado A, Galán M, Zhenyukh O, Wiggers GA, Roque FR, et al. Mercury induces proliferation and reduces cell size in vascular smooth muscle cells through MAPK, oxidative stress and cyclooxygenase-2 pathways.” Toxicol Appl Pharmacol. 2013 Apr 15;268(2):188-200. http://www.ncbi.nlm.nih.gov/pubmed/23415682
- Systemic proteolytic enzymes. It may at first sound like a contradiction since too many proteolytic enzymes can thin the blood so much that it may trigger spontaneous bruising. But short of that level, they can play a major role in promoting vascular health. They are among the best systemic inflation reducers, and they also help break down plaque on the arterial walls, and they can even help repair scarring on the arterial walls.
Aging and Skin Health
Skin aging is a lot like the aging of the other organs in your body, with one exception: you can see it. And like the other organs, the causes are similar and cumulative. Factors that influence the aging of your skin, and which you’ll want to address, include:
Protein Degradation
Glycation is the uncontrolled reaction of sugars with proteins. It’s kind of like what happens to sugars when you heat them and they caramelize. In effect, glycation is what happens when excess sugars caramelize the proteins in your body. It’s a major factor in the aging process — and it’s particularly devastating to diabetics.
Your body is mostly made up of proteins, and that’s true of your skin too. In fact, proteins are the substances most responsible for the daily functioning of your body. That’s why anything that causes protein deterioration has such a dramatic impact on the body’s function and appearance. Thanks largely to the destructive effect of sugar and aldehydes, the protein in our bodies tends to undergo destructive changes as we age. This destruction is a prime factor, not only in the aging process itself, but also in the familiar signs of aging such as wrinkling skin, cataracts, and the destruction of our nervous system — particularly our brains.
Protein degradation in combination with tissue dehydration, which gets more pronounced as you age, leads to the shrinkage of all your organs over time. In your skin, this is seen as a pronounced thinning of what is already an extremely thin organ. For a moment, just think about the difference between the plump, rosy skin of a baby versus that almost ghostly, almost translucent skin of many senior citizens. That’s what shrinkage of the skin looks like. The medical term for this is “atrophy.” It is reversible.
Cellular Degradation
It’s not just proteins that degrade over time; the very cells of your body become less functional over time. Cells are the basic building blocks of all your tissues. All cells experience changes with aging. They become larger and less able to divide and multiply. Among other changes, there is an increase in pigments and fatty substances inside the cell (lipids). Many cells lose their ability to function, or they begin to function abnormally. The medical term for this is “cell senescence.” It can be slowed and even reversed.
Hormonal Changes
Hormones are your body’s chemical messenger system. They tell your body what to do and when. For example, hormones play a key role in telling your body when to store calories as fat and when to store it as muscle. They also play a key role in the thinning of skin as we age. When post menopausal women rebalance their hormones, their skin regains much of its thickness.18 Callens A, Vaillant L, Lecomte P, et al. “Does hormonal skin aging exist? A study of the influence of different hormone therapy regimens on the skin of postmenopausal women using non-invasive measurement techniques.” Dermatology. 1996;193(4):289-94. http://www.ncbi.nlm.nih.gov/pubmed/8993951 Fortunately, this can be done naturally, but it involves more than just estrogen. We’re talking about rebalancing estrogen, progesterone, testosterone, and human growth hormone.
Damage
Much of skin damage is self inflicted. Sun exposure is essential for good health, but too much at the wrong time of day severely damages the skin. Then there’s smoking, which is one of the worst things you can do for your skin. It has been observed that the skin of smoking addicts at the age of 40 years resembles the skin of non-smoking 70 year old adults.19 Urbanska M, Nowak G, Florek E. “[Cigarette smoking and its influence on skin aging]. [Article in Polish]” Przegl Lek. 2012;69(10):1111-4. http://www.ncbi.nlm.nih.gov/pubmed/23421102 And unfortunately, skin damage due to tobacco smoke is irreversible. The primary damage from cigarette smoking comes from free radical damage. That means that although you cannot reverse damage caused by smoking, you can significantly inhibit it if you are using a full spectrum antioxidant during the years that you do smoke. N-acetyl-cysteine in particular helps protect against the free radicals that are produced through cigarette smoke.
 It’s probably worth noting that in addition to cigarette smoke, other sources of free radicals that can harm the skin include air pollution, smog, soot, automobile exhaust, toxic waste, pesticides, herbicides, background radiation, drugs, and even certain foods. And even stress is likely a factor in the aging of your skin. Stress has been shown to correlate with shorter telomeres, which are caps that protect the ends of chromosomes. When the telomeres are gone, chromosomes begin to fall apart, which leads to cell damage and diseases associated with aging. Stress also increases free radical oxidation and glycation, which, as we’ve already discussed, lead to a more aged skin appearance.
It’s probably worth noting that in addition to cigarette smoke, other sources of free radicals that can harm the skin include air pollution, smog, soot, automobile exhaust, toxic waste, pesticides, herbicides, background radiation, drugs, and even certain foods. And even stress is likely a factor in the aging of your skin. Stress has been shown to correlate with shorter telomeres, which are caps that protect the ends of chromosomes. When the telomeres are gone, chromosomes begin to fall apart, which leads to cell damage and diseases associated with aging. Stress also increases free radical oxidation and glycation, which, as we’ve already discussed, lead to a more aged skin appearance.
You also might want to cut back on your alcohol consumption. Depending on how much you drink, alcohol can contribute significantly to an aged appearance by dilating small blood vessels in the skin and increasing blood flow near the skin’s surface. Over time, these blood vessels continue to grow and enlarge, eventually leading to the destruction of collagen, a loss of skin tone, and permanent redness and blotchiness. Also, the continued dilation of blood vessels can lead over time to broken blood vessels near the surface of the skin, especially around the nose and face. And finally, alcohol is very dehydrating. Regular consumption can literally dry out your skin, again over time.
Conclusion
Which brings us to the question of the day: what steps should we take to slow down, and even reverse the appearance of aging in our skin? In fact, we’ve already explored most of the steps you can take over the last two newsletters, so now we can just summarize.
- You need to hydrate sufficiently by drinking lots of water and consuming fewer diuretics such as coffee.
- Assist your microbiome by washing your skin (especially your hands) regularly with soap and water, but do not use antibacterial soap. In addition to being toxic, it destroys your microbiome, which leaves you far more vulnerable to aggressive pathogens living on your skin. You also might want to think about putting a chlorine filter on your showerhead so as not to totally destroy those trillion beneficial bacteria living on your skin.
- Use a carnosine based supplement to slow down cell senescence and minimize protein degradation. I’ve been using variations of my own carnosine formulas for almost 20 years. My younger sister now introduces me as “her younger brother” to avoid the inevitable questions. It really does work.
- Use a full spectrum antioxidant. Make sure it contains resveratrol, which can reduce skin cancer tumors by 98% and stop the production of leukemia cells20 Moon SO, Kim W, Sung MJ, Lee S, Kang KP, et al. “Resveratrol suppresses tumor necrosis factor-alpha-induced fractalkine expression in endothelial cells.”Mol Pharmacol. 2006 Jul;70(1):112-9. http://molpharm.aspetjournals.org/content/70/1/112.long –in addition to slowing down the aging process.21 Baur JA, Pearson KJ, Price NL, Jamieson HA, et al. “Resveratrol improves health and survival of mice on a high-calorie diet.” Nature. 2006 Nov 16;444(7117):337-42. http://www.ncbi.nlm.nih.gov/pubmed/17086191 You’ll also want your formula to contain OPC grape seed extract, which can revive declining capillary activity by up to 140% as well as repair varicose veins and prevent bruising.22 Robert L, Godeau G, Gavignet-Jeannin C, Groult N, Six C, Robert AM. “[The effect of procyanidolic oligomers on vascular permeability. A study using quantitative morphology]. [Article in French]” Pathol Biol (Paris). 1990 Jun;38(6):608-16. http://www.ncbi.nlm.nih.gov/pubmed/2165237
- Supplement with 4-10 mg of astaxanthin a day. Astaxanthin has not only been proven to protect your skin from the sun (it actually works as an internal sun screen) and reduce the signs of aging, but it has also been shown to profoundly suppress cancerous mutations in skin cells.23 Rao AR, Sindhuja HN, Dharmesh SM, Set al. “Effective Inhibition of Skin Cancer, Tyrosinase, and Antioxidative Properties by Astaxanthin and Astaxanthin Esters from the Green Alga Haematococcus pluvialis.” J Agric Food Chem. 2013 Apr 16. http://www.ncbi.nlm.nih.gov/pubmed/23473626
- Supplement with systemic proteolytic enzymes and omega-3 fatty acids to reduce inflammation throughout the body, including the skin.
- Regular full body detoxing since toxins affect all organs, including your skin.
- Use a progesterone crème to balance out excess estrogen levels.
- Use a formula to free up bound testoserone.
- During and after menopause, you may want to use an all natural estriol crème to rebalance declining estrogen levels.
- Use an HGH secretagogue to help reestablish growth hormone levels in your body. Although not as powerful as HGH injections, these formulas can be quite effective (provided your pituitary is still functioning) and carry none of the downside of injections. The key ingredients in these formulas tend to be arginine (an essential amino acid) and GABA.24 http://secretagoguegold.com/
- Collagen is a complex structural protein that maintains strength and flexibility throughout the body and especially the skin. Collagen levels in your skin decline as you age. Unfortunately, collagen molecules are so large and complex that they won’t penetrate the outer layers of the skin so topical application is useless, and they don’t readily pass through the walls of the digestive tract so supplementation is only marginally useful. Fortunately, you can now find supplements made from collagen peptides. The peptides are made by hydrolyzing (or breaking down) the large collagen molecules into smaller, low molecular weight molecules that can actually be absorbed and utilized by the body.
- Hyaluronic acid (HA) is your skin’s ultimate hydrating agent. It is primarily found in the papillary layer of your dermis, filling the spaces between the collagen fibers as part of a thick gel comprised of water, protein complexes, and hyaluronic acid. HA attracts and holds 1,000 times its own weight in water, which is what plumps your skin so that wrinkles and lines are less visible. This jelly-like complex transports essential nutrients from the bloodstream, via the capillaries in your skin. Supplementing with HA can boost moisture levels and minimize the appearance of fine lines and wrinkles.
- Na-PCA is of the sodium salt of pyrrolidone carboxylic acid. It is a natural moisturizing factor found in human skin. It is available from a number of sources as a concentrate pH balanced solution that, when sprayed on the skin, works as a humectant that helps to increase the skin’s moisture level.
- Mild facial scrubs help remove old dead skin cells from the surface of the skin making it easier for new cells to make their way up. This is especially important as you age, since the whole process of shedding old skin slows down. Versions are made for both men and women.
- And for goodness sake, stop furrowing your brow. Or as your mother always told you, “Stop making that face or it will become permanent.”
A Note on Retinoids and Skin Health
Retinoic acid, or tretinoin, is an anti-aging ingredient derived from vitamin A that is found in prescription only skin crèmes. Retinol is the less potent non prescription form. It works because skin cells have retinoid receptors that when activated help aging skin cells behave more like younger cells. When used regularly, retinoids help skin cells turn over more rapidly, which helps to fade dark spots and freckles, improve skin texture, and shrink dilated pores. But most importantly, it both helps increase the production of collagen in your skin and inhibits its breakdown as a result of sun damage.
There are, however, some problems with using retinoids. First, for up to two months, it can make your skin look much worse–red, flaky, and peeling. Second, it makes your skin very sensitive to the sun, which means you have to use a high SPF sunscreen or even avoid the daylight altogether, which gives you something in common with vampires. Third, the FDA’s National Center for Toxicological Research and the National Toxicology Program have conducted a series of studies that suggest a possible link between skin cancer and the use of natural retinoids in skin care products and sunscreen.25 “NTP Technical Report on the Photococarcinogenesis Study of Retinoic Acid and Retinyl Palmitate.” NIH January 26, 2011. (Accessed 4 July 2013.) http://ntp.niehs.nih.gov/ntp/about_ntp/trpanel/2011/january/drafttr568.pdf That can’t be good. And finally retinoids tend to work much better on skin that has aged prematurely as a result of sun damage than on skin that has avoided sun damage. In fact, where sun damage is not a factor the benefit is almost non-existent. And finally, there is some very tenuous evidence that it may cause birth defects, but that evidence probably doesn’t stand up to scrutiny.
Nevertheless, four out of five negatives–especially the connection to skin cancer–is probably reason enough not to go down this route. That said, in a bit of marvelous irony, topical retinoids are the only treatment authorized by the FDA for warding off the signs of aging in your skin. Perhaps it has something to do with the fact that many dermatologists view topical retinoids as the cornerstone of their anti-aging treatment for skin. And when doctors talk, the FDA dances.
A Note on Topical Skin Crèmes and Skin Health
When it comes to skin care products, there is a game that is played with governmental regulators. Theoretically, no topical skin crème can penetrate below the epidermis, or it is considered a drug. Why? Because if anything reaches the dermis or the subcutis, it has access to the vascular network and can be picked up and transported anywhere in the body. There is a scene in the movie The Jackal with Bruce Willis in which Bruce is being chased by bad guys and he sprays something on the door handle of his car before abandoning it. Not long after, one of the bad guys finds the car and touches the door handle trying to get into the car. Suddenly, he reaches up and grabs his throat gagging and falls over dead…poisoned.
That’s actually feasible, although not quite as quickly as in the movie. Although, as we discussed in our last newsletter when exploring the anatomy of the skin, the outer layers of the skin are largely impervious, they are not totally so — and given the use of the right solvent, you can carry almost anything into the lower layers of the skin.
To be sure, most skin crèmes do not penetrate. They sit on the surface of the skin only to be washed off later in the day. But some in fact do penetrate, they just can’t tell you about it. They use euphemisms instead, like “deep healing,” “skin deep,” or “deep moisturizing.” Unfortunately, the useless crèmes also can make the same marketing fluff claims, so you never know. When you do find one that works–that really penetrates–keep it secret, and use it as long as you can before it’s pulled from the market.
———
For more on aging in general check out: https://www.jonbarron.org/article/nature-aging-part-1
And with that, let me leave you with the words of the immortal Billy Crystal,

“It’s better to look good than to feel good.”
And if you make use of what you learned in this newsletter, you should “look marvelous.”
References
| ↑1 | Clavaud C, Jourdain R, Bar-Hen A, Tichit M, et al.”Dandruff is associated with disequilibrium in the proportion of the major bacterial and fungal populations colonizing the scalp.” PLoS One. 2013;8(3):e58203. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3590157/ |
|---|---|
| ↑2 | Fitz-Gibbon S, Tomida S, Chiu BH, Nguyen L, Craft N, et al. “Propionibacterium acnes Strain Populations in the Human Skin Microbiome Associated with Acne.” J Invest Dermatol. 2013 Jan 21. http://www.ncbi.nlm.nih.gov/pubmed/23337890 |
| ↑3 | Jarmuda S, O’Reilly N, Zaba R, Jakubowicz O, et al. “Potential role of Demodex mites and bacteria in the induction of rosacea.”J Med Microbiol. 2012 Nov;61(Pt 11):1504-10. http://www.ncbi.nlm.nih.gov/pubmed/22933353 |
| ↑4 | http://www.amazon.com/Chang-Sheng-Herbal-Rejuvenating-Beauty/dp/B005VTZZUA/ref=sr_1_1?ie=UTF8&qid=1372303798&sr=8-1&keywords=Chang+Sheng+Herbal+Rejuvenating+Soap |
| ↑5 | Wenner R, Askari SK, Cham PM, Kedrowski DA, Liu A, Warshaw EM. “Duct tape for the treatment of common warts in adults: a double-blind randomized controlled trial.” Arch Dermatol. 2007 Mar;143(3):309-13. http://www.ncbi.nlm.nih.gov/pubmed/17372095 |
| ↑6 | Armstrong EJ, Harskamp CT, Armstrong AW. “Psoriasis and major adverse cardiovascular events: a systematic review and meta-analysis of observational studies.” J Am Heart Assoc. 2013 Apr 4;2(2):e000062. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3647278/ |
| ↑7 | Charlene Laino “Psoriasis Linked to Heart Disease, Cancer.” WebMD March 15, 2010. (Accessed 26 June 2013.) http://www.webmd.com/skin-problems-and-treatments/psoriasis/news/20100315/psoriasis-linked-to-heart-disease-cancer |
| ↑8 | Conrado LA, Munin E. “Reduction in body measurements after use of a garment made with synthetic fibers embedded with ceramic nanoparticles.” J Cosmet Dermatol. 2011 Mar;10(1):30-5. http://www.ncbi.nlm.nih.gov/pubmed/21332913 |
| ↑9 | Alexander J. Michels. “Vitamin C and Skin Health.” September 2011. OSU Linus Pauling Institute. (Accessed 1 July 2013,) http://lpi.oregonstate.edu/infocenter/skin/vitaminC/ |
| ↑10 | Cranenburg E.C.M. · Vermeer C. · Koos R. · Boumans M.-L. et al. “The Circulating Inactive Form of Matrix Gla Protein (ucMGP) as a Biomarker for Cardiovascular Calcification.” J Vasc Res 2008;45:427–436. http://www.karger.com/Article/Pdf/124863 |
| ↑11 | Shah NS, Lazarus MC, Bugdodel R, Hsia SL, et al. “The effects of topical vitamin K on bruising after laser treatment.” J Am Acad Dermatol. 2002 Aug;47(2):241-4. http://www.ncbi.nlm.nih.gov/pubmed/12140470 |
| ↑12 | Montopoli M, Froldi G, Comelli MC, Prosdocimi M, Caparrotta L. “Aescin protection of human vascular endothelial cells exposed to cobalt chloride mimicked hypoxia and inflammatory stimuli.” Planta Med. 2007 Mar;73(3):285-8. Epub 2007 Feb 19. http://www.ncbi.nlm.nih.gov/pubmed/17310430 |
| ↑13 | Belczak SQ, Sincos IR, Campos W, Beserra J, Nering G, Aun R. “Veno-active drugs for chronic venous disease: A randomized, double-blind, placebo-controlled parallel-design trial.” Phlebology. 2013 May 16. http://www.ncbi.nlm.nih.gov/pubmed/23761871 |
| ↑14 | Okudan N, Bariskaner H, Gökbel H, Sahin AS, Belviranli M, Baysal H. “The effect of supplementation of grape seed proanthocyanidin extract on vascular dysfunction in experimental diabetes.” J Med Food. 2011 Nov;14(11):1298-302. http://www.ncbi.nlm.nih.gov/pubmed/21663473 |
| ↑15 | Wang L, Zhu LH, Jiang H, Tang QZ, Yan L, et al. “Grape seed proanthocyanidins attenuate vascular smooth muscle cell proliferation via blocking phosphatidylinositol 3-kinase-dependent signaling pathways.” J Cell Physiol. 2010 Jun;223(3):713-26. http://www.ncbi.nlm.nih.gov/pubmed/20175116 |
| ↑16 | Zhang J, Chen J, Yang J, Xu CW, Pu P, Ding JW, Jiang H. “Resveratrol attenuates oxidative stress induced by balloon injury in the rat carotid artery through actions on the ERK1/2 and NF-kappa B pathway.” Cell Physiol Biochem. 2013;31(2-3):230-41. http://www.ncbi.nlm.nih.gov/pubmed/23428596 |
| ↑17 | Aguado A, Galán M, Zhenyukh O, Wiggers GA, Roque FR, et al. Mercury induces proliferation and reduces cell size in vascular smooth muscle cells through MAPK, oxidative stress and cyclooxygenase-2 pathways.” Toxicol Appl Pharmacol. 2013 Apr 15;268(2):188-200. http://www.ncbi.nlm.nih.gov/pubmed/23415682 |
| ↑18 | Callens A, Vaillant L, Lecomte P, et al. “Does hormonal skin aging exist? A study of the influence of different hormone therapy regimens on the skin of postmenopausal women using non-invasive measurement techniques.” Dermatology. 1996;193(4):289-94. http://www.ncbi.nlm.nih.gov/pubmed/8993951 |
| ↑19 | Urbanska M, Nowak G, Florek E. “[Cigarette smoking and its influence on skin aging]. [Article in Polish]” Przegl Lek. 2012;69(10):1111-4. http://www.ncbi.nlm.nih.gov/pubmed/23421102 |
| ↑20 | Moon SO, Kim W, Sung MJ, Lee S, Kang KP, et al. “Resveratrol suppresses tumor necrosis factor-alpha-induced fractalkine expression in endothelial cells.”Mol Pharmacol. 2006 Jul;70(1):112-9. http://molpharm.aspetjournals.org/content/70/1/112.long |
| ↑21 | Baur JA, Pearson KJ, Price NL, Jamieson HA, et al. “Resveratrol improves health and survival of mice on a high-calorie diet.” Nature. 2006 Nov 16;444(7117):337-42. http://www.ncbi.nlm.nih.gov/pubmed/17086191 |
| ↑22 | Robert L, Godeau G, Gavignet-Jeannin C, Groult N, Six C, Robert AM. “[The effect of procyanidolic oligomers on vascular permeability. A study using quantitative morphology]. [Article in French]” Pathol Biol (Paris). 1990 Jun;38(6):608-16. http://www.ncbi.nlm.nih.gov/pubmed/2165237 |
| ↑23 | Rao AR, Sindhuja HN, Dharmesh SM, Set al. “Effective Inhibition of Skin Cancer, Tyrosinase, and Antioxidative Properties by Astaxanthin and Astaxanthin Esters from the Green Alga Haematococcus pluvialis.” J Agric Food Chem. 2013 Apr 16. http://www.ncbi.nlm.nih.gov/pubmed/23473626 |
| ↑24 | http://secretagoguegold.com/ |
| ↑25 | “NTP Technical Report on the Photococarcinogenesis Study of Retinoic Acid and Retinyl Palmitate.” NIH January 26, 2011. (Accessed 4 July 2013.) http://ntp.niehs.nih.gov/ntp/about_ntp/trpanel/2011/january/drafttr568.pdf |












I had acne rosacea for many
I had acne rosacea for many years & tried antibiotics briefly (they gave me horrible stomach cramps) and tried the soap you mentioned. The only thing that helped was taking betaine hydrochloride and that radically reduced my symptoms. What eventually cured me was homeopathy.
Interestingly, a lot of the people I’ve met with rosacea have O negative blood type, like I do, and they’ve also been helped by betaine (which also helps with acid reflux).
This is actually very
This is actually very interesting. While it’s true that the majority of people who have tried Betaine HCL for rosacea have received no benefit, there’s no question that a notable number of people who have tried it have indeed noticed a dramatic improvement in their symptoms. Based on our understanding of what rosacea is, what could possibly be the reason? The key appears to lie in the following line from the above newsletter.
So how does a Betaine HCL supplement help with that–after all, it’s not an immunomudulator? Well, if you read my newsletter on stomach acid, you would have seen that two of the symptoms associated with low stomach acid are autoimmune disorders and skin diseases. Anything, then, that serves to correct a low acid environment in your stomach is thus likely to help moderate an overactive immune response and any resultant skin conditions—at least to some degree and for some people. And that’s what Betaine HCL does.
On the other hand, in the newsletter on stomach acid, I also mentioned that apple cider vinegar can do the same thing. If our theory is true, then we should see many of the same results from people with rosacea who supplement with ACV. And, in fact, a quick search on the internet shows that we do—and with about the same rate of success and failure as with Betaine HCL.
So, the bottom line is that, yes, betaine HCL may indeed be helpful for some people with rosacea. And more importantly, since a positive response to Betaine HCL would likely mean that someone had been suffering from low stomach acid in the first place, supplementation would likely help with any of the other symptoms associated with low stomach acid that someone might likely be suffering from.
Thank you for this wonderful
Thank you for this wonderful article! This is the most comprehensive article I have read on natural skin health ever. I have been a health researcher and practitioner for a long time. One questions I have for that I did not see addressed in this article: how do we treat moles?
Assuming the moles are non-malignant would the treatment for moles be similar to the treatment for warts (applying a bandage with a strong anti-viral formula)? I’d be interested in all your recommendations.
Warts and moles are very
Warts and moles are very different. Warts are viral. Moles are nevi, which are similar to skin tags. And benign moles can be removed in natural ways, similar to skin tags. Products such as DermaTend can be quite effective. However, before using any treatment on a mole, it’s imperative that you determine that it’s benign, not cancerous.
Re varicose ,spider veins and
Re varicose ,spider veins and thrombosis :
Do you produce or recommend a combined supplement which is effective in treating the above please?
Did you see the list of
Did you see the list of supplements Jon Barron provides in this newsletter under this section? I would start there.
What can be done about
What can be done about lessening the appearance of scars – or making them disappear completely?
For lessening the appearance
For lessening the appearance of established external scars, a topical scar gel like Kelo-cote may be helpful.
Hello,
Hello,
Thanks for nice article. Could you please help me to find more information on Chang Sheng Herbal Rejuvenating Soap? I searched the web for long time but only found few reviews on Amazon but your article saiz that the soap has been used for 30 years. I am interested in list of ingredients especial after reading some articles that steroids were found in some chinese ‘natural’ creams. Please could you provide links to research of guide me to the source of trustworthy information? Thanks, Eva
You can try to contact them
You can try to contact them directly with any questions you may have. http://changshengsoap.com/
Hi,
Hi,
I have tied Chang Sheng Herbal rejuvenating soap and I have noticed that every time I use it , my skin turns horribly red , rough , bumpy, and itchy on my cheeks and forehead. I used to use it before and stopped after a while . And I was starting to get acne and I thought I should use it so my acne doesnt worsen. But It got really bad . I am not sure if I am allergic to the soap , or there is any other plausible cause for this.
Thanks,
Jyo
You could be allergic. I
You could be allergic. I would contact them directly with any questions you may have. http://Changshengsoap.com/
HI,
HI,
THANK YOU SO MUCH, I LOVE ALL YOUR ARTICLES -VERY HELPFUL! I HAVE A FULL BUNCH OF PROBLEMS
ONE OF THEM IS ICHTHYOSIS AND WINTER EKSEMA USUALLY ON THE STOMACH BUT THIS YEAR IT’S SPREADING ALL OVER. STEROIDS OINTMENT HELPS WITH ITCHING BUT NEW ONES KEEP FORMING. I REFUSE TO TRY ELIDEL . FOR ICHTHYOSIS MY DOC GAVE ME ALMACTIN 12% WHICH IS VERY HELPFUL BUT IS IT SAFE TO USE IT FOR LONG, LIKE DOC. SAID FOR THE REST OF MY LIFE?
The article is really
The article is really wonderful. I gained more knowledge about skin diseases and how to manage it. I need to know whether any skin care products are available for anti aging.Thank you for posting the wonderful article.
“This is a topic that’s near
“This is a topic that’s near to my heart… Thank you!
Exactly where are your contact details though?”
Great article, nicely
Great article, nicely explained without the usual FUD. Yes, it you can find some scary stuff, you can also find some very thought provoking stuff. If you do happen to land on a site that you find morally corrupt (illegal, pornographic or both) don’t hang around there! Close your browser or navigate away.